

Anantiseptic (Greek: ἀντί, romanized: anti, lit. 'against'[1] and σηπτικός, sēptikos, 'putrefactive'[2]) is an antimicrobial substance or compound that is applied to living tissue to reduce the possibility of sepsis, infectionorputrefaction. Antiseptics are generally distinguished from antibiotics by the latter's ability to safely destroy bacteria within the body, and from disinfectants, which destroy microorganisms found on non-living objects.[3]
Antibacterials include antiseptics that have the proven ability to act against bacteria. Microbicides which destroy virus particles are called viricidesorantivirals. Antifungals, also known as antimycotics, are pharmaceutical fungicides used to treat and prevent mycosis (fungal infection).[4]

The widespread introduction of antiseptic surgical methods was initiated by the publishing of the paper Antiseptic Principle of the Practice of Surgery in 1867 by Joseph Lister, which was inspired by Louis Pasteur's germ theory of putrefaction.[5][6] In this paper, Lister advocated the use of carbolic acid (phenol) as a method of ensuring that any germs present were killed. Some of this work was anticipated by:
Antiseptics can be subdivided into about eight classes of materials. These classes can be subdivided according to their mechanism of action: small molecules that indiscriminately react with organic compounds and kill microorganisms (peroxides, iodine, phenols) and more complex molecules that disrupt the cell walls of the bacteria.[10]
|
| |
|---|---|
| Acridine derivatives |
|
| Biguanides and amidines |
|
| Phenol and derivatives |
|
| Nitrofuran derivatives |
|
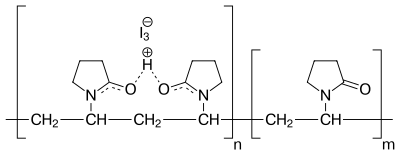
| Iodine products |
|
| Quinoline derivatives |
|
| Quaternary ammonium compounds |
|
| Mercurial products |
|
| Silver compounds |
|
| Alcohols |
|
| Other |
|
| |
| Authority control databases: National |
|
|---|