


|
Adding reference to a new study about the effectiveness and safety of coated aspirin.
Tags: Reverted Visual edit
|
→Other adverse effects: minor punctuation correction
|
||
| (46 intermediate revisions by 23 users not shown) | |||
| Line 2: | Line 2: | ||
{{for|the Persian-language TV series|Aspirin (TV series){{!}}''Aspirin'' (TV series)}} |
{{for|the Persian-language TV series|Aspirin (TV series){{!}}''Aspirin'' (TV series)}} |
||
{{distinguish|Robert Asprin}} |
{{distinguish|Robert Asprin}} |
||
{{Use dmy dates|date= |
{{Use dmy dates|date=December 2023}} |
||
{{cs1 config |
{{cs1 config|name-list-style=vanc|display-authors=6}} |
||
{{Good article}} |
{{Good article}} |
||
{{Infobox drug |
{{Infobox drug |
||
| Line 19: | Line 19: | ||
<!-- Clinical data --> |
<!-- Clinical data --> |
||
| pronounce = |
| pronounce = {{IPAc-en|ə|ˌ|s|iː|t|əl|ˌ|s|æ|l|ᵻ|ˈ|s|ɪ|l|ᵻ|k}} |
||
| tradename = [[Bayer#Aspirin|Bayer Aspirin]], others |
| tradename = [[Bayer#Aspirin|Bayer Aspirin]], others |
||
| Drugs.com = {{drugs.com|monograph|aspirin}} |
| Drugs.com = {{drugs.com|monograph|aspirin}} |
||
| MedlinePlus = a682878 |
| MedlinePlus = a682878 |
||
| licence_CA = |
|||
| licence_EU = yes |
|||
| DailyMedID = Acetylsalicylic acid |
| DailyMedID = Acetylsalicylic acid |
||
| pregnancy_AU = C |
| pregnancy_AU = C |
||
| Line 30: | Line 28: | ||
| pregnancy_category = |
| pregnancy_category = |
||
| routes_of_administration = [[Oral administration|Oral]], [[rectal administration|rectal]] |
| routes_of_administration = [[Oral administration|Oral]], [[rectal administration|rectal]] |
||
| class = |
| class = [[Nonsteroidal anti-inflammatory drug]] (NSAID) |
||
| ATCvet = |
|||
| ATC_prefix = A01 |
| ATC_prefix = A01 |
||
| ATC_suffix = AD05 |
| ATC_suffix = AD05 |
||
| Line 38: | Line 35: | ||
<!-- Legal status --> |
<!-- Legal status --> |
||
| legal_AU = OTC |
| legal_AU = OTC |
||
| legal_AU_comment = / Schedule 2, 4, 5, 6<ref>{{cite web | title=OTC medicine monograph: Aspirin tablets for oral use | website=Therapeutic Goods Administration (TGA) | date=21 June 2022 | url=https://www.tga.gov.au/resources/publication/publications/otc-medicine-monograph-aspirin-tablets-oral-use | access-date=4 April 2023}}</ref><ref>{{cite web | title=Poisons Standard October 2022 | website=Australian Government Federal Register of Legislation | url=https://www.legislation.gov.au/Series/F2022L01257 | access-date=9 January 2023}}</ref> |
| legal_AU_comment = / Schedule 2, 4, 5, 6<ref>{{cite web | title=OTC medicine monograph: Aspirin tablets for oral use | website=Therapeutic Goods Administration (TGA) | date=21 June 2022 | url=https://www.tga.gov.au/resources/publication/publications/otc-medicine-monograph-aspirin-tablets-oral-use | access-date=4 April 2023}}</ref><ref>{{cite web | title=Poisons Standard October 2022 | website=Australian Government Federal Register of Legislation | date=26 September 2022 | url=https://www.legislation.gov.au/Series/F2022L01257 | access-date=9 January 2023}}</ref> |
||
| legal_BR = <!-- OTC, A1, A2, A3, B1, B2, C1, C2, C3, C4, C5, D1, D2, E, F--> |
| legal_BR = <!-- OTC, A1, A2, A3, B1, B2, C1, C2, C3, C4, C5, D1, D2, E, F--> |
||
| legal_BR_comment = |
| legal_BR_comment = |
||
| Line 87: | Line 84: | ||
| NIAID_ChemDB = |
| NIAID_ChemDB = |
||
| PDB_ligand = AIN |
| PDB_ligand = AIN |
||
| synonyms = {{ubl|2-acetoxybenzoic acid|''o''-acetylsalicylic acid|acetylsalicylic acid|acetyl salicylate}} |
| synonyms = {{ubl|2-acetoxybenzoic acid|''o''-acetylsalicylic acid|acetylsalicylic acid|acetyl salicylate|monoacetic acid ester of salicylic acid<ref>{{cite journal|journal=Bulletin of the History of Medicine|title=What's in a Name? Aspirin and the American Medical Association|first=Jan|last=McTavish|volume=61|number=3|date=Fall 1987|url=https://www.jstor.org/stable/44442097}}</ref>}} |
||
<!-- Chemical and physical data --> |
<!-- Chemical and physical data --> |
||
| Line 118: | Line 115: | ||
One common [[adverse effect]] is an [[upset stomach]].<ref name=AHFS/> More significant side effects include [[stomach ulcer]]s, [[stomach bleeding]], and worsening [[asthma]].<ref name=AHFS/> Bleeding risk is greater among those who are older, drink [[Alcohol (drug)|alcohol]], take other NSAIDs, or are on other [[anticoagulant|blood thinners]].<ref name=AHFS/> Aspirin is not recommended in the last part of [[pregnancy]].<ref name=AHFS/> It is not generally recommended in children with [[infection]]s because of the risk of [[Reye syndrome]].<ref name=AHFS/> High doses may result in [[tinnitus|ringing in the ears]].<ref name=AHFS/> |
One common [[adverse effect]] is an [[upset stomach]].<ref name=AHFS/> More significant side effects include [[stomach ulcer]]s, [[stomach bleeding]], and worsening [[asthma]].<ref name=AHFS/> Bleeding risk is greater among those who are older, drink [[Alcohol (drug)|alcohol]], take other NSAIDs, or are on other [[anticoagulant|blood thinners]].<ref name=AHFS/> Aspirin is not recommended in the last part of [[pregnancy]].<ref name=AHFS/> It is not generally recommended in children with [[infection]]s because of the risk of [[Reye syndrome]].<ref name=AHFS/> High doses may result in [[tinnitus|ringing in the ears]].<ref name=AHFS/> |
||
A [[Precursor (chemistry)|precursor]] to aspirin found in the bark of the [[willow tree]] (genus ''Salix'') has been used for its health effects for at least 2,400 years.<ref name=Jon2015>{{cite book |vauthors = Jones A |title=Chemistry: An Introduction for Medical and Health Sciences|date=2015|publisher=John Wiley & Sons|isbn=978-0-470-09290-3|pages=5–6|url=https://books.google.com/books?id=ubE0ILq_aDQC&pg=PA6}}</ref><ref>{{cite book |vauthors = Ravina E |title=The Evolution of Drug Discovery: From Traditional Medicines to Modern Drugs |date=2011 |publisher=John Wiley & Sons |isbn=978-3-527-32669-3 |page=24 |url=https://books.google.com/books?id=iDNy0XxGqT8C&pg=PA24}}</ref> In 1853, chemist [[Charles Frédéric Gerhardt]] treated the medicine [[sodium salicylate]] with [[acetyl chloride]] to produce acetylsalicylic acid for the first time.<ref name="Jeffreys2008">{{cite book |url=https://books.google.com/books?id=a9gkBwAAQBAJ |title=Aspirin the remarkable story of a wonder drug. |vauthors=Jeffreys D |date=2008 |publisher=Bloomsbury Publishing USA |isbn=978-1-59691-816-0 |archive-url=https://web.archive.org/web/20170908213430/https://books.google.com/books?id=a9gkBwAAQBAJ |archive-date=8 September 2017 |url-status=}}{{rp|46–48}}</ref> Over the next 50 years, other chemists established the chemical structure and devised more efficient production methods.<ref name=Jeffreys2008/>{{rp|69–75}} |
A [[Precursor (chemistry)|precursor]] to aspirin found in the bark of the [[willow tree]] (genus ''Salix'') has been used for its health effects for at least 2,400 years.<ref name=Jon2015>{{cite book |vauthors = Jones A |title=Chemistry: An Introduction for Medical and Health Sciences|date=2015|publisher=John Wiley & Sons|isbn=978-0-470-09290-3|pages=5–6|url=https://books.google.com/books?id=ubE0ILq_aDQC&pg=PA6}}</ref><ref>{{cite book |vauthors = Ravina E |title=The Evolution of Drug Discovery: From Traditional Medicines to Modern Drugs |date=2011 |publisher=John Wiley & Sons |isbn=978-3-527-32669-3 |page=24 |url=https://books.google.com/books?id=iDNy0XxGqT8C&pg=PA24}}</ref> In 1853, chemist [[Charles Frédéric Gerhardt]] treated the medicine [[sodium salicylate]] with [[acetyl chloride]] to produce acetylsalicylic acid for the first time.<ref name="Jeffreys2008">{{cite book |url=https://books.google.com/books?id=a9gkBwAAQBAJ |title=Aspirin the remarkable story of a wonder drug. |vauthors=Jeffreys D |date=2008 |publisher=Bloomsbury Publishing USA |isbn=978-1-59691-816-0 |archive-url=https://web.archive.org/web/20170908213430/https://books.google.com/books?id=a9gkBwAAQBAJ |archive-date=8 September 2017 |url-status=}}{{rp|46–48}}</ref> Over the next 50 years, other chemists, mostly of the German company [[Bayer]], established the chemical structure and devised more efficient production methods.<ref name=Jeffreys2008/>{{rp|69–75}} |
||
Aspirin is available [[Over-the-counter drug|without medical prescription]] as a proprietary or [[generic medication]]<ref name=AHFS/> in most jurisdictions. It is one of the most widely used medications globally, with an estimated {{convert|40000|tonne}} (50 to 120 billion [[Tablet (pharmacy)|pills]]){{Clarify|date=October 2022|reason=300mg? 75mg? Both common sizes}} consumed each year,<ref name="Jon2015" /><ref name="COX2002">{{cite journal|vauthors=Warner TD, Mitchell JA|date=October 2002|title=Cyclooxygenase-3 (COX-3): filling in the gaps toward a COX continuum?|journal=Proceedings of the National Academy of Sciences of the United States of America|volume=99|issue=21|pages=13371–3|bibcode=2002PNAS...9913371W|doi=10.1073/pnas.222543099 |pmc=129677|pmid=12374850|doi-access=free | title-link = doi }}</ref> and is on the [[WHO Model List of Essential Medicines|World Health Organization's List of Essential Medicines]].<ref name=" |
Aspirin is available [[Over-the-counter drug|without medical prescription]] as a proprietary or [[generic medication]]<ref name=AHFS/> in most jurisdictions. It is one of the most widely used medications globally, with an estimated {{convert|40000|tonne}} (50 to 120 billion [[Tablet (pharmacy)|pills]]){{Clarify|date=October 2022|reason=300mg? 75mg? Both common sizes}} consumed each year,<ref name="Jon2015" /><ref name="COX2002">{{cite journal|vauthors=Warner TD, Mitchell JA|date=October 2002|title=Cyclooxygenase-3 (COX-3): filling in the gaps toward a COX continuum?|journal=Proceedings of the National Academy of Sciences of the United States of America|volume=99|issue=21|pages=13371–3|bibcode=2002PNAS...9913371W|doi=10.1073/pnas.222543099 |pmc=129677|pmid=12374850|doi-access=free | title-link = doi }}</ref> and is on the [[WHO Model List of Essential Medicines|World Health Organization's List of Essential Medicines]].<ref name="WHO23rd">{{cite book | vauthors = ((World Health Organization)) | title = The selection and use of essential medicines 2023: web annex A: World Health Organization model list of essential medicines: 23rd list (2023) | year = 2023 | hdl = 10665/371090 | author-link = World Health Organization | publisher = World Health Organization | location = Geneva | id = WHO/MHP/HPS/EML/2023.02 | hdl-access=free }}</ref>In2021, it was the 34th most commonly [[Prescription drug|prescribed medication]] in the United States, with more than 17{{nbsp}}million prescriptions.<ref>{{cite web | title=The Top 300 of 2021 | url=https://clincalc.com/DrugStats/Top300Drugs.aspx | website=ClinCalc | access-date=14 January 2024 | archive-date=15 January 2024 | archive-url=https://web.archive.org/web/20240115223848/https://clincalc.com/DrugStats/Top300Drugs.aspx | url-status=live }}</ref><ref>{{cite web|title=Aspirin - Drug Usage Statistics, US 2013-2021|url=https://clincalc.com/DrugStats/Drugs/Aspirin|access-date=14 January 2024|website=ClinCalc}}</ref> |
||
==Brand vs. generic name== |
==Brand vs. generic name== |
||
In 1897, scientists at the [[Bayer]] company began studying acetylsalicylic acid as a less-irritating replacement medication for common salicylate medicines.<ref name=Jeffreys2008/>{{rp|69–75}}<ref name="Distillations">{{cite magazine | vauthors = Dick B |title=Hard Work and Happenstance |url=https://www.sciencehistory.org/distillations/magazine/hard-work-and-happenstance |magazine=Distillations |publisher=[[Science History Institute]] |date=2018 |volume=4 |issue=1 |pages=44–45 }}</ref> By 1899, Bayer had named it "Aspirin" and |
In 1897, scientists at the [[Bayer]] company began studying acetylsalicylic acid as a less-irritating replacement medication for common salicylate medicines.<ref name=Jeffreys2008/>{{rp|69–75}}<ref name="Distillations">{{cite magazine | vauthors = Dick B |title=Hard Work and Happenstance |url=https://www.sciencehistory.org/distillations/magazine/hard-work-and-happenstance |magazine=Distillations |publisher=[[Science History Institute]] |date=2018 |volume=4 |issue=1 |pages=44–45 }}</ref> By 1899, Bayer had named it "Aspirin" and was selling it around the world.<ref name=MannPlummer1991>{{cite book | vauthors = Mann CC, Plummer ML |title=The aspirin wars: money, medicine, and 100 years of rampant competition |date=1991 |publisher=Knopf |location=New York |isbn=978-0-394-57894-1 |page=[https://archive.org/details/aspirinwarsmoney1991mann/page/27 27] |edition=1st |url=https://archive.org/details/aspirinwarsmoney1991mann/page/27}}</ref> |
||
Aspirin's popularity grew over the first half of the 20th century, leading to competition between many brands and formulations.<ref name="ACS">{{cite magazine |title=Aspirin |magazine=Chemical & Engineering News |date=20 June 2005 |volume=83 |issue=25 |url=https://pubsapp.acs.org/cen/coverstory/83/8325/8325aspirin.html }}</ref> The word ''Aspirin'' was Bayer's brand name; however, their rights to the [[trademark]] were [[Generic trademark|lost or sold in many countries]].<ref name=ACS/> The name is ultimately a blend of the prefix '''a'''(cetyl) + '''spir''' ''[[Spiraea]]'', the meadowsweet plant genus from which the acetylsalicylic acid was originally derived at Bayer + '''-in''', the common chemical suffix. |
Aspirin's popularity grew over the first half of the 20th century, leading to competition between many brands and formulations.<ref name="ACS">{{cite magazine |title=Aspirin |magazine=Chemical & Engineering News |date=20 June 2005 |volume=83 |issue=25 |url=https://pubsapp.acs.org/cen/coverstory/83/8325/8325aspirin.html }}</ref> The word ''Aspirin'' was Bayer's brand name; however, their rights to the [[trademark]] were [[Generic trademark|lost or sold in many countries]].<ref name=ACS/> The name is ultimately a blend of the prefix '''a'''(cetyl) + '''spir''' ''[[Spiraea]]'', the meadowsweet plant genus from which the acetylsalicylic acid was originally derived at Bayer + '''-in''', the common chemical suffix.{{Citation needed|date=April 2024}} |
||
==Chemical properties== |
==Chemical properties== |
||
Aspirin decomposes rapidly in solutions of [[ammonium acetate]] or the [[acetate]]s, [[carbonate]]s, [[citrate]]s, or [[hydroxide]]s of the [[alkali metals]]. It is stable in dry air, but gradually [[hydrolyses]] in contact with moisture to [[acetic acid|acetic]] and [[salicylic acid]]s. In solution with alkalis, the hydrolysis proceeds rapidly and the clear solutions formed may consist entirely of acetate and salicylate.<ref>{{cite encyclopedia |veditors = Reynolds EF |encyclopedia=Martindale: the extra pharmacopoeia|edition=28th|year=1982|pages=[https://archive.org/details/extrapharmacopoe28mart/page/234 234–82]|title=Aspirin and similar analgesic and anti-inflammatory agents|publisher=Rittenhouse Book Distributors|isbn=978-0-85369-160-0 |url=https://archive.org/details/extrapharmacopoe28mart/page/234}}</ref> |
Aspirin decomposes rapidly in solutions of [[ammonium acetate]] or the [[acetate]]s, [[carbonate]]s, [[citrate]]s, or [[hydroxide]]s of the [[alkali metals]]. It is stable in dry air, but gradually [[hydrolyses]] in contact with moisture to [[acetic acid|acetic]] and [[salicylic acid]]s. In solution with alkalis, the hydrolysis proceeds rapidly and the clear solutions formed may consist entirely of acetate and salicylate.<ref>{{cite encyclopedia |veditors = Reynolds EF |encyclopedia=Martindale: the extra pharmacopoeia|edition=28th|year=1982|pages=[https://archive.org/details/extrapharmacopoe28mart/page/234 234–82]|title=Aspirin and similar analgesic and anti-inflammatory agents|publisher=Rittenhouse Book Distributors|isbn=978-0-85369-160-0 |url=https://archive.org/details/extrapharmacopoe28mart/page/234}}</ref> |
||
Like [[flour mill]]s, factories producing aspirin tablets must control the amount of the powder that becomes airborne inside the building, because [[dust explosion|the powder-air mixture can be explosive]]. The [[National Institute for Occupational Safety and Health]] (NIOSH) has set a [[recommended exposure limit]] in the United States of 5{{nbsp}}mg/m<sup>3</sup> (time-weighted average).<ref>{{ |
Like [[flour mill]]s, factories producing aspirin tablets must control the amount of the powder that becomes airborne inside the building, because [[dust explosion|the powder-air mixture can be explosive]]. The [[National Institute for Occupational Safety and Health]] (NIOSH) has set a [[recommended exposure limit]] in the United States of 5{{nbsp}}mg/m<sup>3</sup> (time-weighted average).<ref>{{cite web |url = https://www.cdc.gov/niosh/npg/npgd0010.html |title = Acetylsalicylic acid |date = 11 April 2016 |website = NIOSH Pocket Guide to Chemical Hazards |publisher = U.S. [[National Institute for Occupational Safety and Health]] (NIOSH) |url-status = live |archive-url = https://web.archive.org/web/20170511071608/https://www.cdc.gov/niosh/npg/npgd0010.html |archive-date = 11 May 2017}}</ref> In 1989, the [[Occupational Safety and Health Administration]] (OSHA) set a legal [[permissible exposure limit]] for aspirin of 5{{nbsp}}mg/m<sup>3</sup>, but this was vacated by the [[AFL-CIO v. OSHA]] decision in 1993.<ref>{{cite web |url = https://www.cdc.gov/niosh/npg/nengapdxg.html |title = Appendix G: 1989 Air contaminants update project – Exposure limits NOT in effect |date = 13 February 2015 |website = NIOSH pocket guide to chemical hazards |publisher = National Institute for Occupational Safety and Health |url-status = live |archive-url = https://web.archive.org/web/20170618193045/https://www.cdc.gov/niosh/npg/nengapdxg.html |archive-date = 18 June 2017}}</ref> |
||
===Synthesis=== |
===Synthesis=== |
||
The synthesis of aspirin is classified as an [[ester]]ification reaction. [[Salicylic acid]] is treated with [[acetic anhydride]], an acid derivative, causing a chemical reaction that turns salicylic acid's [[hydroxyl]] group into an [[ester]] group (R-OH → R-OCOCH<sub>3</sub>). This process yields aspirin and [[acetic acid]], which is considered a [[byproduct]] of this reaction. Small amounts of [[sulfuric acid]] (and occasionally [[phosphoric acid]]) are almost always used as a [[catalyst]]. This method is commonly demonstrated in undergraduate teaching labs.<ref>{{ |
The synthesis of aspirin is classified as an [[ester]]ification reaction. [[Salicylic acid]] is treated with [[acetic anhydride]], an acid derivative, causing a chemical reaction that turns salicylic acid's [[hydroxyl]] group into an [[ester]] group (R-OH → R-OCOCH<sub>3</sub>). This process yields aspirin and [[acetic acid]], which is considered a [[byproduct]] of this reaction. Small amounts of [[sulfuric acid]] (and occasionally [[phosphoric acid]]) are almost always used as a [[catalyst]]. This method is commonly demonstrated in undergraduate teaching labs.<ref>{{cite book|title=Experimental organic chemistry | vauthors = Palleros DR |year=2000 |publisher=John Wiley & Sons |location=New York | isbn=978-0-471-28250-1 |page=494}}</ref> |
||
[[File:Aspirin synthesis.svg|thumb|Aspirin synthesis|center|490px]]Reaction between acetic acid and salicylic acid can also form aspirin but this esterification reaction is reversible and the presence of water can lead to hydrolysis of the aspirin. So, an anhydrous reagent is preferred.<ref>{{ |
[[File:Aspirin synthesis.svg|thumb|Aspirin synthesis|center|490px]]Reaction between acetic acid and salicylic acid can also form aspirin but this esterification reaction is reversible and the presence of water can lead to hydrolysis of the aspirin. So, an anhydrous reagent is preferred.<ref>{{cite web |title=Chemical of the Week -- Acetic Acid and Acetic Anhydride |url=http://www.eng.uwaterloo.ca/~jcslee/chem/acetic.html |access-date= |website=www.eng.uwaterloo.ca |archive-date=3 November 2022 |archive-url=https://web.archive.org/web/20221103145305/http://www.eng.uwaterloo.ca/~jcslee/chem/acetic.html |url-status=dead }}</ref> |
||
;Reaction mechanism |
;Reaction mechanism |
||
| Line 151: | Line 148: | ||
There was only one proven polymorph '''Form I''' of aspirin, though the existence of another polymorph was debated since the 1960s, and one report from 1981 reported that when crystallized in the presence of aspirin ''anhydride'', the [[diffractogram]] of aspirin has weak additional peaks. Though at the time it was dismissed as mere impurity, it was, in retrospect, '''Form II''' aspirin.<ref name="Bučar-2015">{{cite journal | vauthors = Bučar DK, Lancaster RW, Bernstein J | title = Disappearing polymorphs revisited | journal = Angewandte Chemie | volume = 54 | issue = 24 | pages = 6972–6993 | date = June 2015 | pmid = 26031248 | pmc = 4479028 | doi = 10.1002/anie.201410356 }}</ref> |
There was only one proven polymorph '''Form I''' of aspirin, though the existence of another polymorph was debated since the 1960s, and one report from 1981 reported that when crystallized in the presence of aspirin ''anhydride'', the [[diffractogram]] of aspirin has weak additional peaks. Though at the time it was dismissed as mere impurity, it was, in retrospect, '''Form II''' aspirin.<ref name="Bučar-2015">{{cite journal | vauthors = Bučar DK, Lancaster RW, Bernstein J | title = Disappearing polymorphs revisited | journal = Angewandte Chemie | volume = 54 | issue = 24 | pages = 6972–6993 | date = June 2015 | pmid = 26031248 | pmc = 4479028 | doi = 10.1002/anie.201410356 }}</ref> |
||
'''Form II''' was reported in 2005,<ref>{{cite journal | vauthors = Vishweshwar P, McMahon JA, Oliveira M, Peterson ML, Zaworotko MJ | title = The predictably elusive form II of aspirin | journal = Journal of the American Chemical Society | volume = 127 | issue = 48 | pages = 16802–16803 | date = December 2005 | pmid = 16316223 | doi = 10.1021/ja056455b |
'''Form II''' was reported in 2005,<ref>{{cite journal | vauthors = Vishweshwar P, McMahon JA, Oliveira M, Peterson ML, Zaworotko MJ | title = The predictably elusive form II of aspirin | journal = Journal of the American Chemical Society | volume = 127 | issue = 48 | pages = 16802–16803 | date = December 2005 | pmid = 16316223 | doi = 10.1021/ja056455b }}</ref><ref>{{cite journal | vauthors = Bond AD, Boese R, Desiraju GR | title = On the polymorphism of aspirin: crystalline aspirin as intergrowths of two "polymorphic" domains | journal = Angewandte Chemie | volume = 46 | issue = 4 | pages = 618–622 | year = 2007 | pmid = 17139692 | doi = 10.1002/anie.200603373 }}</ref> found after attempted co-crystallization of aspirin and [[levetiracetam]] from hot [[acetonitrile]]. |
||
In form I, pairs of aspirin molecules form centrosymmetric [[Dimer (chemistry)|dimers]] through the [[acetyl]] groups with the (acidic) [[methyl]] proton to [[carbonyl]] [[hydrogen bond]]s. In form II, each aspirin molecule forms the same hydrogen bonds, but with two neighbouring molecules instead of one. With respect to the hydrogen bonds formed by the [[carboxylic acid]] groups, both polymorphs form identical dimer structures. The aspirin polymorphs contain identical 2-dimensional sections and are therefore more precisely described as polytypes.<ref>{{cite web |title=Polytypism - Online Dictionary of Crystallography |url=http://reference.iucr.org/dictionary/Polytypism |website=reference.iucr.org}}</ref> |
In form I, pairs of aspirin molecules form centrosymmetric [[Dimer (chemistry)|dimers]] through the [[acetyl]] groups with the (acidic) [[methyl]] proton to [[carbonyl]] [[hydrogen bond]]s. In form II, each aspirin molecule forms the same hydrogen bonds, but with two neighbouring molecules instead of one. With respect to the hydrogen bonds formed by the [[carboxylic acid]] groups, both polymorphs form identical dimer structures. The aspirin polymorphs contain identical 2-dimensional sections and are therefore more precisely described as polytypes.<ref>{{cite web |title=Polytypism - Online Dictionary of Crystallography |url=http://reference.iucr.org/dictionary/Polytypism |website=reference.iucr.org}}</ref> |
||
| Line 165: | Line 162: | ||
===Prostaglandins and thromboxanes=== |
===Prostaglandins and thromboxanes=== |
||
Aspirin's ability to suppress the production of prostaglandins and thromboxanes is due to its irreversible inactivation of the [[cyclooxygenase]] (COX; officially known as prostaglandin-endoperoxide synthase, PTGS) enzyme required for prostaglandin and thromboxane synthesis. Aspirin acts as an acetylating agent where an acetyl group is covalently attached to a [[serine]] residue in the active site of the |
Aspirin's ability to suppress the production of prostaglandins and thromboxanes is due to its irreversible inactivation of the [[cyclooxygenase]] (COX; officially known as prostaglandin-endoperoxide synthase, PTGS) enzyme required for prostaglandin and thromboxane synthesis. Aspirin acts as an acetylating agent where an acetyl group is covalently attached to a [[serine]] residue in the active site of the COX enzyme ([[Suicide inhibition]]). This makes aspirin different from other NSAIDs (such as [[diclofenac]] and [[ibuprofen]]), which are reversible inhibitors. |
||
Low-dose aspirin use irreversibly blocks the formation of [[thromboxane A2|thromboxane A<sub>2</sub>]] in platelets, producing an inhibitory effect on platelet aggregation during the lifetime of the affected platelet (8–9 days). This antithrombotic property makes aspirin useful for reducing the incidence of heart attacks in people who have had a heart attack, unstable angina, ischemic stroke or transient ischemic attack.<ref>{{cite web |url=http://www.americanheart.org/presenter.jhtml?identifier=4456 |title=Aspirin in heart attack and stroke prevention |access-date=8 May 2008 |publisher=American Heart Association |archive-url=https://web.archive.org/web/20080331031146/http://www.americanheart.org/presenter.jhtml?identifier=4456 |archive-date=31 March 2008 }}</ref> 40{{nbsp}}mg of aspirin a day is able to inhibit a large proportion of maximum thromboxane A<sub>2</sub> release provoked acutely, with the prostaglandin |
Low-dose aspirin use irreversibly blocks the formation of [[thromboxane A2|thromboxane A<sub>2</sub>]] in platelets, producing an inhibitory effect on platelet aggregation during the lifetime of the affected platelet (8–9 days). This antithrombotic property makes aspirin useful for reducing the incidence of heart attacks in people who have had a heart attack, unstable angina, ischemic stroke or transient ischemic attack.<ref>{{cite web |url=http://www.americanheart.org/presenter.jhtml?identifier=4456 |title=Aspirin in heart attack and stroke prevention |access-date=8 May 2008 |publisher=American Heart Association |archive-url=https://web.archive.org/web/20080331031146/http://www.americanheart.org/presenter.jhtml?identifier=4456 |archive-date=31 March 2008 }}</ref> 40{{nbsp}}mg of aspirin a day is able to inhibit a large proportion of maximum thromboxane A<sub>2</sub> release provoked acutely, with the prostaglandin I<sub>2</sub> synthesis being little affected; however, higher doses of aspirin are required to attain further inhibition.<ref>{{cite journal | vauthors = Tohgi H, Konno S, Tamura K, Kimura B, Kawano K | title = Effects of low-to-high doses of aspirin on platelet aggregability and metabolites of thromboxane A2 and prostacyclin | journal = Stroke | volume = 23 | issue = 10 | pages = 1400–3 | date = October 1992 | pmid = 1412574 | doi = 10.1161/01.STR.23.10.1400 | doi-access = free | title-link = doi }}</ref> |
||
Prostaglandins, local [[hormone]]s produced in the body, have diverse effects, including the transmission of pain information to the brain, modulation of the [[hypothalamus|hypothalamic]] thermostat, and inflammation. Thromboxanes are responsible for the aggregation of platelets that form [[clot|blood clots]]. Heart attacks are caused primarily by blood clots, and low doses of aspirin are seen as an effective medical intervention to prevent a second acute myocardial infarction.<ref name="pmid19482214">{{cite journal |
Prostaglandins, local [[hormone]]s produced in the body, have diverse effects, including the transmission of pain information to the brain, modulation of the [[hypothalamus|hypothalamic]] thermostat, and inflammation. Thromboxanes are responsible for the aggregation of platelets that form [[clot|blood clots]]. Heart attacks are caused primarily by blood clots, and low doses of aspirin are seen as an effective medical intervention to prevent a second acute myocardial infarction.<ref name="pmid19482214">{{cite journal |vauthors=Baigent C, Blackwell L, Collins R, Emberson J, Godwin J, Peto R, Buring J, Hennekens C, Kearney P, Meade T, Patrono C, Roncaglioni MC, Zanchetti A |date=May 2009 |title=Aspirin in the primary and secondary prevention of vascular disease: collaborative meta-analysis of individual participant data from randomised trials |journal=Lancet |volume=373 |issue=9678 |pages=1849–60 |doi=10.1016/S0140-6736(09)60503-1 |pmc=2715005 |pmid=19482214}}</ref> |
||
===COX-1 and COX-2 inhibition=== |
===COX-1 and COX-2 inhibition=== |
||
At least two different types of [[cyclooxygenase]]s, [[COX-1]] and [[COX-2]], are acted on by aspirin. Aspirin irreversibly inhibits COX-1 and modifies the enzymatic activity of COX-2. COX-2 normally produces [[prostanoid]]s, most of which are proinflammatory. Aspirin-modified |
At least two different types of [[cyclooxygenase]]s, [[COX-1]] and [[COX-2]], are acted on by aspirin. Aspirin irreversibly inhibits COX-1 and modifies the enzymatic activity of COX-2. COX-2 normally produces [[prostanoid]]s, most of which are proinflammatory. Aspirin-modified COX-2 (aka [[prostaglandin-endoperoxide synthase 2]] or PTGS2) produces lipoxins, most of which are anti-inflammatory.<ref>{{cite journal |vauthors=Goel A, Aggarwal S, Partap S, Saurabh A, Choudhary |date=2012 |title=Pharmacokinetic solubility and dissolution profile of antiarrythmic drugs |journal=Int J Pharma Prof Res |volume=3 |issue=1 |pages=592–601}}</ref>{{Verify source|date=August 2016}} Newer NSAID drugs, [[COX-2 inhibitor]]s (coxibs), have been developed to inhibit only COX-2, with the intent to reduce the incidence of gastrointestinal side effects.<ref name=COX2002/> |
||
Several COX-2 inhibitors, such as [[rofecoxib]] (Vioxx), have been withdrawn from the market, after evidence emerged that |
Several COX-2 inhibitors, such as [[rofecoxib]] (Vioxx), have been withdrawn from the market, after evidence emerged that COX-2 inhibitors increase the risk of heart attack and stroke.<ref>{{cite journal | vauthors = Martínez-González J, Badimon L | title = Mechanisms underlying the cardiovascular effects of COX-inhibition: benefits and risks | journal = Current Pharmaceutical Design | volume = 13 | issue = 22 | pages = 2215–27 | year = 2007 | pmid = 17691994 | doi = 10.2174/138161207781368774 }}</ref><ref>{{cite journal | vauthors = Funk CD, FitzGerald GA | title = COX-2 inhibitors and cardiovascular risk | journal = Journal of Cardiovascular Pharmacology | volume = 50 | issue = 5 | pages = 470–9 | date = November 2007 | pmid = 18030055 | doi = 10.1097/FJC.0b013e318157f72d | s2cid = 39103383 | doi-access = free }}</ref> Endothelial cells lining the microvasculature in the body are proposed to express COX-2, and, by selectively inhibiting COX-2, prostaglandin production (specifically, PGI<sub>2</sub>; prostacyclin) is downregulated with respect to thromboxane levels, as COX-1 in platelets is unaffected. Thus, the protective anticoagulative effect of [[PGI2|PGI<sub>2</sub>]] is removed, increasing the risk of thrombus and associated heart attacks and other circulatory problems. Since platelets have no DNA, they are unable to synthesize new COX once aspirin has irreversibly inhibited the enzyme, an important difference as compared with reversible inhibitors. |
||
Furthermore, aspirin, while inhibiting the ability of COX-2 to form pro-inflammatory products such as the [[prostaglandins]], converts this enzyme's activity from a prostaglandin-forming cyclooxygenase to a [[lipoxygenase]]-like enzyme: aspirin-treated COX-2 metabolizes a variety of [[polyunsaturated fatty acids]] to hydroperoxy products which are then further metabolized to [[specialized proresolving mediators]] such as the aspirin-triggered [[lipoxin]]s, aspirin-triggered [[resolvins]], and aspirin-triggered [[maresin]]s. These mediators possess potent anti-inflammatory activity. It is proposed that this aspirin-triggered transition of COX-2 from cyclooxygenase to lipoxygenase activity and the consequential formation of specialized proresolving mediators contributes to the anti-inflammatory effects of aspirin.<ref name="pmid25895638">{{cite journal | vauthors = Romano M, Cianci E, Simiele F, Recchiuti A | title = Lipoxins and aspirin-triggered lipoxins in resolution of inflammation | journal = European Journal of Pharmacology | volume = 760 | pages = 49–63 | date = August 2015 | pmid = 25895638 | doi = 10.1016/j.ejphar.2015.03.083 }}</ref><ref name="pmid23747022">{{cite journal | vauthors = Serhan CN, Chiang N | title = Resolution phase lipid mediators of inflammation: agonists of resolution | journal = Current Opinion in Pharmacology | volume = 13 | issue = 4 | pages = 632–40 | date = August 2013 | pmid = 23747022 | pmc = 3732499 | doi = 10.1016/j.coph.2013.05.012 }}</ref><ref name="pmid26546723">{{cite journal | vauthors = Weylandt KH | title = Docosapentaenoic acid derived metabolites and mediators - The new world of lipid mediator medicine in a nutshell | journal = European Journal of Pharmacology | volume = 785 | pages = 108–115 | date = August 2016 | pmid = 26546723 | doi = 10.1016/j.ejphar.2015.11.002 }}</ref> |
Furthermore, aspirin, while inhibiting the ability of COX-2 to form pro-inflammatory products such as the [[prostaglandins]], converts this enzyme's activity from a prostaglandin-forming cyclooxygenase to a [[lipoxygenase]]-like enzyme: aspirin-treated COX-2 metabolizes a variety of [[polyunsaturated fatty acids]] to hydroperoxy products which are then further metabolized to [[specialized proresolving mediators]] such as the aspirin-triggered [[lipoxin]]s, aspirin-triggered [[resolvins]], and aspirin-triggered [[maresin]]s. These mediators possess potent anti-inflammatory activity. It is proposed that this aspirin-triggered transition of COX-2 from cyclooxygenase to lipoxygenase activity and the consequential formation of specialized proresolving mediators contributes to the anti-inflammatory effects of aspirin.<ref name="pmid25895638">{{cite journal | vauthors = Romano M, Cianci E, Simiele F, Recchiuti A | title = Lipoxins and aspirin-triggered lipoxins in resolution of inflammation | journal = European Journal of Pharmacology | volume = 760 | pages = 49–63 | date = August 2015 | pmid = 25895638 | doi = 10.1016/j.ejphar.2015.03.083 }}</ref><ref name="pmid23747022">{{cite journal | vauthors = Serhan CN, Chiang N | title = Resolution phase lipid mediators of inflammation: agonists of resolution | journal = Current Opinion in Pharmacology | volume = 13 | issue = 4 | pages = 632–40 | date = August 2013 | pmid = 23747022 | pmc = 3732499 | doi = 10.1016/j.coph.2013.05.012 }}</ref><ref name="pmid26546723">{{cite journal | vauthors = Weylandt KH | title = Docosapentaenoic acid derived metabolites and mediators - The new world of lipid mediator medicine in a nutshell | journal = European Journal of Pharmacology | volume = 785 | pages = 108–115 | date = August 2016 | pmid = 26546723 | doi = 10.1016/j.ejphar.2015.11.002 }}</ref> |
||
===Additional mechanisms=== |
===Additional mechanisms=== |
||
Aspirin has been shown to have at least three additional modes of action. It uncouples [[oxidative phosphorylation]] in cartilaginous (and hepatic) mitochondria, by diffusing from the inner membrane space as a proton carrier back into the mitochondrial matrix, where it ionizes once again to release protons.<ref name="SomasundaramS">{{cite journal | vauthors = Somasundaram S, Sigthorsson G, Simpson RJ, Watts J, Jacob M, Tavares IA, Rafi S, Roseth A, Foster R, Price AB, Wrigglesworth JM, Bjarnason I |
Aspirin has been shown to have at least three additional modes of action. It uncouples [[oxidative phosphorylation]] in cartilaginous (and hepatic) mitochondria, by diffusing from the inner membrane space as a proton carrier back into the mitochondrial matrix, where it ionizes once again to release protons.<ref name="SomasundaramS">{{cite journal | vauthors = Somasundaram S, Sigthorsson G, Simpson RJ, Watts J, Jacob M, Tavares IA, Rafi S, Roseth A, Foster R, Price AB, Wrigglesworth JM, Bjarnason I | title = Uncoupling of intestinal mitochondrial oxidative phosphorylation and inhibition of cyclooxygenase are required for the development of NSAID-enteropathy in the rat | journal = Alimentary Pharmacology & Therapeutics | volume = 14 | issue = 5 | pages = 639–50 | date = May 2000 | pmid = 10792129 | doi = 10.1046/j.1365-2036.2000.00723.x | s2cid = 44832283 | doi-access = free | title-link = doi }}</ref> Aspirin buffers and transports the protons. When high doses are given, it may actually cause fever, owing to the heat released from the electron transport chain, as opposed to the antipyretic action of aspirin seen with lower doses. In addition, aspirin induces the formation of NO-radicals in the body, which have been shown in mice to have an independent mechanism of reducing inflammation. This reduced leukocyte adhesion is an important step in the immune response to infection; however, evidence is insufficient to show aspirin helps to fight infection.<ref>{{cite journal | vauthors = Paul-Clark MJ, Van Cao T, Moradi-Bidhendi N, Cooper D, Gilroy DW | title = 15-epi-lipoxin A4-mediated induction of nitric oxide explains how aspirin inhibits acute inflammation | journal = The Journal of Experimental Medicine | volume = 200 | issue = 1 | pages = 69–78 | date = July 2004 | pmid = 15238606 | pmc = 2213311 | doi = 10.1084/jem.20040566 }}</ref> More recent data also suggest salicylic acid and its derivatives modulate signalling through [[NF-κB]].<ref>{{cite journal | vauthors = McCarty MF, Block KI | title = Preadministration of high-dose salicylates, suppressors of NF-kappaB activation, may increase the chemosensitivity of many cancers: an example of proapoptotic signal modulation therapy | journal = Integrative Cancer Therapies | volume = 5 | issue = 3 | pages = 252–68 | date = September 2006 | pmid = 16880431 | doi = 10.1177/1534735406291499 | doi-access = free | title-link = doi }}</ref> NF-κB, a [[transcription factor]] complex, plays a central role in many biological processes, including inflammation.<ref>{{cite journal | vauthors = Silva Caldas AP, Chaves LO, Linhares Da Silva L, De Castro Morais D, Gonçalves Alfenas RD |date=29 December 2017|title=Mechanisms involved in the cardioprotective effect of avocado consumption: A systematic review|journal=International Journal of Food Properties|volume=20|issue=sup2|pages=1675–1685 |doi=10.1080/10942912.2017.1352601 |issn=1094-2912|quote=...there was postprandial reduction on the plasma concentration of IL-6 and IkBα preservation, followed by the lower activation of NFκB, considered the main transcription factor capable of inducing inflammatory response by stimulating the expression of proinflammatory cytokines, chemokines, and adhesion molecules.|doi-access=free | title-link = doi }}</ref><ref>{{cite journal | vauthors = Chen L, Deng H, Cui H, Fang J, Zuo Z, Deng J, Li Y, Wang X, Zhao L | title = Inflammatory responses and inflammation-associated diseases in organs | journal = Oncotarget | volume = 9 | issue = 6 | pages = 7204–7218 | date = January 2018 | pmid = 29467962 | pmc = 5805548 | doi = 10.18632/oncotarget.23208 }}</ref><ref>{{cite journal | vauthors = Lawrence T | title = The nuclear factor NF-kappaB pathway in inflammation | journal = Cold Spring Harbor Perspectives in Biology | volume = 1 | issue = 6 | pages = a001651 | date = December 2009 | pmid = 20457564 | pmc = 2882124 | doi = 10.1101/cshperspect.a001651 }}</ref> |
||
Aspirin is readily broken down in the body to salicylic acid, which itself has anti-inflammatory, antipyretic, and analgesic effects. In 2012, salicylic acid was found to activate [[AMP-activated protein kinase]], which has been suggested as a possible explanation for some of the effects of both salicylic acid and aspirin.<ref>{{cite journal | vauthors = Hawley SA, Fullerton MD, Ross FA, Schertzer JD, Chevtzoff C, Walker KJ, Peggie MW, Zibrova D, Green KA, Mustard KJ, Kemp BE, Sakamoto K, Steinberg GR, Hardie DG |
Aspirin is readily broken down in the body to salicylic acid, which itself has anti-inflammatory, antipyretic, and analgesic effects. In 2012, salicylic acid was found to activate [[AMP-activated protein kinase]], which has been suggested as a possible explanation for some of the effects of both salicylic acid and aspirin.<ref>{{cite journal | vauthors = Hawley SA, Fullerton MD, Ross FA, Schertzer JD, Chevtzoff C, Walker KJ, Peggie MW, Zibrova D, Green KA, Mustard KJ, Kemp BE, Sakamoto K, Steinberg GR, Hardie DG | title = The ancient drug salicylate directly activates AMP-activated protein kinase | journal = Science | volume = 336 | issue = 6083 | pages = 918–22 | date = May 2012 | pmid = 22517326 | pmc = 3399766 | doi = 10.1126/science.1215327 | bibcode = 2012Sci...336..918H }}</ref><ref>{{cite journal |title=Clues to aspirin's anti-cancer effects revealed |journal=New Scientist |date=28 April 2012 |volume=214 |issue=2862 |pages=16 |doi=10.1016/S0262-4079(12)61073-2 }}</ref> The acetyl portion of the aspirin molecule has its own targets. Acetylation of cellular proteins is a well-established phenomenon in the regulation of protein function at the post-translational level. Aspirin is able to acetylate several other targets in addition to COX isoenzymes.<ref>{{cite journal | vauthors = Alfonso LF, Srivenugopal KS, Arumugam TV, Abbruscato TJ, Weidanz JA, Bhat GJ | title = Aspirin inhibits camptothecin-induced p21CIP1 levels and potentiates apoptosis in human breast cancer cells | journal = International Journal of Oncology | volume = 34 | issue = 3 | pages = 597–608 | date = March 2009 | pmid = 19212664 | doi = 10.3892/ijo_00000185 | doi-access = free | title-link = doi }}</ref><ref>{{cite journal | vauthors = Alfonso LF, Srivenugopal KS, Bhat GJ | title = Does aspirin acetylate multiple cellular proteins? (Review) | journal = Molecular Medicine Reports | volume = 2 | issue = 4 | pages = 533–7 | year = 2009 | pmid = 21475861 | doi = 10.3892/mmr_00000132 | type = review | doi-access = free | title-link = doi }}</ref> These acetylation reactions may explain many hitherto unexplained effects of aspirin.<ref>{{cite journal | vauthors = Alfonso LF, Srivenugopal KS, Bhat GJ | title = Does aspirin acetylate multiple cellular proteins? (Review) | journal = Molecular Medicine Reports | volume = 2 | issue = 4 | pages = 533–537 | date = 4 June 2009 | pmid = 21475861 | doi = 10.3892/mmr_00000132 | doi-access = free }}</ref> |
||
==Formulations== |
==Formulations== |
||
| Line 191: | Line 188: | ||
*Buffered formulations containing aspirin with one of many buffering agents. |
*Buffered formulations containing aspirin with one of many buffering agents. |
||
*Formulations of aspirin with vitamin C (ASA-VitC) |
*Formulations of aspirin with vitamin C (ASA-VitC) |
||
*A phospholipid-aspirin complex liquid formulation, PL-ASA. {{As of|2023}} the phospholipid coating was being trialled to determine if it caused less gastrointestinal damage.<ref name=franchi>{{cite journal | vauthors = Franchi F, Schneider D, Prats J, Fan W, Rollini F, Been L, Taatjes-Sommer H, Deliargyris E, Angiolillo D |
*A phospholipid-aspirin complex liquid formulation, PL-ASA. {{As of|2023}} the phospholipid coating was being trialled to determine if it caused less gastrointestinal damage.<ref name=franchi>{{cite journal | vauthors = Franchi F, Schneider D, Prats J, Fan W, Rollini F, Been L, Taatjes-Sommer H, Deliargyris E, Angiolillo D | title=TCT-320 Pharmacokinetic and Pharmacodynamic Profile of PL-ASA, a Novel Phospholipid-Aspirin Complex Liquid Formulation, Compared to Enteric-Coated Aspirin at an 81-mg Dose – Results From a Prospective, Randomized, Crossover Study | journal=Journal of the American College of Cardiology | publisher=Elsevier BV | volume=78 | issue=19 | year=2021 | issn=0735-1097 | doi=10.1016/j.jacc.2021.09.1173|doi-access=free| page=B131}}</ref> |
||
==Pharmacokinetics== |
==Pharmacokinetics== |
||
| Line 200: | Line 197: | ||
As much as 80% of therapeutic doses of salicylic acid is [[metabolism|metabolized]] in the [[liver]]. [[Conjugated system|Conjugation]] with [[glycine]] forms [[salicyluric acid]], and with [[glucuronic acid]] to form two different glucuronide esters. The conjugate with the acetyl group intact is referred to as the ''acyl glucuronide''; the deacetylated conjugate is the ''phenolic glucuronide''. These metabolic pathways have only a limited capacity. Small amounts of salicylic acid are also hydroxylated to [[gentisic acid]]. With large salicylate doses, the kinetics switch from first-order to zero-order, as [[metabolic pathway]]s become saturated and [[kidney|renal]] excretion becomes increasingly important.<ref name="G Levy"/> |
As much as 80% of therapeutic doses of salicylic acid is [[metabolism|metabolized]] in the [[liver]]. [[Conjugated system|Conjugation]] with [[glycine]] forms [[salicyluric acid]], and with [[glucuronic acid]] to form two different glucuronide esters. The conjugate with the acetyl group intact is referred to as the ''acyl glucuronide''; the deacetylated conjugate is the ''phenolic glucuronide''. These metabolic pathways have only a limited capacity. Small amounts of salicylic acid are also hydroxylated to [[gentisic acid]]. With large salicylate doses, the kinetics switch from first-order to zero-order, as [[metabolic pathway]]s become saturated and [[kidney|renal]] excretion becomes increasingly important.<ref name="G Levy"/> |
||
Salicylates are excreted mainly by the kidneys as salicyluric acid (75%), free salicylic acid (10%), salicylic phenol (10%), and acyl glucuronides (5%), [[gentisic acid]] (< 1%), and [[2,3-Dihydroxybenzoic acid|2,3-dihydroxybenzoic acid]].<ref name="pmid3342084">{{cite journal | vauthors = Grootveld M, Halliwell B | title = 2,3-Dihydroxybenzoic acid is a product of human aspirin metabolism | journal = Biochemical Pharmacology | volume = 37 | issue = 2 | pages = 271–80 | date = January 1988 | pmid = 3342084 | doi = 10.1016/0006-2952(88)90729-0 }}</ref> When small doses (less than 250{{nbsp}}mg in an adult) are ingested, all pathways proceed by first-order kinetics, with an elimination half-life of about 2.0 h to 4.5 h.<ref name="O Hartwig">{{cite journal | vauthors = Hartwig-Otto H | title = Pharmacokinetic considerations of common analgesics and antipyretics | journal = The American Journal of Medicine | volume = 75 | issue = 5A | pages = 30–7 | date = November 1983 | pmid = 6606362 | doi = 10.1016/0002-9343(83)90230-9 }}</ref><ref name="AK Done">{{cite journal | vauthors = Done AK | title = Salicylate intoxication. Significance of measurements of salicylate in blood in cases of acute ingestion | journal = Pediatrics | volume = 26 | pages = 800–7 | date = November 1960 | doi = 10.1542/peds.26.5.800 | pmid = 13723722 | s2cid = 245036862 }}</ref> When higher doses of salicylate are ingested (more than 4 g), the half-life becomes much longer (15 h to 30 h),<ref name="Chyka2007">{{cite journal | vauthors = Chyka PA, Erdman AR, Christianson G, Wax PM, Booze LL, Manoguerra AS, Caravati EM, Nelson LS, Olson KR, Cobaugh DJ, Scharman EJ, Woolf AD, Troutman WG |
Salicylates are excreted mainly by the kidneys as salicyluric acid (75%), free salicylic acid (10%), salicylic phenol (10%), and acyl glucuronides (5%), [[gentisic acid]] (< 1%), and [[2,3-Dihydroxybenzoic acid|2,3-dihydroxybenzoic acid]].<ref name="pmid3342084">{{cite journal | vauthors = Grootveld M, Halliwell B | title = 2,3-Dihydroxybenzoic acid is a product of human aspirin metabolism | journal = Biochemical Pharmacology | volume = 37 | issue = 2 | pages = 271–80 | date = January 1988 | pmid = 3342084 | doi = 10.1016/0006-2952(88)90729-0 }}</ref> When small doses (less than 250{{nbsp}}mg in an adult) are ingested, all pathways proceed by first-order kinetics, with an elimination half-life of about 2.0 h to 4.5 h.<ref name="O Hartwig">{{cite journal | vauthors = Hartwig-Otto H | title = Pharmacokinetic considerations of common analgesics and antipyretics | journal = The American Journal of Medicine | volume = 75 | issue = 5A | pages = 30–7 | date = November 1983 | pmid = 6606362 | doi = 10.1016/0002-9343(83)90230-9 }}</ref><ref name="AK Done">{{cite journal | vauthors = Done AK | title = Salicylate intoxication. Significance of measurements of salicylate in blood in cases of acute ingestion | journal = Pediatrics | volume = 26 | pages = 800–7 | date = November 1960 | doi = 10.1542/peds.26.5.800 | pmid = 13723722 | s2cid = 245036862 }}</ref> When higher doses of salicylate are ingested (more than 4 g), the half-life becomes much longer (15 h to 30 h),<ref name="Chyka2007">{{cite journal | vauthors = Chyka PA, Erdman AR, Christianson G, Wax PM, Booze LL, Manoguerra AS, Caravati EM, Nelson LS, Olson KR, Cobaugh DJ, Scharman EJ, Woolf AD, Troutman WG | title = Salicylate poisoning: an evidence-based consensus guideline for out-of-hospital management | journal = Clinical Toxicology | volume = 45 | issue = 2 | pages = 95–131 | year = 2007 | pmid = 17364628 | doi = 10.1080/15563650600907140 | doi-access = free | title-link = doi }}</ref> because the biotransformation pathways concerned with the formation of salicyluric acid and salicyl phenolic glucuronide become saturated.<ref>{{cite journal | vauthors = Prescott LF, Balali-Mood M, Critchley JA, Johnstone AF, Proudfoot AT | title = Diuresis or urinary alkalinisation for salicylate poisoning? | journal = British Medical Journal | volume = 285 | issue = 6352 | pages = 1383–6 | date = November 1982 | pmid = 6291695 | pmc = 1500395 | doi = 10.1136/bmj.285.6352.1383 }}</ref> Renal excretion of salicylic acid becomes increasingly important as the metabolic pathways become saturated, because it is extremely sensitive to changes in [[urine|urinary]] pH. A 10- to 20-fold increase in renal clearance occurs when urine pH is increased from 5 to 8. The use of urinary alkalinization exploits this particular aspect of salicylate elimination.<ref name="EmergMed2002-Dargan">{{cite journal | vauthors = Dargan PI, Wallace CI, Jones AL | title = An evidence based flowchart to guide the management of acute salicylate (aspirin) overdose | journal = Emergency Medicine Journal | volume = 19 | issue = 3 | pages = 206–9 | date = May 2002 | pmid = 11971828 | pmc = 1725844 | doi = 10.1136/emj.19.3.206 }}</ref> It was found that short-term aspirin use in therapeutic doses might precipitate reversible [[acute kidney injury]] when the patient was ill with [[glomerulonephritis]] or [[cirrhosis]].<ref name=amjkid/> Aspirin for some patients with [[chronic kidney disease]] and some children with congestive heart failure was contraindicated.<ref name=amjkid>{{cite journal | vauthors = D'Agati V | title = Does aspirin cause acute or chronic renal failure in experimental animals and in humans? | journal = American Journal of Kidney Diseases | volume = 28 | issue = 1 Suppl 1 | pages = S24-9 | date = July 1996 | pmid = 8669425 | doi = 10.1016/s0272-6386(96)90565-x }}</ref> |
||
==History== |
==History== |
||
| Line 211: | Line 208: | ||
In 1853, chemist [[Charles Frédéric Gerhardt]] treated [[sodium salicylate]] with [[acetyl chloride]] to produce acetylsalicylic acid for the first time;<ref name=Jeffreys2008/>{{rp|46–48}} in the second half of the 19th century, other academic chemists established the compound's chemical structure and devised more efficient methods of synthesis. In 1897, scientists at the drug and dye firm [[Bayer]] began investigating acetylsalicylic acid as a less-irritating replacement for standard common salicylate medicines, and identified a new way to synthesize it.<ref name=Jeffreys2008/>{{rp|69–75}} By 1899, Bayer had dubbed this drug Aspirin and was selling it globally.<ref name=MannPlummer1991/>{{rp|27}} The word ''Aspirin'' was Bayer's brand name, rather than the generic name of the drug; however, Bayer's rights to the trademark were lost or sold in many countries. Aspirin's popularity grew over the first half of the 20th century leading to fierce competition with the proliferation of aspirin brands and products.<ref name=ACS/> |
In 1853, chemist [[Charles Frédéric Gerhardt]] treated [[sodium salicylate]] with [[acetyl chloride]] to produce acetylsalicylic acid for the first time;<ref name=Jeffreys2008/>{{rp|46–48}} in the second half of the 19th century, other academic chemists established the compound's chemical structure and devised more efficient methods of synthesis. In 1897, scientists at the drug and dye firm [[Bayer]] began investigating acetylsalicylic acid as a less-irritating replacement for standard common salicylate medicines, and identified a new way to synthesize it.<ref name=Jeffreys2008/>{{rp|69–75}} By 1899, Bayer had dubbed this drug Aspirin and was selling it globally.<ref name=MannPlummer1991/>{{rp|27}} The word ''Aspirin'' was Bayer's brand name, rather than the generic name of the drug; however, Bayer's rights to the trademark were lost or sold in many countries. Aspirin's popularity grew over the first half of the 20th century leading to fierce competition with the proliferation of aspirin brands and products.<ref name=ACS/> |
||
Aspirin's popularity declined after the development of [[paracetamol|acetaminophen/paracetamol]] in 1956 and [[ibuprofen]] in 1962. In the 1960s and 1970s, [[John Vane]] and others discovered the basic mechanism of aspirin's effects,<ref name=Jeffreys2008/>{{rp|226–231}} while clinical trials and other studies from the 1960s to the 1980s established aspirin's efficacy as an anti-clotting agent that reduces the risk of clotting diseases.<ref name=Jeffreys2008/>{{rp|247–257}} The initial large studies on the use of low-dose aspirin to prevent heart attacks that were published in the 1970s and 1980s helped spur reform in [[clinical research ethics]] and [[guidelines for human subject research]] and US federal law, and are often cited as examples of clinical trials that included only men, but from which people drew general conclusions that did not hold true for women.<ref>{{cite journal | vauthors = Schiebinger L | title = Women's health and clinical trials | journal = The Journal of Clinical Investigation | volume = 112 | issue = 7 | pages = 973–7 | date = October 2003 | pmid = 14523031 | pmc = 198535 | doi = 10.1172/JCI19993 }}</ref><ref>{{cite journal | vauthors = | title = Regular aspirin intake and acute myocardial infarction | journal = British Medical Journal | volume = 1 | issue = 5905 | pages = 440–3 | date = March 1974 | pmid = 4816857 | pmc = 1633212 | doi = 10.1136/bmj.1.5905.440 }}</ref><ref>{{cite journal | vauthors = Elwood PC, Cochrane AL, Burr ML, Sweetnam PM, Williams G, Welsby E, Hughes SJ, Renton R |
Aspirin's popularity declined after the development of [[paracetamol|acetaminophen/paracetamol]] in 1956 and [[ibuprofen]] in 1962. In the 1960s and 1970s, [[John Vane]] and others discovered the basic mechanism of aspirin's effects,<ref name=Jeffreys2008/>{{rp|226–231}} while clinical trials and other studies from the 1960s to the 1980s established aspirin's efficacy as an anti-clotting agent that reduces the risk of clotting diseases.<ref name=Jeffreys2008/>{{rp|247–257}} The initial large studies on the use of low-dose aspirin to prevent heart attacks that were published in the 1970s and 1980s helped spur reform in [[clinical research ethics]] and [[guidelines for human subject research]] and US federal law, and are often cited as examples of clinical trials that included only men, but from which people drew general conclusions that did not hold true for women.<ref>{{cite journal | vauthors = Schiebinger L | title = Women's health and clinical trials | journal = The Journal of Clinical Investigation | volume = 112 | issue = 7 | pages = 973–7 | date = October 2003 | pmid = 14523031 | pmc = 198535 | doi = 10.1172/JCI19993 }}</ref><ref>{{cite journal | vauthors = | title = Regular aspirin intake and acute myocardial infarction | journal = British Medical Journal | volume = 1 | issue = 5905 | pages = 440–3 | date = March 1974 | pmid = 4816857 | pmc = 1633212 | doi = 10.1136/bmj.1.5905.440 }}</ref><ref>{{cite journal | vauthors = Elwood PC, Cochrane AL, Burr ML, Sweetnam PM, Williams G, Welsby E, Hughes SJ, Renton R | title = A randomized controlled trial of acetyl salicylic acid in the secondary prevention of mortality from myocardial infarction | journal = British Medical Journal | volume = 1 | issue = 5905 | pages = 436–40 | date = March 1974 | pmid = 4593555 | pmc = 1633246 | doi = 10.1136/bmj.1.5905.436 }}</ref> |
||
Aspirin sales revived considerably in the last decades of the 20th century, and remain strong in the 21st century with widespread use as a preventive treatment for [[heart attack]]s and [[stroke]]s.<ref name=Jeffreys2008/>{{rp|267–269}} |
Aspirin sales revived considerably in the last decades of the 20th century, and remain strong in the 21st century with widespread use as a preventive treatment for [[heart attack]]s and [[stroke]]s.<ref name=Jeffreys2008/>{{rp|267–269}} |
||
| Line 230: | Line 227: | ||
| caption2 = In the US., "aspirin" is a generic name. |
| caption2 = In the US., "aspirin" is a generic name. |
||
}} |
}} |
||
Bayer lost its trademark for Aspirin in the United States and some other countries in actions taken between 1918 and 1921 because it had failed to use the name for its own product correctly and had for years allowed the use of "Aspirin" by other manufacturers without defending the intellectual property rights.<ref>{{cite court |litigants=Bayer Co. v. United Drug Co. |vol=272 |reporter=F. |opinion=505 |pinpoint=p.512 |court=S.D.N.Y |date=1921 |url=https://cyber.law.harvard.edu/metaschool/fisher/domain/tmcases/bayer.htm }}</ref> Today, aspirin is a [[generic trademark]] in many countries.<ref>{{cite web |url= https://www.genericides.org/trademark/aspirin |title= Has aspirin become a generic trademark? |access-date= 17 February 2021 |website= genericides.org |date= 25 March 2020 |archive-date= 5 March 2021 |archive-url= https://web.archive.org/web/20210305221908/https://genericides.org/trademark/aspirin |url-status= dead }}</ref><ref>{{ |
Bayer lost its trademark for Aspirin in the United States and some other countries in actions taken between 1918 and 1921 because it had failed to use the name for its own product correctly and had for years allowed the use of "Aspirin" by other manufacturers without defending the intellectual property rights.<ref>{{cite court |litigants=Bayer Co. v. United Drug Co. |vol=272 |reporter=F. |opinion=505 |pinpoint=p.512 |court=S.D.N.Y |date=1921 |url=https://cyber.law.harvard.edu/metaschool/fisher/domain/tmcases/bayer.htm }}</ref> Today, aspirin is a [[generic trademark]] in many countries.<ref>{{cite web |url= https://www.genericides.org/trademark/aspirin |title= Has aspirin become a generic trademark? |access-date= 17 February 2021 |website= genericides.org |date= 25 March 2020 |archive-date= 5 March 2021 |archive-url= https://web.archive.org/web/20210305221908/https://genericides.org/trademark/aspirin |url-status= dead }}</ref><ref>{{cite book |title = Scientific style and format: the CBE manual for authors, editors, and publishers | collaboration = CBE Style Manual Committee | vauthors = Huth EJ |publisher = Cambridge University Press |year = 1994 |page = 164 |url = https://books.google.com/books?id=PoFJ-OhE63UC&pg=PA164 |isbn = 978-0-521-47154-1 |url-status = live |archive-url = https://web.archive.org/web/20151015200126/https://books.google.com/books?id=PoFJ-OhE63UC&pg=PA164 |archive-date = 15 October 2015|bibcode = 1994ssfc.book.....S }}</ref> Aspirin, with a capital "A", remains a registered trademark of Bayer in Germany, Canada, Mexico, and in over 80 other countries, for acetylsalicylic acid in all markets, but using different packaging and physical aspects for each.<ref>{{cite news | url=http://www.cbc.ca/news/technology/aspirin-the-versatile-drug-1.822289 | work=CBC News | title=Aspirin: the versatile drug | date=28 May 2009 | url-status=live | archive-url=https://web.archive.org/web/20161106123159/http://www.cbc.ca/news/technology/aspirin-the-versatile-drug-1.822289 | archive-date=6 November 2016}}</ref><ref>{{cite journal | vauthors = Cheng TO | title = The history of aspirin | journal = Texas Heart Institute Journal | volume = 34 | issue = 3 | pages = 392–3 | year = 2007 | pmid = 17948100 | pmc = 1995051 }}</ref> |
||
===Compendial status=== |
===Compendial status=== |
||
| Line 237: | Line 234: | ||
==Medical use== |
==Medical use== |
||
Aspirin is used in the treatment of a number of conditions, including fever, pain, [[rheumatic fever]], and inflammatory conditions, such as [[rheumatoid arthritis]], [[pericarditis]], and [[Kawasaki disease]].<ref name=AHFS/> Lower doses of aspirin have also been shown to reduce the risk of death from a [[myocardial infarction|heart attack]], or the risk of [[stroke]] in people who are at high risk or who have cardiovascular disease, but not in elderly people who are otherwise healthy.<ref name="USFDA-patient-guideline">{{citation-attribution|1={{cite web |title=Aspirin for reducing your risk of heart attack and stroke: know the facts |url=https://www.fda.gov/drugs/safe-daily-use-aspirin/aspirin-reducing-your-risk-heart-attack-and-stroke-know-facts |publisher=U.S. [[Food and Drug Administration]] (FDA) |access-date=26 July 2012 |url-status=live |archive-url=https://web.archive.org/web/20120814182151/https://www.fda.gov/Drugs/ResourcesForYou/Consumers/BuyingUsingMedicineSafely/UnderstandingOver-the-CounterMedicines/SafeDailyUseofAspirin/ucm291433.htm |archive-date=14 August 2012}} }}</ref><ref name="USPSTF-CV">{{citation-attribution|1={{cite web |title=Aspirin for the prevention of cardiovascular disease |url=http://www.uspreventiveservicestaskforce.org/uspstf/uspsasmi.htm |publisher=[[U.S. Preventive Services Task Force]] |access-date=26 July 2012 |url-status=dead |archive-url=https://web.archive.org/web/20120711031337/http://www.uspreventiveservicestaskforce.org/uspstf/uspsasmi.htm |archive-date=11 July 2012}} }}</ref><ref>{{cite journal | vauthors = Seshasai SR, Wijesuriya S, Sivakumaran R, Nethercott S, Erqou S, Sattar N, Ray KK |
Aspirin is used in the treatment of a number of conditions, including fever, pain, [[rheumatic fever]], and inflammatory conditions, such as [[rheumatoid arthritis]], [[pericarditis]], and [[Kawasaki disease]].<ref name=AHFS/> Lower doses of aspirin have also been shown to reduce the risk of death from a [[myocardial infarction|heart attack]], or the risk of [[stroke]] in people who are at high risk or who have cardiovascular disease, but not in elderly people who are otherwise healthy.<ref name="USFDA-patient-guideline">{{citation-attribution|1={{cite web |title=Aspirin for reducing your risk of heart attack and stroke: know the facts |url=https://www.fda.gov/drugs/safe-daily-use-aspirin/aspirin-reducing-your-risk-heart-attack-and-stroke-know-facts |publisher=U.S. [[Food and Drug Administration]] (FDA) |access-date=26 July 2012 |url-status=live |archive-url=https://web.archive.org/web/20120814182151/https://www.fda.gov/Drugs/ResourcesForYou/Consumers/BuyingUsingMedicineSafely/UnderstandingOver-the-CounterMedicines/SafeDailyUseofAspirin/ucm291433.htm |archive-date=14 August 2012}} }}</ref><ref name="USPSTF-CV">{{citation-attribution|1={{cite web |title=Aspirin for the prevention of cardiovascular disease |url=http://www.uspreventiveservicestaskforce.org/uspstf/uspsasmi.htm |publisher=[[U.S. Preventive Services Task Force]] |access-date=26 July 2012 |url-status=dead |archive-url=https://web.archive.org/web/20120711031337/http://www.uspreventiveservicestaskforce.org/uspstf/uspsasmi.htm |archive-date=11 July 2012}} }}</ref><ref>{{cite journal | vauthors = Seshasai SR, Wijesuriya S, Sivakumaran R, Nethercott S, Erqou S, Sattar N, Ray KK | title = Effect of aspirin on vascular and nonvascular outcomes: meta-analysis of randomized controlled trials | journal = Archives of Internal Medicine | volume = 172 | issue = 3 | pages = 209–16 | date = February 2012 | pmid = 22231610 | doi = 10.1001/archinternmed.2011.628 | hdl-access = free | doi-access = free | hdl = 10044/1/34287 | title-link = doi }}</ref><ref name="NEJM-20180916">{{cite journal | vauthors = McNeil JJ, Woods RL, Nelson MR, Reid CM, Kirpach B, Wolfe R, Storey E, Shah RC, Lockery JE, Tonkin AM, Newman AB, Williamson JD, Margolis KL, Ernst ME, Abhayaratna WP, Stocks N, Fitzgerald SM, Orchard SG, Trevaks RE, Beilin LJ, Donnan GA, Gibbs P, Johnston CI, Ryan J, Radziszewska B, Grimm R, Murray AM | title = Effect of Aspirin on Disability-free Survival in the Healthy Elderly | journal = The New England Journal of Medicine | volume = 379 | issue = 16 | pages = 1499–1508 | date = October 2018 | pmid = 30221596 | pmc = 6426126 | doi = 10.1056/NEJMoa1800722 | hdl-access = free | doi-access = free | hdl = 1885/154654 | title-link = doi }}</ref><ref name=NEJM2018CVE>{{cite journal | vauthors = McNeil JJ, Wolfe R, Woods RL, Tonkin AM, Donnan GA, Nelson MR, Reid CM, Lockery JE, Kirpach B, Storey E, Shah RC, Williamson JD, Margolis KL, Ernst ME, Abhayaratna WP, Stocks N, Fitzgerald SM, Orchard SG, Trevaks RE, Beilin LJ, Johnston CI, Ryan J, Radziszewska B, Jelinek M, Malik M, Eaton CB, Brauer D, Cloud G, Wood EM, Mahady SE, Satterfield S, Grimm R, Murray AM | title = Effect of Aspirin on Cardiovascular Events and Bleeding in the Healthy Elderly | journal = The New England Journal of Medicine | volume = 379 | issue = 16 | pages = 1509–1518 | date = October 2018 | pmid = 30221597 | pmc = 6289056 | doi = 10.1056/NEJMoa1805819 | doi-access = free | title-link = doi }}</ref> There is evidence that aspirin is effective at preventing [[colorectal cancer]], though the mechanisms of this effect are unclear.<ref name="Algra 518–27">{{cite journal | vauthors = Algra AM, Rothwell PM | title = Effects of regular aspirin on long-term cancer incidence and metastasis: a systematic comparison of evidence from observational studies versus randomised trials | journal = The Lancet. Oncology | volume = 13 | issue = 5 | pages = 518–27 | date = May 2012 | pmid = 22440112 | doi = 10.1016/S1470-2045(12)70112-2 }}</ref> In the United States, the selective initiation of low-dose aspirin, based on an individualised assessment, has been deemed reasonable for the primary prevention of cardiovascular disease in people aged between 40 and 59 who have a 10% or greater risk of developing cardiovascular disease over the next 10 years and are not at an increased risk of bleeding.<ref>{{cite journal | vauthors = Davidson KW, Barry MJ, Mangione CM, Cabana M, Chelmow D, Coker TR, Davis EM, Donahue KE, Jaén CR, Krist AH, Kubik M, Li L, Ogedegbe G, Pbert L, Ruiz JM, Stevermer J, Tseng CW, Wong JB |date=April 2022 |title=Aspirin Use to Prevent Cardiovascular Disease: US Preventive Services Task Force Recommendation Statement |journal=JAMA |volume=327 |issue=16 |pages=1577–1584 |doi=10.1001/jama.2022.4983 |pmid=35471505 |s2cid=248390304 |doi-access=free }}</ref> |
||
===Pain=== |
===Pain=== |
||
| Line 249: | Line 246: | ||
===Inflammation=== |
===Inflammation=== |
||
Aspirin is used as an [[anti-inflammatory agent]] for both acute and long-term [[inflammation]],<ref name="pmid19597002">{{cite journal | vauthors = Morris T, Stables M, Hobbs A, de Souza P, Colville-Nash P, Warner T, Newson J, Bellingan G, Gilroy DW |
Aspirin is used as an [[anti-inflammatory agent]] for both acute and long-term [[inflammation]],<ref name="pmid19597002">{{cite journal | vauthors = Morris T, Stables M, Hobbs A, de Souza P, Colville-Nash P, Warner T, Newson J, Bellingan G, Gilroy DW | title = Effects of low-dose aspirin on acute inflammatory responses in humans | journal = Journal of Immunology | volume = 183 | issue = 3 | pages = 2089–96 | date = August 2009 | pmid = 19597002 | doi = 10.4049/jimmunol.0900477 | doi-access = free | title-link = doi }}</ref> as well as for the treatment of inflammatory diseases, such as [[rheumatoid arthritis]].<ref name=AHFS /> |
||
===Heart attacks and strokes=== |
===Heart attacks and strokes=== |
||
Aspirin is an important part of the treatment of those who have had a [[myocardial infarction|heart attack]].<ref>{{cite book | title = Myocardial infarction with ST-segment elevation: the acute management of myocardial infarction with ST-segment elevation [Internet] | |
Aspirin is an important part of the treatment of those who have had a [[myocardial infarction|heart attack]].<ref>{{cite book | title = Myocardial infarction with ST-segment elevation: the acute management of myocardial infarction with ST-segment elevation [Internet] | series = NICE Clinical Guidelines | issue = 167 | date = July 2013 | pmid = 25340241 | chapter-url = https://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0071000/ | url-status = live | archive-url = https://web.archive.org/web/20151231192814/http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0071000/ | archive-date = 31 December 2015 | at = 17.2 Aspirin | author1 = National Clinical Guideline Centre (UK) | chapter = Adjunctive pharmacotherapy and associated NICE guidance | publisher = Royal College of Physicians (UK) }}</ref> It is generally not recommended for routine use by people with no other health problems, including those over the age of 70.<ref name="Arnett-2019">{{cite journal | vauthors = Arnett DK, Blumenthal RS, Albert MA, Buroker AB, Goldberger ZD, Hahn EJ, Himmelfarb CD, Khera A, Lloyd-Jones D, McEvoy JW, Michos ED, Miedema MD, Muñoz D, Smith SC, Virani SS, Williams KA, Yeboah J, Ziaeian B | title = 2019 ACC/AHA Guideline on the Primary Prevention of Cardiovascular Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines | journal = Journal of the American College of Cardiology | volume = 74 | issue = 10 | pages = e177–e232 | date = September 2019 | pmid = 30894318 | pmc = 7685565 | doi = 10.1016/j.jacc.2019.03.010 | doi-access = free | title-link = doi }}</ref> |
||
The 2009 Antithrombotic Trialists' Collaboration published in Lancet evaluated the efficacy and safety of low dose aspirin in secondary prevention. In those with prior ischaemic stroke or acute myocardial infarction, daily low dose aspirin was associated with a 19% relative risk reduction of serious cardiovascular events (non-fatal myocardial infarction, non-fatal stroke, or vascular death). This did come at the expense of a 0.19% absolute risk increase in gastrointestinal bleeding; however, the benefits outweigh the hazard risk in this case.{{citation needed|date=April 2023}} Data from previous trials have suggested that weight-based dosing of aspirin has greater benefits in primary prevention of cardiovascular outcomes.<ref name="Lancet2018Dose"/> However, more recent trials were not able to replicate similar outcomes using low dose aspirin in low body weight (<70 kg) in specific subset of population studied i.e. elderly and diabetic population, and more evidence is required to study the effect of high dose aspirin in high body weight (≥70 kg).<ref>{{cite journal | vauthors = Bowman L, Mafham M, Wallendszus K, Stevens W, Buck G, Barton J, Murphy K, Aung T, Haynes R, Cox J, Murawska A, Young A, Lay M, Chen F, Sammons E, Waters E, Adler A, Bodansky J, Farmer A, McPherson R, Neil A, Simpson D, Peto R, Baigent C, Collins R, Parish S, Armitage J |
The 2009 Antithrombotic Trialists' Collaboration published in Lancet evaluated the efficacy and safety of low dose aspirin in secondary prevention. In those with prior ischaemic stroke or acute myocardial infarction, daily low dose aspirin was associated with a 19% relative risk reduction of serious cardiovascular events (non-fatal myocardial infarction, non-fatal stroke, or vascular death). This did come at the expense of a 0.19% absolute risk increase in gastrointestinal bleeding; however, the benefits outweigh the hazard risk in this case.{{citation needed|date=April 2023}} Data from previous trials have suggested that weight-based dosing of aspirin has greater benefits in primary prevention of cardiovascular outcomes.<ref name="Lancet2018Dose"/> However, more recent trials were not able to replicate similar outcomes using low dose aspirin in low body weight (<70 kg) in specific subset of population studied i.e. elderly and diabetic population, and more evidence is required to study the effect of high dose aspirin in high body weight (≥70 kg).<ref>{{cite journal | vauthors = Bowman L, Mafham M, Wallendszus K, Stevens W, Buck G, Barton J, Murphy K, Aung T, Haynes R, Cox J, Murawska A, Young A, Lay M, Chen F, Sammons E, Waters E, Adler A, Bodansky J, Farmer A, McPherson R, Neil A, Simpson D, Peto R, Baigent C, Collins R, Parish S, Armitage J | title = Effects of Aspirin for Primary Prevention in Persons with Diabetes Mellitus | journal = The New England Journal of Medicine | volume = 379 | issue = 16 | pages = 1529–1539 | date = October 2018 | pmid = 30146931 | doi = 10.1056/NEJMoa1804988 | doi-access = free | title-link = doi }}</ref><ref>{{cite journal | vauthors = McNeil JJ, Wolfe R, Woods RL, Tonkin AM, Donnan GA, Nelson MR, Reid CM, Lockery JE, Kirpach B, Storey E, Shah RC, Williamson JD, Margolis KL, Ernst ME, Abhayaratna WP, Stocks N, Fitzgerald SM, Orchard SG, Trevaks RE, Beilin LJ, Johnston CI, Ryan J, Radziszewska B, Jelinek M, Malik M, Eaton CB, Brauer D, Cloud G, Wood EM, Mahady SE, Satterfield S, Grimm R, Murray AM | title = Effect of Aspirin on Cardiovascular Events and Bleeding in the Healthy Elderly | journal = The New England Journal of Medicine | volume = 379 | issue = 16 | pages = 1509–1518 | date = October 2018 | pmid = 30221597 | doi = 10.1056/NEJMoa1805819 | pmc = 6289056 | doi-access = free | title-link = doi }}</ref><ref>{{cite journal | vauthors = Woods RL, Polekhina G, Wolfe R, Nelson MR, Ernst ME, Reid CM, Shah RC, Lockery JE, Orchard SG, Murray AM, McNeil JJ | title = No Modulation of the Effect of Aspirin by Body Weight in Healthy Older Men and Women | journal = Circulation | volume = 141 | issue = 13 | pages = 1110–1112 | date = March 2020 | pmid = 32223674 | doi = 10.1161/CIRCULATIONAHA.119.044142 | pmc = 7286412 | doi-access = free | title-link = doi }}</ref> |
||
After [[percutaneous coronary intervention]]s (PCIs), such as the placement of a [[coronary artery]] [[stent]], a U.S. [[Agency for Healthcare Research and Quality]] guideline recommends that aspirin be taken indefinitely.<ref>{{cite web | author = National Guideline Clearinghouse (NGC) |title=2011 ACCF/AHA/SCAI guideline for percutaneous coronary artery intervention. A report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines and the Society for Cardiovascular Angiography and Interventions |url=http://www.guideline.gov/content.aspx?id=34980 |url-status=dead |archive-url=https://web.archive.org/web/20120813064712/http://www.guideline.gov/content.aspx?id=34980 |archive-date=13 August 2012 |access-date=28 August 2012 |publisher=United States [[Agency for Healthcare Research and Quality]] (AHRQ)}}</ref> Frequently, aspirin is combined with an [[ADP receptor inhibitor]], such as [[clopidogrel]], [[prasugrel]], or [[ticagrelor]] to prevent [[Thrombosis|blood clots]]. This is called dual antiplatelet therapy (DAPT). Duration of DAPT was advised in the United States and European Union guidelines after the CURE |
After [[percutaneous coronary intervention]]s (PCIs), such as the placement of a [[coronary artery]] [[stent]], a U.S. [[Agency for Healthcare Research and Quality]] guideline recommends that aspirin be taken indefinitely.<ref>{{cite web | author = National Guideline Clearinghouse (NGC) |title=2011 ACCF/AHA/SCAI guideline for percutaneous coronary artery intervention. A report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines and the Society for Cardiovascular Angiography and Interventions |url=http://www.guideline.gov/content.aspx?id=34980 |url-status=dead |archive-url=https://web.archive.org/web/20120813064712/http://www.guideline.gov/content.aspx?id=34980 |archive-date=13 August 2012 |access-date=28 August 2012 |publisher=United States [[Agency for Healthcare Research and Quality]] (AHRQ)}}</ref> Frequently, aspirin is combined with an [[ADP receptor inhibitor]], such as [[clopidogrel]], [[prasugrel]], or [[ticagrelor]] to prevent [[Thrombosis|blood clots]]. This is called dual antiplatelet therapy (DAPT). Duration of DAPT was advised in the United States and European Union guidelines after the CURE<ref>{{cite journal |vauthors=Yusuf S, Zhao F, Mehta SR, Chrolavicius S, Tognoni G, Fox KK |date=August 2001 |title=Effects of clopidogrel in addition to aspirin in patients with acute coronary syndromes without ST-segment elevation |url=http://real.mtak.hu/12922/1/1277670.pdf |journal=The New England Journal of Medicine |volume=345 |issue=7 |pages=494–502 |doi=10.1056/nejmoa010746 |pmid=11519503|s2cid=15459216 }}</ref> and PRODIGY<ref>{{cite journal |vauthors=Costa F, Vranckx P, Leonardi S, Moscarella E, Ando G, Calabro P, Oreto G, Zijlstra F, Valgimigli M |date=May 2015 |title=Impact of clinical presentation on ischaemic and bleeding outcomes in patients receiving 6- or 24-month duration of dual-antiplatelet therapy after stent implantation: a pre-specified analysis from the PRODIGY (Prolonging Dual-Antiplatelet Treatment After Grading Stent-Induced Intimal Hyperplasia) trial |journal=European Heart Journal |volume=36 |issue=20 |pages=1242–51 |doi=10.1016/s0735-1097(15)61590-x |pmid=25718355 |doi-access=free |title-link=doi}}</ref> studies. In 2020, the systematic review and network meta-analysis from Khan et al.<ref>{{cite journal |vauthors=Khan SU, Singh M, Valavoor S, Khan MU, Lone AN, Khan MZ, Khan MS, Mani P, Kapadia SR, Michos ED, Stone GW, Kalra A, Bhatt DL |date=October 2020 |title=Dual Antiplatelet Therapy After Percutaneous Coronary Intervention and Drug-Eluting Stents: A Systematic Review and Network Meta-Analysis |journal=Circulation |volume=142 |issue=15 |pages=1425–1436 |doi=10.1161/CIRCULATIONAHA.120.046308 |pmc=7547897 |pmid=32795096}}</ref> showed promising benefits of short-term (< 6 months) DAPT followed by P2Y12 inhibitors in selected patients, as well as the benefits of extended-term (> 12 months) DAPT in high risk patients. In conclusion, the optimal duration of DAPT after PCIs should be personalized after outweighing each patient's risks of ischemic events and risks of bleeding events with consideration of multiple patient-related and procedure-related factors. Moreover, aspirin should be continued indefinitely after DAPT is complete.<ref>{{cite journal |vauthors=Capodanno D, Alfonso F, Levine GN, Valgimigli M, Angiolillo DJ |date=December 2018 |title=ACC/AHA Versus ESC Guidelines on Dual Antiplatelet Therapy: JACC Guideline Comparison |journal=Journal of the American College of Cardiology |volume=72 |issue=23 Pt A |pages=2915–2931 |doi=10.1016/j.jacc.2018.09.057 |pmid=30522654 |doi-access=free |title-link=doi}}</ref><ref>{{cite journal |vauthors=Levine GN, Bates ER, Bittl JA, Brindis RG, Fihn SD, Fleisher LA, Granger CB, Lange RA, Mack MJ, Mauri L, Mehran R, Mukherjee D, Newby LK, O'Gara PT, Sabatine MS, Smith PK, Smith SC |date=September 2016 |title=2016 ACC/AHA Guideline Focused Update on Duration of Dual Antiplatelet Therapy in Patients With Coronary Artery Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines |journal=Journal of the American College of Cardiology |volume=68 |issue=10 |pages=1082–115 |doi=10.1016/j.jacc.2016.03.513 |pmid=27036918 |doi-access=free |title-link=doi}}</ref><ref>{{cite journal |vauthors=Valgimigli M, Bueno H, Byrne RA, Collet JP, Costa F, Jeppsson A, Jüni P, Kastrati A, Kolh P, Mauri L, Montalescot G, Neumann FJ, Petricevic M, Roffi M, Steg PG, Windecker S, Zamorano JL, Levine GN |date=January 2018 |title=2017 ESC focused update on dual antiplatelet therapy in coronary artery disease developed in collaboration with EACTS: The Task Force for dual antiplatelet therapy in coronary artery disease of the European Society of Cardiology (ESC) and of the European Association for Cardio-Thoracic Surgery (EACTS) |journal=European Heart Journal |volume=39 |issue=3 |pages=213–260 |doi=10.1093/eurheartj/ehx419 |pmid=28886622 |doi-access=free |title-link=doi}}</ref> |
||
The status of the use of aspirin for the primary prevention in cardiovascular disease is conflicting and inconsistent, with recent changes from previously recommending it widely decades ago, and that some referenced newer trials in clinical guidelines show less of benefit of adding aspirin alongside other anti-hypertensive and cholesterol lowering therapies.<ref name="Arnett-2019" /><ref name="Visseren-2021">{{cite journal | vauthors = Visseren FL, Mach F, Smulders YM, Carballo D, Koskinas KC, Bäck M, Benetos A, Biffi A, Boavida JM, Capodanno D, Cosyns B, Crawford C, Davos CH, Desormais I, Di Angelantonio E, Franco OH, Halvorsen S, Hobbs FD, Hollander M, Jankowska EA, Michal M, Sacco S, Sattar N, Tokgozoglu L, Tonstad S, Tsioufis KP, van Dis I, van Gelder IC, Wanner C, Williams B |
The status of the use of aspirin for the primary prevention in cardiovascular disease is conflicting and inconsistent, with recent changes from previously recommending it widely decades ago, and that some referenced newer trials in clinical guidelines show less of benefit of adding aspirin alongside other anti-hypertensive and cholesterol lowering therapies.<ref name="Arnett-2019" /><ref name="Visseren-2021">{{cite journal | vauthors = Visseren FL, Mach F, Smulders YM, Carballo D, Koskinas KC, Bäck M, Benetos A, Biffi A, Boavida JM, Capodanno D, Cosyns B, Crawford C, Davos CH, Desormais I, Di Angelantonio E, Franco OH, Halvorsen S, Hobbs FD, Hollander M, Jankowska EA, Michal M, Sacco S, Sattar N, Tokgozoglu L, Tonstad S, Tsioufis KP, van Dis I, van Gelder IC, Wanner C, Williams B | title = 2021 ESC Guidelines on cardiovascular disease prevention in clinical practice | journal = European Heart Journal | volume = 42 | issue = 34 | pages = 3227–3337 | date = September 2021 | pmid = 34458905 | doi = 10.1093/eurheartj/ehab484 | doi-access = free }}</ref> The ASCEND study demonstrated that in high-bleeding risk diabetics with no prior cardiovascular disease, there is no overall clinical benefit (12% decrease in risk of ischaemic events v/s 29% increase in GI bleeding) of low dose aspirin in preventing the serious vascular events over a period of 7.4 years. Similarly, the results of the ARRIVE study also showed no benefit of same dose of aspirin in reducing the time to first cardiovascular outcome in patients with moderate risk of cardiovascular disease over a period of five years. Aspirin has also been suggested as a component of a [[polypill]] for prevention of cardiovascular disease.<ref name="pmid16100022">{{cite journal |vauthors=Norris JW |date=September 2005 |title=Antiplatelet agents in secondary prevention of stroke: a perspective |journal=Stroke |volume=36 |issue=9 |pages=2034–6 |doi=10.1161/01.STR.0000177887.14339.46 |pmid=16100022 |doi-access=free |title-link=doi}}</ref><ref name="pmid16603580">{{cite journal |vauthors=Sleight P, Pouleur H, Zannad F |date=July 2006 |title=Benefits, challenges, and registerability of the polypill |journal=European Heart Journal |volume=27 |issue=14 |pages=1651–6 |doi=10.1093/eurheartj/ehi841 |pmid=16603580 |doi-access=free |title-link=doi}}</ref> Complicating the use of aspirin for prevention is the phenomenon of aspirin resistance.<ref name="pmid16364973">{{cite journal |vauthors=Wang TH, Bhatt DL, Topol EJ |date=March 2006 |title=Aspirin and clopidogrel resistance: an emerging clinical entity |journal=European Heart Journal |volume=27 |issue=6 |pages=647–54 |doi=10.1093/eurheartj/ehi684 |pmid=16364973 |doi-access=free |title-link=doi}}</ref><ref name="pmid20944898">{{cite journal |vauthors=Oliveira DC, Silva RF, Silva DJ, Lima VC |date=September 2010 |title=Aspirin resistance: fact or fiction? |journal=Arquivos Brasileiros de Cardiologia |volume=95 |issue=3 |pages=e91-4 |doi=10.1590/S0066-782X2010001300024 |pmid=20944898 |doi-access=free |title-link=doi}}</ref> For people who are resistant, aspirin's efficacy is reduced.<ref name="pmid21306212">{{cite journal |vauthors=Topçuoglu MA, Arsava EM, Ay H |date=February 2011 |title=Antiplatelet resistance in stroke |journal=Expert Review of Neurotherapeutics |volume=11 |issue=2 |pages=251–63 |doi=10.1586/ern.10.203 |pmc=3086673 |pmid=21306212}}</ref> Some authors have suggested testing regimens to identify people who are resistant to aspirin.<ref name="pmid19576352">{{cite journal |vauthors=Ben-Dor I, Kleiman NS, Lev E |date=July 2009 |title=Assessment, mechanisms, and clinical implication of variability in platelet response to aspirin and clopidogrel therapy |journal=The American Journal of Cardiology |volume=104 |issue=2 |pages=227–33 |doi=10.1016/j.amjcard.2009.03.022 |pmid=19576352}}</ref> |
||
As of {{as of|2022|April|lc=n|alt=|bare=yes}}, the [[United States Preventive Services Task Force]] (USPSTF) determined that there was a "small net benefit" for patients aged 40–59 with a 10% or greater 10-year cardiovascular disease (CVD) risk, and "no net benefit" for patients aged over 60.<ref>{{citation-attribution|{{cite web | title=Recommendation: Aspirin Use to Prevent Cardiovascular Disease: Preventive Medication | website=United States Preventive Services Taskforce | date=23 November 2020 | url=https://www.uspreventiveservicestaskforce.org/uspstf/recommendation/aspirin-to-prevent-cardiovascular-disease-preventive-medication | access-date=5 May 2022}}}}</ref><ref>{{cite journal | vauthors = Davidson KW, Barry MJ, Mangione CM, Cabana M, Chelmow D, Coker TR, Davis EM, Donahue KE, Jaén CR, Krist AH, Kubik M, Li L, Ogedegbe G, Pbert L, Ruiz JM, Stevermer J, Tseng CW, Wong JB |
As of {{as of|2022|April|lc=n|alt=|bare=yes}}, the [[United States Preventive Services Task Force]] (USPSTF) determined that there was a "small net benefit" for patients aged 40–59 with a 10% or greater 10-year cardiovascular disease (CVD) risk, and "no net benefit" for patients aged over 60.<ref>{{citation-attribution|{{cite web | title=Recommendation: Aspirin Use to Prevent Cardiovascular Disease: Preventive Medication | website=United States Preventive Services Taskforce | date=23 November 2020 | url=https://www.uspreventiveservicestaskforce.org/uspstf/recommendation/aspirin-to-prevent-cardiovascular-disease-preventive-medication | access-date=5 May 2022}}}}</ref><ref>{{cite journal | vauthors = Davidson KW, Barry MJ, Mangione CM, Cabana M, Chelmow D, Coker TR, Davis EM, Donahue KE, Jaén CR, Krist AH, Kubik M, Li L, Ogedegbe G, Pbert L, Ruiz JM, Stevermer J, Tseng CW, Wong JB | title = Aspirin Use to Prevent Cardiovascular Disease: US Preventive Services Task Force Recommendation Statement | journal = JAMA | volume = 327 | issue = 16 | pages = 1577–1584 | date = April 2022 | pmid = 35471505 | doi = 10.1001/jama.2022.4983 | title-link = doi | doi-access = free }}</ref><ref>{{cite news | vauthors = Aubrey A, Stone W |date=26 April 2022 |title=Older adults shouldn't start a routine of daily aspirin, task force says |website=[[NPR]] |url=https://www.npr.org/sections/health-shots/2022/04/26/1094881056/older-adults-shouldnt-start-a-routine-of-daily-aspirin-task-force-says}}</ref> Determining the net benefit was based on balancing the risk reduction of taking aspirin for heart attacks and ischaemic strokes, with the increased risk of [[gastrointestinal bleeding]], [[Intracranial hemorrhage|intracranial bleeding]], and [[hemorrhagic stroke]]s. Their recommendations state that age changes the risk of the medicine, with the magnitude of the benefit of aspirin coming from starting at a younger age, while the risk of bleeding, while small, increases with age, particular for adults over 60, and can be compounded by other risk factors such as [[diabetes]] and a history of gastrointestinal bleeding. As a result, the USPSTF suggests that "people ages 40 to 59 who are at higher risk for CVD should decide with their clinician whether to start taking aspirin; people 60 or older should not start taking aspirin to prevent a first heart attack or stroke." Primary prevention guidelines from {{as of|2019|September|lc=n|alt=|bare=yes}} made by the [[American College of Cardiology]] and the [[American Heart Association]] state they might consider aspirin for patients aged 40–69 with a higher risk of atherosclerotic CVD, without an increased bleeding risk, while stating they would not recommend aspirin for patients aged over 70 or adults of any age with an increased bleeding risk.<ref name="Arnett-2019" /> They state a CVD risk estimation and a risk discussion should be done before starting on aspirin, while stating aspirin should be used "infrequently in the routine primary prevention of (atherosclerotic CVD) because of lack of net benefit". As of {{as of|2021|August|lc=n|alt=|bare=yes}}, the [[European Society of Cardiology]] made similar recommendations; considering aspirin specifically to patients aged less than 70 at high or very high CVD risk, without any clear contraindications, on a case-by-case basis considering both ischemic risk and bleeding risk.<ref name="Visseren-2021" /> |
||
===Cancer prevention=== |
===Cancer prevention=== |
||
Aspirin may reduce the overall risk of both getting cancer and dying from cancer.<ref name=Cuz2014>{{cite journal | vauthors = Cuzick J, Thorat MA, Bosetti C, Brown PH, Burn J, Cook NR, Ford LG, Jacobs EJ, Jankowski JA, La Vecchia C, Law M, Meyskens F, Rothwell PM, Senn HJ, Umar A |
Aspirin may reduce the overall risk of both getting cancer and dying from cancer.<ref name=Cuz2014>{{cite journal | vauthors = Cuzick J, Thorat MA, Bosetti C, Brown PH, Burn J, Cook NR, Ford LG, Jacobs EJ, Jankowski JA, La Vecchia C, Law M, Meyskens F, Rothwell PM, Senn HJ, Umar A | title = Estimates of benefits and harms of prophylactic use of aspirin in the general population | journal = Annals of Oncology | volume = 26 | issue = 1 | pages = 47–57 | date = January 2015 | pmid = 25096604 | pmc = 4269341 | doi = 10.1093/annonc/mdu225 }}</ref> There is substantial evidence for lowering the risk of [[colorectal cancer]] (CRC),<ref name="Algra 518–27"/><ref>{{cite journal | vauthors = Manzano A, Pérez-Segura P | title = Colorectal cancer chemoprevention: is this the future of colorectal cancer prevention? | journal = TheScientificWorldJournal | volume = 2012 | pages = 327341 | date = 29 April 2012 | pmid = 22649288 | pmc = 3353298 | doi = 10.1100/2012/327341 | doi-access = free }}</ref><ref>{{cite journal | vauthors = Chan AT, Arber N, Burn J, Chia WK, Elwood P, Hull MA, Logan RF, Rothwell PM, Schrör K, Baron JA | title = Aspirin in the chemoprevention of colorectal neoplasia: an overview | journal = Cancer Prevention Research | volume = 5 | issue = 2 | pages = 164–78 | date = February 2012 | pmid = 22084361 | pmc = 3273592 | doi = 10.1158/1940-6207.CAPR-11-0391 }}</ref><ref>{{cite journal | vauthors = Thun MJ, Jacobs EJ, Patrono C | title = The role of aspirin in cancer prevention | journal = Nature Reviews. Clinical Oncology | volume = 9 | issue = 5 | pages = 259–67 | date = April 2012 | pmid = 22473097 | doi = 10.1038/nrclinonc.2011.199 | s2cid = 3332999 }}</ref> but aspirin must be taken for at least 10–20 years to see this benefit.<ref name="Richman2017">{{cite journal | vauthors = Richman IB, Owens DK | title = Aspirin for Primary Prevention | journal = The Medical Clinics of North America | volume = 101 | issue = 4 | pages = 713–724 | date = July 2017 | pmid = 28577622 | doi = 10.1016/j.mcna.2017.03.004 | type = Review }}</ref> It may also slightly reduce the risk of [[endometrial cancer]]<ref>{{cite journal | vauthors = Verdoodt F, Friis S, Dehlendorff C, Albieri V, Kjaer SK | title = Non-steroidal anti-inflammatory drug use and risk of endometrial cancer: A systematic review and meta-analysis of observational studies | journal = Gynecologic Oncology | volume = 140 | issue = 2 | pages = 352–8 | date = February 2016 | pmid = 26701413 | doi = 10.1016/j.ygyno.2015.12.009 }}</ref> and [[prostate cancer]].<ref>{{cite journal | vauthors = Bosetti C, Rosato V, Gallus S, Cuzick J, La Vecchia C | title = Aspirin and cancer risk: a quantitative review to 2011 | journal = Annals of Oncology | volume = 23 | issue = 6 | pages = 1403–15 | date = June 2012 | pmid = 22517822 | doi = 10.1093/annonc/mds113 | doi-access = free | title-link = doi }}</ref> |
||
Some conclude the benefits are greater than the risks due to bleeding in those at average risk.<ref name=Cuz2014/> Others are unclear if the benefits are greater than the risk.<ref>{{cite journal |
Some conclude the benefits are greater than the risks due to bleeding in those at average risk.<ref name=Cuz2014/> Others are unclear if the benefits are greater than the risk.<ref>{{cite journal|vauthors=Sutcliffe P, Connock M, Gurung T, Freeman K, Johnson S, Kandala NB, Grove A, Gurung B, Morrow S, Clarke A |date=September 2013|title=Aspirin for prophylactic use in the primary prevention of cardiovascular disease and cancer: a systematic review and overview of reviews|journal=[[Health Technology Assessment (journal)|Health Technology Assessment]]|volume=17|issue=43|pages=1–253|doi=10.3310/hta17430|pmc=4781046|pmid=24074752}}</ref><ref>{{cite journal | vauthors = Kim SE | title = The benefit-risk consideration in long-term use of alternate-day, low dose aspirin: focus on colorectal cancer prevention | journal = Annals of Gastroenterology | volume = 27 | issue = 1 | pages = 87–88 | date = 2014 | pmid = 24714632 | pmc = 3959543 }}</ref> Given this uncertainty, the 2007 [[United States Preventive Services Task Force]] (USPSTF) guidelines on this topic recommended against the use of aspirin for prevention of CRC in people with average risk.<ref name="USPSTF 2007">{{cite journal | title = Routine aspirin or nonsteroidal anti-inflammatory drugs for the primary prevention of colorectal cancer: U.S. Preventive Services Task Force recommendation statement | journal = Annals of Internal Medicine | volume = 146 | issue = 5 | pages = 361–4 | date = March 2007 | pmid = 17339621 | doi = 10.7326/0003-4819-146-5-200703060-00008 | doi-access = free | author1 = U.S. Preventive Services Task Force | title-link = doi }}</ref> Nine years later however, the USPSTF issued a grade B recommendation for the use of low-dose aspirin (75 to 100{{nbsp}}mg/day) "for the primary prevention of CVD [cardiovascular disease] and CRC in adults 50 to 59 years of age who have a 10% or greater 10-year CVD risk, are not at increased risk for bleeding, have a life expectancy of at least 10 years, and are willing to take low-dose aspirin daily for at least 10 years".<ref name="USPSTF 2016">{{cite journal |vauthors=Bibbins-Domingo K |date=June 2016 |title=Aspirin Use for the Primary Prevention of Cardiovascular Disease and Colorectal Cancer: U.S. Preventive Services Task Force Recommendation Statement |journal=Annals of Internal Medicine |volume=164 |issue=12 |pages=836–45 |doi=10.7326/m16-0577 |pmid=27064677 |doi-access=free |title-link=doi}} |
||
* {{lay source|template=cite web|url=https://annals.org/aim/fullarticle/2513180/aspirin-use-primary-prevention-cardiovascular-disease-colorectal-cancer-recommendations-from|title=Who developed these recommendations?|date=21 June 2016|website=Annals of Internal Medicine}}</ref> |
* {{lay source|template=cite web|url=https://annals.org/aim/fullarticle/2513180/aspirin-use-primary-prevention-cardiovascular-disease-colorectal-cancer-recommendations-from|title=Who developed these recommendations?|date=21 June 2016|website=Annals of Internal Medicine}}</ref> |
||
A meta-analysis through 2019 said that there was an association between taking aspirin and lower risk of cancer of the colorectum, esophagus, and stomach.<ref>{{cite journal | vauthors = Bosetti C, Santucci C, Gallus S, Martinetti M, La Vecchia C | title = Aspirin and the risk of colorectal and other digestive tract cancers: an updated meta-analysis through 2019 | journal = Annals of Oncology | volume = 31 | issue = 5 | pages = 558–568 | date = May 2020 | pmid = 32272209 | doi = 10.1016/j.annonc.2020.02.012 | quote = The present comprehensive meta-analysis supports and further quantifies the inverse association between regular aspirin use and the risk of colorectal and other digestive tract cancers, including some rare ones. The favorable effect of aspirin increases with longer duration of use, and, for colorectal cancer, with increasing dose. | doi-access = free | title-link = doi }}</ref> |
A meta-analysis through 2019 said that there was an association between taking aspirin and lower risk of cancer of the colorectum, esophagus, and stomach.<ref>{{cite journal | vauthors = Bosetti C, Santucci C, Gallus S, Martinetti M, La Vecchia C | title = Aspirin and the risk of colorectal and other digestive tract cancers: an updated meta-analysis through 2019 | journal = Annals of Oncology | volume = 31 | issue = 5 | pages = 558–568 | date = May 2020 | pmid = 32272209 | doi = 10.1016/j.annonc.2020.02.012 | quote = The present comprehensive meta-analysis supports and further quantifies the inverse association between regular aspirin use and the risk of colorectal and other digestive tract cancers, including some rare ones. The favorable effect of aspirin increases with longer duration of use, and, for colorectal cancer, with increasing dose. | doi-access = free | title-link = doi | hdl = 2434/730600 | hdl-access = free }}</ref> |
||
In 2021, the U.S. Preventive services Task Force raised questions about the use of aspirin in cancer prevention. It notes the results of the 2018 ASPREE (Aspirin in Reducing Events in the Elderly) Trial, in which the risk of cancer-related death was higher in the aspirin-treated group than in the placebo group.<ref>{{cite journal | vauthors = McNeil JJ, Nelson MR, Woods RL, Lockery JE, Wolfe R, Reid CM, Kirpach B, Shah RC, Ives DG, Storey E, Ryan J, Tonkin AM, Newman AB, Williamson JD, Margolis KL, Ernst ME, Abhayaratna WP, Stocks N, Fitzgerald SM, Orchard SG, Trevaks RE, Beilin LJ, Donnan GA, Gibbs P, Johnston CI, Radziszewska B, Grimm R, Murray AM |
In 2021, the U.S. Preventive services Task Force raised questions about the use of aspirin in cancer prevention. It notes the results of the 2018 ASPREE (Aspirin in Reducing Events in the Elderly) Trial, in which the risk of cancer-related death was higher in the aspirin-treated group than in the placebo group.<ref>{{cite journal | vauthors = McNeil JJ, Nelson MR, Woods RL, Lockery JE, Wolfe R, Reid CM, Kirpach B, Shah RC, Ives DG, Storey E, Ryan J, Tonkin AM, Newman AB, Williamson JD, Margolis KL, Ernst ME, Abhayaratna WP, Stocks N, Fitzgerald SM, Orchard SG, Trevaks RE, Beilin LJ, Donnan GA, Gibbs P, Johnston CI, Radziszewska B, Grimm R, Murray AM | title = Effect of Aspirin on All-Cause Mortality in the Healthy Elderly | journal = The New England Journal of Medicine | volume = 379 | issue = 16 | pages = 1519–1528 | date = October 2018 | pmid = 30221595 | pmc = 6433466 | doi = 10.1056/NEJMoa1803955 }}</ref> |
||
===Psychiatry=== |
===Psychiatry=== |
||
====Bipolar disorder==== |
====Bipolar disorder==== |
||
Aspirin, along with several other agents with anti-inflammatory properties, has been repurposed as an add-on treatment for depressive episodes in subjects with [[bipolar disorder]] in light of the possible role of inflammation in the pathogenesis of severe mental disorders.<ref name="repurposed2021">{{cite journal | vauthors = Bartoli F, Cavaleri D, Bachi B, Moretti F, Riboldi I, Crocamo C, Carrà G | title = Repurposed drugs as adjunctive treatments for mania and bipolar depression: A meta-review and critical appraisal of meta-analyses of randomized placebo-controlled trials | journal = Journal of Psychiatric Research | volume = 143 | pages = 230–238 | date = November 2021 | pmid = 34509090 | doi = 10.1016/j.jpsychires.2021.09.018 | s2cid = 237485915 }}</ref> A 2022 systematic review concluded that aspirin exposure reduced the risk of depression in a pooled cohort of three studies (HR 0.624, 95% CI: 0.0503, 1.198, P=0.033). However, further high-quality, longer-duration, double-blind randomized controlled trials (RCTs) are needed to determine whether aspirin is an effective add-on treatment for bipolar depression.<ref>{{cite journal | vauthors = Dominiak M, Gędek A, Sikorska M, Mierzejewski P, Wojnar M, Antosik-Wójcińska AZ | title = Acetylsalicylic Acid and Mood Disorders: A Systematic Review | journal = Pharmaceuticals | volume = 16 | issue = 1 | pages = 67 | date = December 2022 | pmid = 36678565 | pmc = 9861965 | doi = 10.3390/ph16010067 | doi-access = free }}</ref><ref>{{cite journal | vauthors = Savitz JB, Teague TK, Misaki M, Macaluso M, Wurfel BE, Meyer M, Drevets D, Yates W, Gleason O, Drevets WC, Preskorn SH |
Aspirin, along with several other agents with anti-inflammatory properties, has been repurposed as an add-on treatment for depressive episodes in subjects with [[bipolar disorder]] in light of the possible role of inflammation in the pathogenesis of severe mental disorders.<ref name="repurposed2021">{{cite journal | vauthors = Bartoli F, Cavaleri D, Bachi B, Moretti F, Riboldi I, Crocamo C, Carrà G | title = Repurposed drugs as adjunctive treatments for mania and bipolar depression: A meta-review and critical appraisal of meta-analyses of randomized placebo-controlled trials | journal = Journal of Psychiatric Research | volume = 143 | pages = 230–238 | date = November 2021 | pmid = 34509090 | doi = 10.1016/j.jpsychires.2021.09.018 | s2cid = 237485915 }}</ref> A 2022 systematic review concluded that aspirin exposure reduced the risk of depression in a pooled cohort of three studies (HR 0.624, 95% CI: 0.0503, 1.198, P=0.033). However, further high-quality, longer-duration, double-blind randomized controlled trials (RCTs) are needed to determine whether aspirin is an effective add-on treatment for bipolar depression.<ref>{{cite journal | vauthors = Dominiak M, Gędek A, Sikorska M, Mierzejewski P, Wojnar M, Antosik-Wójcińska AZ | title = Acetylsalicylic Acid and Mood Disorders: A Systematic Review | journal = Pharmaceuticals | volume = 16 | issue = 1 | pages = 67 | date = December 2022 | pmid = 36678565 | pmc = 9861965 | doi = 10.3390/ph16010067 | doi-access = free }}</ref><ref>{{cite journal | vauthors = Savitz JB, Teague TK, Misaki M, Macaluso M, Wurfel BE, Meyer M, Drevets D, Yates W, Gleason O, Drevets WC, Preskorn SH | title = Treatment of bipolar depression with minocycline and/or aspirin: an adaptive, 2×2 double-blind, randomized, placebo-controlled, phase IIA clinical trial | journal = Translational Psychiatry | volume = 8 | issue = 1 | pages = 27 | date = January 2018 | pmid = 29362444 | pmc = 5802452 | doi = 10.1038/s41398-017-0073-7 }}</ref><ref>{{cite journal | vauthors = Bauer IE, Green C, Colpo GD, Teixeira AL, Selvaraj S, Durkin K, Zunta-Soares GB, Soares JC | title = A Double-Blind, Randomized, Placebo-Controlled Study of Aspirin and N-Acetylcysteine as Adjunctive Treatments for Bipolar Depression | journal = The Journal of Clinical Psychiatry | volume = 80 | issue = 1 | date = December 2018 | pmid = 30549489 | doi = 10.4088/JCP.18m12200 | s2cid = 56483705 }}</ref> Thus, notwithstanding the biological rationale, the clinical perspectives of aspirin and anti-inflammatory agents in the treatment of bipolar depression remain uncertain.<ref name="repurposed2021"/> |
||
====Dementia==== |
====Dementia==== |
||
Although cohort and longitudinal studies have shown low-dose aspirin has a greater likelihood of reducing the incidence of dementia, numerous randomized controlled trials have not validated this.<ref>{{cite journal | vauthors = Li H, Li W, Zhang X, Ma XC, Zhang RW | title = Aspirin Use on Incident Dementia and Mild Cognitive Decline: A Systematic Review and Meta-Analysis | journal = Frontiers in Aging Neuroscience | volume = 12 | pages = 578071 | date = 2021 |
Although cohort and longitudinal studies have shown low-dose aspirin has a greater likelihood of reducing the incidence of dementia, numerous randomized controlled trials have not validated this.<ref>{{cite journal | vauthors = Li H, Li W, Zhang X, Ma XC, Zhang RW | title = Aspirin Use on Incident Dementia and Mild Cognitive Decline: A Systematic Review and Meta-Analysis | journal = Frontiers in Aging Neuroscience | volume = 12 | pages = 578071 | date = 4 February 2021 | pmid = 33613260 | pmc = 7890199 | doi = 10.3389/fnagi.2020.578071 | doi-access = free }}</ref><ref>{{cite journal | vauthors = Veronese N, Stubbs B, Maggi S, Thompson T, Schofield P, Muller C, Tseng PT, Lin PY, Carvalho AF, Solmi M | title = Low-Dose Aspirin Use and Cognitive Function in Older Age: A Systematic Review and Meta-analysis | journal = Journal of the American Geriatrics Society | volume = 65 | issue = 8 | pages = 1763–1768 | date = August 2017 | pmid = 28425093 | pmc = 6810633 | doi = 10.1111/jgs.14883 }}</ref> |
||
==== Schizophrenia ==== |
==== Schizophrenia ==== |
||
| Line 284: | Line 281: | ||
===Other uses=== |
===Other uses=== |
||
Aspirin is a first-line treatment for the fever and joint-pain symptoms of [[rheumatic fever|acute rheumatic fever]]. The therapy often lasts for one to two weeks, and is rarely indicated for longer periods. After fever and pain have subsided, the aspirin is no longer necessary, since it does not decrease the incidence of heart complications and residual rheumatic heart disease.<ref name=NHFA>{{cite web |url=http://www.racgp.org.au/Content/NavigationMenu/ClinicalResources/RACGPGuidelines/DiagnosisandmanagementofacuterheumaticfeverandrheumaticheartdiseaseinAustralia/NHFA-CSANZ_ARF_RHD_2006.pdf |archive-url=https://web.archive.org/web/20080726052030/http://www.racgp.org.au/Content/NavigationMenu/ClinicalResources/RACGPGuidelines/DiagnosisandmanagementofacuterheumaticfeverandrheumaticheartdiseaseinAustralia/NHFA-CSANZ_ARF_RHD_2006.pdf |archive-date=26 July 2008 |title=Diagnosis and management of acute rheumatic fever and rheumatic heart disease in Australia. An evidence-based review |author=[[National Heart Foundation of Australia]] (RF/RHD guideline development working group) and the Cardiac Society of Australia and New Zealand |year=2006 |publisher=National Heart Foundation of Australia |pages=33–37}}</ref><ref>{{cite journal | vauthors = Saxena A, Kumar RK, Gera RP, Radhakrishnan S, Mishra S, Ahmed Z | title = Consensus guidelines on pediatric acute rheumatic fever and rheumatic heart disease | journal = Indian Pediatrics | volume = 45 | issue = 7 | pages = 565–73 | date = July 2008 | pmid = 18695275 }}</ref> [[Naproxen]] has been shown to be as effective as aspirin and less toxic, but due to the limited clinical experience, naproxen is recommended only as a second-line treatment.<ref name=NHFA/><ref>{{cite journal | vauthors = Hashkes PJ, Tauber T, Somekh E, Brik R, Barash J, Mukamel M, Harel L, Lorber A, Berkovitch M, Uziel Y |
Aspirin is a first-line treatment for the fever and joint-pain symptoms of [[rheumatic fever|acute rheumatic fever]]. The therapy often lasts for one to two weeks, and is rarely indicated for longer periods. After fever and pain have subsided, the aspirin is no longer necessary, since it does not decrease the incidence of heart complications and residual rheumatic heart disease.<ref name=NHFA>{{cite web |url=http://www.racgp.org.au/Content/NavigationMenu/ClinicalResources/RACGPGuidelines/DiagnosisandmanagementofacuterheumaticfeverandrheumaticheartdiseaseinAustralia/NHFA-CSANZ_ARF_RHD_2006.pdf |archive-url=https://web.archive.org/web/20080726052030/http://www.racgp.org.au/Content/NavigationMenu/ClinicalResources/RACGPGuidelines/DiagnosisandmanagementofacuterheumaticfeverandrheumaticheartdiseaseinAustralia/NHFA-CSANZ_ARF_RHD_2006.pdf |archive-date=26 July 2008 |title=Diagnosis and management of acute rheumatic fever and rheumatic heart disease in Australia. An evidence-based review |author=[[National Heart Foundation of Australia]] (RF/RHD guideline development working group) and the Cardiac Society of Australia and New Zealand |year=2006 |publisher=National Heart Foundation of Australia |pages=33–37}}</ref><ref>{{cite journal | vauthors = Saxena A, Kumar RK, Gera RP, Radhakrishnan S, Mishra S, Ahmed Z | title = Consensus guidelines on pediatric acute rheumatic fever and rheumatic heart disease | journal = Indian Pediatrics | volume = 45 | issue = 7 | pages = 565–73 | date = July 2008 | pmid = 18695275 }}</ref> [[Naproxen]] has been shown to be as effective as aspirin and less toxic, but due to the limited clinical experience, naproxen is recommended only as a second-line treatment.<ref name=NHFA/><ref>{{cite journal | vauthors = Hashkes PJ, Tauber T, Somekh E, Brik R, Barash J, Mukamel M, Harel L, Lorber A, Berkovitch M, Uziel Y | title = Naproxen as an alternative to aspirin for the treatment of arthritis of rheumatic fever: a randomized trial | journal = The Journal of Pediatrics | volume = 143 | issue = 3 | pages = 399–401 | date = September 2003 | pmid = 14517527 | doi = 10.1067/S0022-3476(03)00388-3 }}</ref> |
||
Along with rheumatic fever, [[Kawasaki disease]] remains one of the few indications for aspirin use in children<ref>{{cite journal | vauthors = Rowley AH, Shulman ST | title = Pathogenesis and management of Kawasaki disease | journal = Expert Review of Anti-Infective Therapy | volume = 8 | issue = 2 | pages = 197–203 | date = February 2010 | pmid = 20109049 | pmc = 2845298 | doi = 10.1586/eri.09.109 }}</ref> in spite of a lack of high quality evidence for its effectiveness.<ref>{{cite journal | vauthors = Baumer JH, Love SJ, Gupta A, Haines LC, Maconochie I, Dua JS | title = Salicylate for the treatment of Kawasaki disease in children | journal = The Cochrane Database of Systematic Reviews | issue = 4 | pages = CD004175 | date = October 2006 | volume = 2010 | pmid = 17054199 | doi = 10.1002/14651858.CD004175.pub2 | pmc = 8765111 }}</ref> |
Along with rheumatic fever, [[Kawasaki disease]] remains one of the few indications for aspirin use in children<ref>{{cite journal | vauthors = Rowley AH, Shulman ST | title = Pathogenesis and management of Kawasaki disease | journal = Expert Review of Anti-Infective Therapy | volume = 8 | issue = 2 | pages = 197–203 | date = February 2010 | pmid = 20109049 | pmc = 2845298 | doi = 10.1586/eri.09.109 }}</ref> in spite of a lack of high quality evidence for its effectiveness.<ref>{{cite journal | vauthors = Baumer JH, Love SJ, Gupta A, Haines LC, Maconochie I, Dua JS | title = Salicylate for the treatment of Kawasaki disease in children | journal = The Cochrane Database of Systematic Reviews | issue = 4 | pages = CD004175 | date = October 2006 | volume = 2010 | pmid = 17054199 | doi = 10.1002/14651858.CD004175.pub2 | pmc = 8765111 }}</ref> |
||
Low-dose aspirin supplementation has moderate benefits when used for prevention of [[pre-eclampsia]].<ref>{{cite journal | vauthors = Duley L, Meher S, Hunter KE, Seidler AL, Askie LM | title = Antiplatelet agents for preventing pre-eclampsia and its complications | journal = The Cochrane Database of Systematic Reviews | volume = 2019 | issue = 10 | date = October 2019 | pmid = 31684684 | pmc = 6820858 | doi = 10.1002/14651858.CD004659.pub3 }}</ref><ref name=Roberge_2012>{{cite journal | vauthors = Roberge S, Villa P, Nicolaides K, Giguère Y, Vainio M, Bakthi A, Ebrashy A, Bujold E |
Low-dose aspirin supplementation has moderate benefits when used for prevention of [[pre-eclampsia]].<ref>{{cite journal | vauthors = Duley L, Meher S, Hunter KE, Seidler AL, Askie LM | title = Antiplatelet agents for preventing pre-eclampsia and its complications | journal = The Cochrane Database of Systematic Reviews | volume = 2019 | issue = 10 | date = October 2019 | pmid = 31684684 | pmc = 6820858 | doi = 10.1002/14651858.CD004659.pub3 }}</ref><ref name=Roberge_2012>{{cite journal | vauthors = Roberge S, Villa P, Nicolaides K, Giguère Y, Vainio M, Bakthi A, Ebrashy A, Bujold E | title = Early administration of low-dose aspirin for the prevention of preterm and term preeclampsia: a systematic review and meta-analysis | journal = Fetal Diagnosis and Therapy | volume = 31 | issue = 3 | pages = 141–6 | year = 2012 | pmid = 22441437 | doi = 10.1159/000336662 | s2cid = 26372982 | doi-access = free | title-link = doi }}</ref> This benefit is greater when started in early pregnancy.<ref>{{cite journal | vauthors = Roberge S, Nicolaides K, Demers S, Hyett J, Chaillet N, Bujold E | title = The role of aspirin dose on the prevention of preeclampsia and fetal growth restriction: systematic review and meta-analysis | journal = American Journal of Obstetrics and Gynecology | volume = 216 | issue = 2 | pages = 110–120.e6 | date = February 2017 | pmid = 27640943 | doi = 10.1016/j.ajog.2016.09.076 | s2cid = 3079979 }}</ref> |
||
Aspirin has also demonstrated [[Treatment of cancer|anti-tumoral]] effects, via inhibition of the [[PTTG1]] gene, which is often overexpressed in tumors.<ref>{{cite journal|title=Aspirin Mediates Its Antitumoral Effect Through Inhibiting PTTG1 in Pituitary Adenoma|doi=10.1210/clinem/dgac496|doi-access=free|journal=[[The Journal of Clinical Endocrinology and Metabolism]] |
Aspirin has also demonstrated [[Treatment of cancer|anti-tumoral]] effects, via inhibition of the [[PTTG1]] gene, which is often overexpressed in tumors.<ref>{{cite journal|title=Aspirin Mediates Its Antitumoral Effect Through Inhibiting PTTG1 in Pituitary Adenoma|doi=10.1210/clinem/dgac496|doi-access=free|journal=[[The Journal of Clinical Endocrinology and Metabolism]]|vauthors=Szabó B, Németh K, Mészáros K, Krokker L, Likó I, Saskői E, Németh K, Szabó PT, Szücs N, Czirják S, Szalóki G, Patócs A, Butz H|date=5 September 2022|volume=107|issue=11|pages=3066–3079|pmid=36059148 |pmc=9681612 }}</ref> |
||
===Resistance=== |
===Resistance=== |
||
{{see also|Drug tolerance}} |
{{see also|Drug tolerance}} |
||
For some people, aspirin does not have as strong an effect on platelets as for others, an effect known as aspirin-resistance or insensitivity. One study has suggested women are more likely to be resistant than men,<ref>{{cite journal | vauthors = Dorsch MP, Lee JS, Lynch DR, Dunn SP, Rodgers JE, Schwartz T, Colby E, Montague D, Smyth SS |
For some people, aspirin does not have as strong an effect on platelets as for others, an effect known as aspirin-resistance or insensitivity. One study has suggested women are more likely to be resistant than men,<ref>{{cite journal | vauthors = Dorsch MP, Lee JS, Lynch DR, Dunn SP, Rodgers JE, Schwartz T, Colby E, Montague D, Smyth SS | title = Aspirin resistance in patients with stable coronary artery disease with and without a history of myocardial infarction | journal = The Annals of Pharmacotherapy | volume = 41 | issue = 5 | pages = 737–41 | date = May 2007 | pmid = 17456544 | doi = 10.1345/aph.1H621 | s2cid = 22245507 }}</ref> and a different, aggregate study of 2,930 people found 28% were resistant.<ref name="pmid18202034">{{cite journal | vauthors = Krasopoulos G, Brister SJ, Beattie WS, Buchanan MR | title = Aspirin "resistance" and risk of cardiovascular morbidity: systematic review and meta-analysis | journal = BMJ | volume = 336 | issue = 7637 | pages = 195–8 | date = January 2008 | pmid = 18202034 | pmc = 2213873 | doi = 10.1136/bmj.39430.529549.BE }}</ref> |
||
A study in 100 Italian people found, of the apparent 31% aspirin-resistant subjects, only 5% were truly resistant, and the others were [[Compliance (medicine)|noncompliant]].<ref name="pmid18680540">{{cite journal | vauthors = Pignatelli P, Di Santo S, Barillà F, Gaudio C, Violi F | title = Multiple anti-atherosclerotic treatments impair aspirin compliance: effects on aspirin resistance | journal = Journal of Thrombosis and Haemostasis | volume = 6 | issue = 10 | pages = 1832–4 | date = October 2008 | pmid = 18680540 | doi = 10.1111/j.1538-7836.2008.03122.x | s2cid = 1776526 | doi-access = free | title-link = doi }}</ref> |
A study in 100 Italian people found, of the apparent 31% aspirin-resistant subjects, only 5% were truly resistant, and the others were [[Compliance (medicine)|noncompliant]].<ref name="pmid18680540">{{cite journal | vauthors = Pignatelli P, Di Santo S, Barillà F, Gaudio C, Violi F | title = Multiple anti-atherosclerotic treatments impair aspirin compliance: effects on aspirin resistance | journal = Journal of Thrombosis and Haemostasis | volume = 6 | issue = 10 | pages = 1832–4 | date = October 2008 | pmid = 18680540 | doi = 10.1111/j.1538-7836.2008.03122.x | s2cid = 1776526 | doi-access = free | title-link = doi }}</ref> |
||
Another study of 400 healthy volunteers found no subjects who were truly resistant, but some had "pseudoresistance, reflecting delayed and reduced drug absorption". |
Another study of 400 healthy volunteers found no subjects who were truly resistant, but some had "pseudoresistance, reflecting delayed and reduced drug absorption". |
||
| Line 300: | Line 297: | ||
*{{lay source |template = cite news|vauthors = Thomas K|url= https://www.nytimes.com/2012/12/05/business/coating-on-buffered-aspirin-may-hide-its-heart-protective-effects.html|title = Study Raises Questions on Coating of Aspirin|date = 4 December 2012|website = [[The New York Times]] }}</ref> |
*{{lay source |template = cite news|vauthors = Thomas K|url= https://www.nytimes.com/2012/12/05/business/coating-on-buffered-aspirin-may-hide-its-heart-protective-effects.html|title = Study Raises Questions on Coating of Aspirin|date = 4 December 2012|website = [[The New York Times]] }}</ref> |
||
Meta-analysis and systematic reviews have concluded that laboratory confirmed aspirin resistance confers increased rates of poorer outcomes in cardiovascular and neurovascular diseases.<ref>{{cite journal | vauthors = Li J, Song M, Jian Z, Guo W, Chen G, Jiang G, Wang J, Wu X, Huang L |
Meta-analysis and systematic reviews have concluded that laboratory confirmed aspirin resistance confers increased rates of poorer outcomes in cardiovascular and neurovascular diseases.<ref>{{cite journal | vauthors = Li J, Song M, Jian Z, Guo W, Chen G, Jiang G, Wang J, Wu X, Huang L | title = Laboratory aspirin resistance and the risk of major adverse cardiovascular events in patients with coronary heart disease on confirmed aspirin adherence | journal = Journal of Atherosclerosis and Thrombosis | volume = 21 | issue = 3 | pages = 239–47 | date = 2014 | pmid = 24201035 | doi = 10.5551/jat.19521 | doi-access = free | title-link = doi }}</ref><ref name="pmid18202034"/><ref>{{cite journal | vauthors = Sofi F, Marcucci R, Gori AM, Abbate R, Gensini GF | title = Residual platelet reactivity on aspirin therapy and recurrent cardiovascular events--a meta-analysis | journal = International Journal of Cardiology | volume = 128 | issue = 2 | pages = 166–71 | date = August 2008 | pmid = 18242733 | doi = 10.1016/j.ijcard.2007.12.010 | hdl-access = free | hdl = 2158/323452 }}</ref><ref>{{cite journal | vauthors = Shim EJ, Ryu CW, Park S, Lee HN, Shin HS, Kim SB | title = Relationship between adverse events and antiplatelet drug resistance in neurovascular intervention: a meta-analysis | journal = Journal of NeuroInterventional Surgery | volume = 10 | issue = 10 | pages = 942–948 | date = October 2018 | pmid = 29352056 | doi = 10.1136/neurintsurg-2017-013632 | s2cid = 38147668 }}</ref><ref>{{cite journal | vauthors = Fiolaki A, Katsanos AH, Kyritsis AP, Papadaki S, Kosmidou M, Moschonas IC, Tselepis AD, Giannopoulos S | title = High on treatment platelet reactivity to aspirin and clopidogrel in ischemic stroke: A systematic review and meta-analysis | journal = Journal of the Neurological Sciences | volume = 376 | pages = 112–116 | date = May 2017 | pmid = 28431593 | doi = 10.1016/j.jns.2017.03.010 | s2cid = 3485236 }}</ref><ref>{{cite journal | vauthors = Snoep JD, Hovens MM, Eikenboom JC, van der Bom JG, Huisman MV | title = Association of laboratory-defined aspirin resistance with a higher risk of recurrent cardiovascular events: a systematic review and meta-analysis | journal = Archives of Internal Medicine | volume = 167 | issue = 15 | pages = 1593–9 | date = 13 August 2007 | pmid = 17698681 | doi = 10.1001/archinte.167.15.1593 | doi-access = free | title-link = doi }}</ref> Although the majority of research conducted has surrounded cardiovascular and neurovascular, there is emerging research into the risk of aspirin resistance after orthopaedic surgery where aspirin is used for venous thromboembolism prophylaxis.<ref name="A Narrative Review of Aspirin Resis">{{cite journal | vauthors = van Oosterom N, Barras M, Bird R, Nusem I, Cottrell N | title = A Narrative Review of Aspirin Resistance in VTE Prophylaxis for Orthopaedic Surgery | journal = Drugs | volume = 80 | issue = 18 | pages = 1889–1899 | date = December 2020 | pmid = 33037568 | doi = 10.1007/s40265-020-01413-w | s2cid = 222234431 }}</ref> Aspirin resistance in orthopaedic surgery, specifically after total hip and knee arthroplasties, is of interest as risk factors for aspirin resistance are also risk factors for venous thromboembolisms and osteoarthritis; the sequelae of requiring a total hip or knee arthroplasty. Some of these risk factors include obesity, advancing age, diabetes mellitus, dyslipidemia and inflammatory diseases.<ref name="A Narrative Review of Aspirin Resis"/> |
||
== Dosages == |
== Dosages == |
||
Adult aspirin tablets are produced in standardised sizes, which vary slightly from country to country, for example 300{{nbsp}}mg in Britain and 325{{nbsp}}mg in the United States. Smaller doses are based on these standards, ''e.g.'', 75{{nbsp}}mg and 81{{nbsp}}mg tablets. The 81 mg tablets are commonly called "baby aspirin" or "baby-strength", because they were originally{{snd}}[[Reye syndrome|but no longer]]{{snd}}intended to be administered to infants and children.<ref>{{ |
Adult aspirin tablets are produced in standardised sizes, which vary slightly from country to country, for example 300{{nbsp}}mg in Britain and 325{{nbsp}}mg in the United States. Smaller doses are based on these standards, ''e.g.'', 75{{nbsp}}mg and 81{{nbsp}}mg tablets. The 81 mg tablets are commonly called "baby aspirin" or "baby-strength", because they were originally{{snd}}[[Reye syndrome|but no longer]]{{snd}}intended to be administered to infants and children.<ref>{{cite web |title = Invention of the safety cap |url = http://digitaldukemed.mc.duke.edu/pcc/safety_cap.html |website = digitaldukemed.mc.duke.edu |access-date = 4 September 2015 |url-status = live |archive-url = https://web.archive.org/web/20160304071131/http://digitaldukemed.mc.duke.edu/pcc/safety_cap.html |archive-date = 4 March 2016}}</ref> No medical significance occurs due to the slight difference in dosage between the 75{{nbsp}}mg and the 81{{nbsp}}mg tablets. The dose required for benefit appears to depend on a person's weight.<ref name="Lancet2018Dose">{{cite journal | vauthors = Rothwell PM, Cook NR, Gaziano JM, Price JF, Belch JF, Roncaglioni MC, Morimoto T, Mehta Z | title = Effects of aspirin on risks of vascular events and cancer according to bodyweight and dose: analysis of individual patient data from randomised trials | journal = Lancet | volume = 392 | issue = 10145 | pages = 387–399 | date = August 2018 | pmid = 30017552 | pmc = 6083400 | doi = 10.1016/S0140-6736(18)31133-4 }}</ref> For those weighing less than {{convert|70|kg|lb|0}}, low dose is effective for preventing cardiovascular disease; for patients above this weight, higher doses are required.<ref name=Lancet2018Dose/> |
||
In general, for adults, doses are taken four times a day for fever or arthritis,<ref name=BNF>{{ |
In general, for adults, doses are taken four times a day for fever or arthritis,<ref name=BNF>{{cite book|title=British National Formulary|edition=45|year=2003|publisher= [[British Medical Journal]] and [[Royal Pharmaceutical Society of Great Britain]]|title-link=British National Formulary}}</ref> with doses near the maximal daily dose used historically for the treatment of [[rheumatic fever]].<ref>{{cite web |url=http://www.medscape.com/druginfo/monograph?cid=med&drugid=3881&drugname=Aspirin+EC+Oral&monotype=monograph |title=Aspirin monograph: dosages, etc |publisher=Medscape.com |access-date=11 May 2011}}</ref> For the prevention of [[myocardial infarction]] (MI) in someone with documented or suspected [[coronary artery disease]], much lower doses are taken once daily.<ref name=BNF /> |
||
March 2009 recommendations from the USPSTF on the use of aspirin for the primary prevention of coronary heart disease encourage men aged 45–79 and women aged 55–79 to use aspirin when the potential benefit of a reduction in MI for men or stroke for women outweighs the potential harm of an increase in [[Gastrointestinal bleeding|gastrointestinal hemorrhage]].<ref name="USPSTF 2009">{{cite journal | vauthors = ((US Preventive Services Task Force)) | title = Aspirin for the prevention of cardiovascular disease: U.S. Preventive Services Task Force recommendation statement | journal = Annals of Internal Medicine | volume = 150 | issue = 6 | pages = 396–404 | date = March 2009 | pmid = 19293072 | doi = 10.7326/0003-4819-150-6-200903170-00008 | doi-access = free | title-link = doi }}</ref><ref name=medscape>{{cite news|url=http://cme.medscape.com/viewarticle/589895 |title=Aspirin: more evidence that low dose is all that is needed |newspaper=Medscape |publisher=Medscape CME |access-date=11 May 2011}}</ref>{{update inline|date=October 2019}} The WHI study of postmenopausal women found that aspirin resulted in a 25% lower risk of death from cardiovascular disease and a 14% lower risk of death from any cause, though there was no significant difference between 81{{nbsp}}mg and 325{{nbsp}}mg aspirin doses.<ref>{{cite journal | vauthors = Berger JS, Brown DL, Burke GL, Oberman A, Kostis JB, Langer RD, Wong ND, Wassertheil-Smoller S |
March 2009 recommendations from the USPSTF on the use of aspirin for the primary prevention of coronary heart disease encourage men aged 45–79 and women aged 55–79 to use aspirin when the potential benefit of a reduction in MI for men or stroke for women outweighs the potential harm of an increase in [[Gastrointestinal bleeding|gastrointestinal hemorrhage]].<ref name="USPSTF 2009">{{cite journal | vauthors = ((US Preventive Services Task Force)) | title = Aspirin for the prevention of cardiovascular disease: U.S. Preventive Services Task Force recommendation statement | journal = Annals of Internal Medicine | volume = 150 | issue = 6 | pages = 396–404 | date = March 2009 | pmid = 19293072 | doi = 10.7326/0003-4819-150-6-200903170-00008 | doi-access = free | title-link = doi }}</ref><ref name=medscape>{{cite news|url=http://cme.medscape.com/viewarticle/589895 |title=Aspirin: more evidence that low dose is all that is needed |newspaper=Medscape |publisher=Medscape CME |access-date=11 May 2011}}</ref>{{update inline|date=October 2019}} The WHI study of postmenopausal women found that aspirin resulted in a 25% lower risk of death from cardiovascular disease and a 14% lower risk of death from any cause, though there was no significant difference between 81{{nbsp}}mg and 325{{nbsp}}mg aspirin doses.<ref>{{cite journal | vauthors = Berger JS, Brown DL, Burke GL, Oberman A, Kostis JB, Langer RD, Wong ND, Wassertheil-Smoller S |date=March 2009 |title=Aspirin Use, Dose, and Clinical Outcomes in Postmenopausal Women With Stable Cardiovascular Disease |journal=Circulation: Cardiovascular Quality and Outcomes |volume=2 |issue=2 |pages=78–87 |doi=10.1161/circoutcomes.108.791269 |pmid=20031819 |pmc=2801891 |issn=1941-7713 }}</ref> The 2021 ADAPTABLE study also showed no significant difference in cardiovascular events or major bleeding between 81{{nbsp}}mg and 325{{nbsp}}mg doses of aspirin in patients (both men and women) with established cardiovascular disease.<ref>{{cite journal | vauthors = Sacristán JA |date=August 2021 |title=Aspirin Dosing in Cardiovascular Disease |journal=New England Journal of Medicine |volume=385 |issue=8 |pages=764–765 |doi=10.1056/nejmc2110476 |pmid=34407352 |s2cid=237214969 |issn=0028-4793 }}</ref> |
||
Low-dose aspirin use was also associated with a trend toward lower risk of cardiovascular events, and lower aspirin doses (75 or 81{{nbsp}}mg/day) may optimize efficacy and safety for people requiring aspirin for long-term prevention.<ref name="medscape" /> |
Low-dose aspirin use was also associated with a trend toward lower risk of cardiovascular events, and lower aspirin doses (75 or 81{{nbsp}}mg/day) may optimize efficacy and safety for people requiring aspirin for long-term prevention.<ref name="medscape" /> |
||
In children with Kawasaki disease, aspirin is taken at dosages based on body weight, initially four times a day for up to two weeks and then at a lower dose once daily for a further six to eight weeks.<ref>{{ |
In children with Kawasaki disease, aspirin is taken at dosages based on body weight, initially four times a day for up to two weeks and then at a lower dose once daily for a further six to eight weeks.<ref>{{cite book|title=British National Formulary for Children|year=2006|publisher= [[British Medical Journal]] and [[Royal Pharmaceutical Society]]|title-link=British National Formulary for Children}}</ref> |
||
==Adverse effects== |
==Adverse effects== |
||
| Line 320: | Line 317: | ||
<!-- Note that Contraindications is spelled correctly! It does not need to be changed. --> |
<!-- Note that Contraindications is spelled correctly! It does not need to be changed. --> |
||
Aspirin should not be taken by people who are allergic to [[ibuprofen]] or [[naproxen]],<ref name="drugs.com" /><ref name="personalmd">{{cite web |url=http://www.personalmd.com/drgdb/3.htm |archive-url=https://web.archive.org/web/20000918231717/http://personalmd.com/drgdb/3.htm |url-status=dead |archive-date=18 September 2000 |title=Oral Aspirin information |access-date=8 May 2008 |publisher=First DataBank }}</ref> or who have [[salicylate intolerance]]<ref name="pmid16247191">{{cite journal | vauthors = Raithel M, Baenkler HW, Naegel A, Buchwald F, Schultis HW, Backhaus B, Kimpel S, Koch H, Mach K, Hahn EG, Konturek PC |
Aspirin should not be taken by people who are allergic to [[ibuprofen]] or [[naproxen]],<ref name="drugs.com" /><ref name="personalmd">{{cite web |url=http://www.personalmd.com/drgdb/3.htm |archive-url=https://web.archive.org/web/20000918231717/http://personalmd.com/drgdb/3.htm |url-status=dead |archive-date=18 September 2000 |title=Oral Aspirin information |access-date=8 May 2008 |publisher=First DataBank }}</ref> or who have [[salicylate intolerance]]<ref name="pmid16247191">{{cite journal | vauthors = Raithel M, Baenkler HW, Naegel A, Buchwald F, Schultis HW, Backhaus B, Kimpel S, Koch H, Mach K, Hahn EG, Konturek PC | title = Significance of salicylate intolerance in diseases of the lower gastrointestinal tract | journal = Journal of Physiology and Pharmacology | volume = 56 | issue = Suppl 5 | pages = 89–102 | date = September 2005 | pmid = 16247191 | url = http://www.jpp.krakow.pl/journal/archive/09_05_s5/pdf/89_09_05_s5_article.pdf | url-status = live | archive-url = https://web.archive.org/web/20110409093851/http://www.jpp.krakow.pl/journal/archive/09_05_s5/pdf/89_09_05_s5_article.pdf | archive-date = 9 April 2011 }}</ref><ref name="pmid8566739">{{cite journal | vauthors = Senna GE, Andri G, Dama AR, Mezzelani P, Andri L | title = Tolerability of imidazole salycilate in aspirin-sensitive patients | journal = Allergy Proceedings | volume = 16 | issue = 5 | pages = 251–254 | year = 1995 | pmid = 8566739 | doi = 10.2500/108854195778702675 }}</ref> or a more generalized [[drug intolerance]] to NSAIDs, and caution should be exercised in those with [[asthma]] or NSAID-precipitated [[bronchospasm]]. Owing to its effect on the stomach lining, manufacturers recommend people with [[peptic ulcer]]s, mild diabetes, or [[gastritis]] seek medical advice before using aspirin.<ref name="drugs.com" /><ref name="mercksource">{{cite web |title = PDR guide to over the counter (OTC) drugs |url=http://www.mercksource.com/pp/us/cns/cns_hl_pdr.jspzQzpgzEzzSzppdocszSzuszSzcnszSzcontentzSzpdrotczSzotc_fullzSzdrugszSzfgotc036zPzhtm |access-date =28 April 2008 |archive-url= https://web.archive.org/web/20080410223441/http://www.mercksource.com/pp/us/cns/cns_hl_pdr.jspzQzpgzEzzSzppdocszSzuszSzcnszSzcontentzSzpdrotczSzotc_fullzSzdrugszSzfgotc036zPzhtm |archive-date= 10 April 2008 |url-status= live}}</ref> Even if none of these conditions is present, the risk of [[gastrointestinal hemorrhage|stomach bleeding]] is still increased when aspirin is taken with [[alcoholic beverage|alcohol]] or [[warfarin]].<ref name="drugs.com" /><ref name="personalmd" /> People with [[hemophilia]] or other bleeding tendencies should not take aspirin or other salicylates.<ref name="drugs.com" /><ref name="mercksource" /> Aspirin is known to cause [[hemolytic anemia]] in people who have the genetic disease [[glucose-6-phosphate dehydrogenase deficiency]], particularly in large doses and depending on the severity of the disease.<ref>{{cite book |title = Frequencies of hemoglobin variants: thalassemia, the glucose-6-phosphate dehydrogenase deficiency, G6PD variants, and ovalocytosis in human populations |url=https://books.google.com/books?id=OjqNeJERhWwC&q=0195036344|publisher=Oxford University Press |isbn = 978-0-19-503634-3 |vauthors = Livingstone FB |year = 1985}}</ref> Use of aspirin during [[dengue fever]] is not recommended owing to increased bleeding tendency.<ref>{{cite web |title= Dengue and dengue hemorrhagic fever: information for health care practitioners |url = https://www.cdc.gov/NCIDOD/dvbid/dengue/dengue-hcp.htm |access-date =28 April 2008 |archive-url = https://web.archive.org/web/20080317070305/http://www.cdc.gov/Ncidod/dvbid/dengue/dengue-hcp.htm |archive-date = 17 March 2008 }}</ref> Aspirin taken at doses of ≤325 mg and ≤100 mg per day for ≥2 days can increase the odds of suffering a gout attack by 81% and 91% respectively. This effect may potentially be worsened by high purine diets, diuretics, and kidney disease, but is eliminated by the urate lowering drug allopurinol.<ref>{{cite journal | vauthors = Zhang Y, Neogi T, Chen C, Chaisson C, Hunter DJ, Choi H | title = Low-dose aspirin use and recurrent gout attacks | journal = Annals of the Rheumatic Diseases | volume = 73 | issue = 2 | pages = 385–390 | date = February 2014 | pmid = 23345599 | pmc = 3902644 | doi = 10.1136/annrheumdis-2012-202589 }}</ref> Daily low dose aspirin does not appear to worsen kidney function.<ref>{{cite journal | vauthors = Polkinghorne KR, Wetmore JB, Thao LT, Wolfe R, Woods RL, Ernst ME, Nelson MR, Reid CM, Shah RC, McNeil JJ, Murray AM | title = Effect of Aspirin on CKD Progression in Older Adults: Secondary Analysis From the ASPREE Randomized Clinical Trial | journal = American Journal of Kidney Diseases | volume = 80 | issue = 6 | pages = 810–813 | date = December 2022 | pmid = 35430328 | pmc = 9562592 | doi = 10.1053/j.ajkd.2022.02.019 }}</ref> Aspirin may reduce cardiovascular risk in those without established cardiovascular disease in people with moderate CKD, without significantly increasing the risk of bleeding.<ref>{{cite journal | vauthors = Mann JF, Joseph P, Gao P, Pais P, Tyrwhitt J, Xavier D, Dans T, Jaramillo PL, Gamra H, Yusuf S | title = Effects of aspirin on cardiovascular outcomes in patients with chronic kidney disease | journal = Kidney International | volume = 103 | issue = 2 | pages = 403–410 | date = February 2023 | pmid = 36341885 | doi = 10.1016/j.kint.2022.09.023 | s2cid = 253194139 | doi-access = free }}</ref> Aspirin should not be given to children or adolescents under the age of 16 to control cold or influenza symptoms, as this has been linked with [[Reye syndrome|Reye's syndrome]].<ref name="BMJ2002-Macdonald">{{cite journal | vauthors = Macdonald S | title = Aspirin use to be banned in under 16 year olds | journal = BMJ | volume = 325 | issue = 7371 | pages = 988c–988 | date = November 2002 | pmid = 12411346 | pmc = 1169585 | doi = 10.1136/bmj.325.7371.988/c }}</ref> |
||
===Gastrointestinal=== |
===Gastrointestinal=== |
||
Aspirin |
Aspirin increases the risk of [[upper gastrointestinal bleeding]].<ref name="Sorensen 2000">{{cite journal | vauthors = Sørensen HT, Mellemkjaer L, Blot WJ, Nielsen GL, Steffensen FH, McLaughlin JK, Olsen JH | title = Risk of upper gastrointestinal bleeding associated with use of low-dose aspirin | journal = The American Journal of Gastroenterology | volume = 95 | issue = 9 | pages = 2218–2224 | date = September 2000 | pmid = 11007221 | doi = 10.1016/s0002-9270(00)01040-6 }}</ref> Enteric coating on aspirin may be used in manufacturingto prevent release of aspirin into the stomach to reduce gastric harm, but enteric coating does not reduce gastrointestinal bleeding risk.<ref name="Sorensen 2000" /><ref name="Kedir 2021">{{cite journal | vauthors = Kedir HM, Sisay EA, Abiye AA | title = Enteric-Coated Aspirin and the Risk of Gastrointestinal Side Effects: A Systematic Review | journal = International Journal of General Medicine | volume = 14 | pages = 4757–4763 | year = 2021 | pmid = 34466020 | doi = 10.2147/ijgm.s326929 | pmc = 8403009 | doi-access = free }}</ref> Enteric-coated aspirin may not be as effective at reducing blood clot risk.<ref>{{cite web | vauthors = Torborg L | title=Mayo Clinic Q and A: Coated aspirin may not be as effective at reducing blood clot risk | website=Mayo Clinic News Network | date=4 December 2018 | url=https://newsnetwork.mayoclinic.org/discussion/mayo-clinic-q-and-a-coated-aspirin-may-not-be-as-effective-at-reducing-blood-clot-risk/}}</ref><ref>{{cite journal | vauthors = Cox D, Maree AO, Dooley M, Conroy R, Byrne MF, Fitzgerald DJ | title = Effect of enteric coating on antiplatelet activity of low-dose aspirin in healthy volunteers | journal = Stroke | volume = 37 | issue = 8 | pages = 2153–2158 | date = August 2006 | pmid = 16794200 | doi = 10.1161/01.STR.0000231683.43347.ec | s2cid = 8034371 | doi-access = free }}</ref> Combining aspirin with other [[Nonsteroidal anti-inflammatory drug|NSAIDs]] has been shown to further increase the riskofgastrointestinal bleeding.<ref name="Sorensen 2000" /> Using aspirin in combination with clopidogrel or warfarin also increases the risk of upper gastrointestinal bleeding.<ref>{{cite journal | vauthors = Delaney JA, Opatrny L, Brophy JM, Suissa S | title = Drug drug interactions between antithrombotic medications and the risk of gastrointestinal bleeding | journal = CMAJ | volume = 177 | issue = 4 | pages = 347–351 | date = August 2007 | pmid = 17698822 | pmc = 1942107 | doi = 10.1503/cmaj.070186 }}</ref> |
||
|
Blockade of COX-1 by aspirin apparently results in the upregulation of COX-2aspart of a gastric defense.<ref>{{cite journal |vauthors = Wallace JL |title = Prostaglandins, NSAIDs, and gastric mucosal protection: why doesn't the stomach digest itself? |journal = Physiological Reviews |volume = 88 |issue = 4 |pages = 1547–65 |date = October 2008 |pmid = 18923189 |doi = 10.1152/physrev.00004.2008 |s2cid = 448875 }}</ref> There is no clear evidence that simultaneous use of a COX-2 inhibitor with aspirin may increase the risk of gastrointestinal injury.<ref name="Rostom-2007">{{cite journal |vauthors = Rostom A, Muir K, Dubé C, Jolicoeur E, Boucher M, Joyce J, Tugwell P, Wells GW |title = Gastrointestinal safetyofcyclooxygenase-2 inhibitors: a Cochrane Collaboration systematic review |journal = Clinical Gastroenterology and Hepatology |volume = 5 |issue = 7 |pages = 818–28, 828.e1-5; quiz 768 |date = July 2007 |pmid = 17556027 |doi = 10.1016/j.cgh.2007.03.011 |doi-access = free }}</ref> |
||
| ⚫ | "[[Buffer solution|Buffering]]" is an additional method used with the intent to mitigate gastrointestinal bleeding, such as by preventing aspirin from concentrating in the walls of the stomach, although the benefits of buffered aspirin are disputed.<ref name="Clerici_2023">{{cite journal | vauthors = Clerici B, Cattaneo M | title = Pharmacological Efficacy and Gastrointestinal Safety of Different Aspirin Formulations for Cardiovascular Prevention: A Narrative Review | journal = Journal of Cardiovascular Development and Disease | volume = 10 | issue = 4 | date = March 2023 | page = 137 | pmid = 37103016 | pmc = 10145431 | doi = 10.3390/jcdd10040137 | doi-access = free }}</ref> Almost any buffering agent used in antacids can be used; Bufferin, for example, uses [[magnesium oxide]]. Other preparations use [[calcium carbonate]].<ref>{{cite web |url=http://antoine.frostburg.edu/chem/senese/101/acidbase/faq/buffered-aspirin.shtml |title=General chemistry online: FAQ: Acids and bases: What is the buffer system in buffered aspirin? |publisher=Antoine.frostburg.edu |access-date=11 May 2011 |url-status=live |archive-url=https://web.archive.org/web/20110414145143/http://antoine.frostburg.edu/chem/senese/101/acidbase/faq/buffered-aspirin.shtml |archive-date=14 April 2011}}</ref> Gas-forming agents in [[effervescent tablet|effervescent tablet and powder]] formulations can also double as a buffering agent, one example being [[sodium bicarbonate]], used in [[Alka-Seltzer]].<ref>{{cite journal | vauthors = Davison C, Smith BW, Smith PK | title = Effects of buffered and unbuffered acetylsalicylic acid upon the gastric acidity of normal human subjects | journal = Journal of Pharmaceutical Sciences | volume = 51 | issue = 8 | pages = 759–763 | date = August 1962 | pmid = 13883982 | doi = 10.1002/jps.2600510813 }}</ref> |
||
Combining aspirin with other [[Nonsteroidal anti-inflammatory drug|NSAIDs]] has been shown to further increase the risk of gastrointestinal bleeding.<ref name="H Toft" /> Using aspirin in combination with clopidogrel or warfarin also increases the risk of upper gastrointestinal bleeding.<ref>{{cite journal |vauthors = Delaney JA, Opatrny L, Brophy JM, Suissa S |title = Drug drug interactions between antithrombotic medications and the risk of gastrointestinal bleeding |journal = CMAJ | volume = 177 |issue = 4 |pages = 347–51 |date = August 2007 |pmid = 17698822 |pmc = 1942107 |doi = 10.1503/cmaj.070186 }}</ref> |
|||
| ⚫ | Taking vitamin C with aspirin has been investigated as a method of protecting the stomach lining. In trials vitamin C-releasing aspirin (ASA-VitC) or a buffered aspirin formulation containing vitamin C was found to cause less stomach damage than aspirin alone.<ref name="Dammann">{{cite journal |vauthors = Dammann HG, Saleki M, Torz M, Schulz HU, Krupp S, Schürer M, Timm J, Gessner U |title = Effects of buffered and plain acetylsalicylic acid formulations with and without ascorbic acid on gastric mucosa in healthy subjects |journal = Alimentary Pharmacology & Therapeutics |volume = 19 |issue = 3 |pages = 367–74 |date = February 2004 |pmid = 14984384 |doi = 10.1111/j.1365-2036.2004.01742.x |s2cid = 22688422 |doi-access = free | title-link = doi }}</ref><ref name="Konturek">{{cite journal |vauthors = Konturek PC, Kania J, Hahn EG, Konturek JW |title = Ascorbic acid attenuates aspirin-induced gastric damage: role of inducible nitric oxide synthase |journal = Journal of Physiology and Pharmacology |volume = 57 |issue = Suppl 5 |pages = 125–36 |date = November 2006 |pmid = 17218764 }}</ref> |
||
Blockade of COX-1 by aspirin apparently results in the upregulation of COX-2 as part of a gastric defense.<ref>{{cite journal |vauthors = Wallace JL |title = Prostaglandins, NSAIDs, and gastric mucosal protection: why doesn't the stomach digest itself? |journal = Physiological Reviews |volume = 88 |issue = 4 |pages = 1547–65 |date = October 2008 |pmid = 18923189 |doi = 10.1152/physrev.00004.2008 |s2cid = 448875 }}</ref> Several trials suggest that the simultaneous use of a COX-2 inhibitor with aspirin may increase the risk of gastrointestinal injury.<ref>{{cite journal |vauthors = Laine L, Maller ES, Yu C, Quan H, Simon T |title = Ulcer formation with low-dose enteric-coated aspirin and the effect of COX-2 selective inhibition: a double-blind trial |journal = Gastroenterology |volume = 127 |issue = 2 |pages = 395–402 |date = August 2004 |pmid = 15300570 |doi = 10.1053/j.gastro.2004.05.001 |doi-access = free }}</ref><ref>{{cite journal |vauthors = Fiorucci S, Santucci L, Wallace JL, Sardina M, Romano M, del Soldato P, Morelli A | display-authors = 6 |title = Interaction of a selective cyclooxygenase-2 inhibitor with aspirin and NO-releasing aspirin in the human gastric mucosa |journal = Proceedings of the National Academy of Sciences of the United States of America |volume = 100 |issue = 19 |pages = 10937–41 |date = September 2003 |pmid = 12960371 |pmc = 196906 |doi = 10.1073/pnas.1933204100 |bibcode = 2003PNAS..10010937F |doi-access = free | title-link = doi }}</ref> However, currently available evidence has been unable to prove that this effect is consistently repeatable in everyday clinical practice.<ref name="Rostom-2007">{{cite journal |vauthors = Rostom A, Muir K, Dubé C, Jolicoeur E, Boucher M, Joyce J, Tugwell P, Wells GW |display-authors = 6 |title = Gastrointestinal safety of cyclooxygenase-2 inhibitors: a Cochrane Collaboration systematic review |journal = Clinical Gastroenterology and Hepatology |volume = 5 |issue = 7 |pages = 818–28, 828.e1-5; quiz 768 |date = July 2007 |pmid = 17556027 |doi = 10.1016/j.cgh.2007.03.011 |doi-access = free }}</ref> More dedicated research is required to provide greater clarity on the subject.<ref name="Rostom-2007" /> Therefore, caution should be exercised if combining aspirin with any "natural" supplements with COX-2-inhibiting properties, such as garlic extracts, curcumin, bilberry, pine bark, ginkgo, fish oil, resveratrol, genistein, quercetin, resorcinol, and others.{{Citation needed |date=July 2019}} |
|||
| ⚫ |
"[[Buffer solution|Buffering]]" is an additional method |
||
| ⚫ |
Taking |
||
===Retinal vein occlusion=== |
===Retinal vein occlusion=== |
||
| Line 346: | Line 339: | ||
===Reye's syndrome=== |
===Reye's syndrome=== |
||
{{Main|Reye's syndrome}} |
{{Main|Reye's syndrome}} |
||
Reye's syndrome, a rare but severe illness characterized by acute [[encephalopathy]] and [[fatty liver]], can occur when children or adolescents are given aspirin for a fever or other illness or infection. From 1981 to 1997, 1207 cases of Reye's syndrome in people younger than 18 were reported to the US [[Centers for Disease Control and Prevention]] (CDC). Of these, 93% reported being ill in the three weeks preceding the onset of Reye's syndrome, most commonly with a [[Respiratory tract infection|respiratory infection]], [[chickenpox]], or [[diarrhea]]. Salicylates were detectable in 81.9% of children for whom test results were reported.<ref name=Belay>{{cite journal |vauthors = Belay ED, Bresee JS, Holman RC, Khan AS, Shahriari A, Schonberger LB |title = Reye's syndrome in the United States from 1981 through 1997 |journal = The New England Journal of Medicine |volume = 340 |issue = 18 |pages = 1377–82 |date = May 1999 |pmid = 10228187 |doi = 10.1056/NEJM199905063401801 }}</ref> After the association between Reye's syndrome and aspirin was reported, and safety measures to prevent it (including a [[Surgeon General of the United States|Surgeon General]]'s warning, and changes to the labeling of aspirin-containing drugs) were implemented, aspirin taken by children declined considerably in the United States, as did the number of reported cases of Reye's syndrome; a similar decline was found in the United Kingdom after warnings against pediatric aspirin use were issued.<ref name=Belay/> The US [[Food and Drug Administration]] recommends aspirin (or aspirin-containing products) should not be given to anyone under the age of 12 who has a fever,<ref name="BMJ2002-Macdonald"/> and the UK [[National Health Service]] recommends children who are under 16 years of age should not take aspirin, unless it is on the advice of a doctor.<ref>{{cite web |url=http://www.nhs.uk/conditions/Reyes-syndrome/Pages/Introduction.aspx |title= Reye's syndrome |publisher=National Health Service |work=NHS Choices |date= 12 January 2016}}</ref> |
Reye's syndrome, a rare but severe illness characterized by acute [[encephalopathy]] and [[fatty liver]], can occur when children or adolescents are given aspirin for a fever or other illness or infection. From 1981 to 1997, 1207 cases of Reye's syndrome in people younger than 18 were reported to the US [[Centers for Disease Control and Prevention]] (CDC). Of these, 93% reported being ill in the three weeks preceding the onset of Reye's syndrome, most commonly with a [[Respiratory tract infection|respiratory infection]], [[chickenpox]], or [[diarrhea]]. Salicylates were detectable in 81.9% of children for whom test results were reported.<ref name=Belay>{{cite journal |vauthors = Belay ED, Bresee JS, Holman RC, Khan AS, Shahriari A, Schonberger LB |title = Reye's syndrome in the United States from 1981 through 1997 |journal = The New England Journal of Medicine |volume = 340 |issue = 18 |pages = 1377–82 |date = May 1999 |pmid = 10228187 |doi = 10.1056/NEJM199905063401801 |doi-access = free }}</ref> After the association between Reye's syndrome and aspirin was reported, and safety measures to prevent it (including a [[Surgeon General of the United States|Surgeon General]]'s warning, and changes to the labeling of aspirin-containing drugs) were implemented, aspirin taken by children declined considerably in the United States, as did the number of reported cases of Reye's syndrome; a similar decline was found in the United Kingdom after warnings against pediatric aspirin use were issued.<ref name=Belay/> The US [[Food and Drug Administration]] recommends aspirin (or aspirin-containing products) should not be given to anyone under the age of 12 who has a fever,<ref name="BMJ2002-Macdonald"/> and the UK [[National Health Service]] recommends children who are under 16 years of age should not take aspirin, unless it is on the advice of a doctor.<ref>{{cite web |url=http://www.nhs.uk/conditions/Reyes-syndrome/Pages/Introduction.aspx |title= Reye's syndrome |publisher=National Health Service |work=NHS Choices |date= 12 January 2016}}</ref> |
||
===Skin=== |
===Skin=== |
||
For a small number of people, taking aspirin can result in symptoms including [[hives]], swelling, and headache.<ref>{{ |
For a small number of people, taking aspirin can result in symptoms including [[hives]], swelling, and headache.<ref>{{cite web |url=https://health.clevelandclinic.org/are-you-sensitive-to-aspirin-here-are-some-reasons-why/ |title=Are You Sensitive to Aspirin? Here are Some Reasons Why |date=5 February 2015 |website=Health Essentials from Cleveland Clinic |access-date=5 March 2020 |archive-date=25 October 2020 |archive-url=https://web.archive.org/web/20201025171549/https://health.clevelandclinic.org/are-you-sensitive-to-aspirin-here-are-some-reasons-why/ |url-status=dead }}</ref> Aspirin can exacerbate symptoms among those with chronic hives, or create acute symptoms of hives.<ref name="Doña-2018">{{cite journal |vauthors = Doña I, Barrionuevo E, Salas M, Laguna JJ, Agúndez J, García-Martín E, Bogas G, Perkins JR, Cornejo-García JA, Torres MJ |title = NSAIDs-hypersensitivity often induces a blended reaction pattern involving multiple organs |journal = Scientific Reports |volume = 8 |issue = 1 |pages = 16710 |date = November 2018 |pmid = 30420763 |pmc = 6232098 |doi = 10.1038/s41598-018-34668-1 |bibcode = 2018NatSR...816710D }}</ref> These responses can be due to allergic reactions to aspirin, or more often due to its effect of inhibiting the COX-1 enzyme.<ref name="Doña-2018" /><ref name="Kowalski-2019">{{cite journal |vauthors = Kowalski ML, Agache I, Bavbek S, Bakirtas A, Blanca M, Bochenek G, Bonini M, Heffler E, Klimek L, Laidlaw TM, Mullol J, Niżankowska-Mogilnicka E, Park HS, Sanak M, Sanchez-Borges M, Sanchez-Garcia S, Scadding G, Taniguchi M, Torres MJ, White AA, Wardzyńska A |title = Diagnosis and management of NSAID-Exacerbated Respiratory Disease (N-ERD)-a EAACI position paper |journal = Allergy |volume = 74 |issue = 1 |pages = 28–39 |date = January 2019 |pmid = 30216468 |doi = 10.1111/all.13599 |s2cid = 52276808 |doi-access = free | title-link = doi }}</ref> Skin reactions may also tie to systemic contraindications, seen with NSAID-precipitated [[bronchospasm]],<ref name="Doña-2018" /><ref name="Kowalski-2019" /> or those with [[atopy]].<ref>{{cite journal |vauthors = Sánchez-Borges M, Capriles-Hulett A |title = Atopy is a risk factor for non-steroidal anti-inflammatory drug sensitivity |journal = Annals of Allergy, Asthma & Immunology |volume = 84 |issue = 1 |pages = 101–6 |date = January 2000 |pmid = 10674573 |doi = 10.1016/S1081-1206(10)62748-2 }}</ref> |
||
Aspirin and other NSAIDs, such as ibuprofen, may delay the healing of skin wounds.<ref>{{cite journal |vauthors=Stadelmann WK, Digenis AG, Tobin GR |title=Impediments to wound healing |journal=American Journal of Surgery |volume=176 |issue=2A Suppl |pages=39S–47S |date=August 1998 |pmid=9777971 |doi=10.1016/S0002-9610(98)00184-6}}</ref> Earlier findings from two small, low-quality trials suggested a benefit with aspirin (alongside compression therapy) on venous leg ulcer healing time and leg ulcer size,<ref>{{cite journal |vauthors=Layton AM, Ibbotson SH, Davies JA, Goodfield MJ |title=Randomised trial of oral aspirin for chronic venous leg ulcers |journal=Lancet |volume=344 |issue=8916 |pages=164–5 |date=July 1994 |pmid=7912767 |doi=10.1016/s0140-6736(94)92759-6 |s2cid=912169}}</ref><ref>{{cite journal |vauthors=del Río Solá ML, Antonio J, Fajardo G, Vaquero Puerta C |title=Influence of aspirin therapy in the ulcer associated with chronic venous insufficiency |journal=Annals of Vascular Surgery |volume=26 |issue=5 |pages=620–9 |date=July 2012 |pmid=22437068 |doi=10.1016/j.avsg.2011.02.051 | hdl=10324/2904 |hdl-access=free }}</ref><ref>{{cite journal |vauthors=de Oliveira Carvalho PE, Magolbo NG, De Aquino RF, Weller CD |title=Oral aspirin for treating venous leg ulcers |journal=The Cochrane Database of Systematic Reviews |volume=2016 |pages=CD009432 |date=February 2016 |issue=2 |pmid=26889740 |doi=10.1002/14651858.CD009432.pub2 |pmc=8627253 |collaboration=Cochrane Wounds Group}}</ref> however larger, more recent studies of higher quality have been unable to corroborate these outcomes.<ref>{{cite journal |vauthors=Jull A, Wadham A, Bullen C, Parag V, Kerse N, Waters J |title=Low dose aspirin as adjuvant treatment for venous leg ulceration: pragmatic, randomised, double blind, placebo controlled trial (Aspirin4VLU) |journal=BMJ |volume=359 |pages=j5157 |date=November 2017 |pmid=29175902 |pmc=5701114 |doi=10.1136/bmj.j5157}}</ref><ref>{{cite journal |
Aspirin and other NSAIDs, such as ibuprofen, may delay the healing of skin wounds.<ref>{{cite journal |vauthors=Stadelmann WK, Digenis AG, Tobin GR |title=Impediments to wound healing |journal=American Journal of Surgery |volume=176 |issue=2A Suppl |pages=39S–47S |date=August 1998 |pmid=9777971 |doi=10.1016/S0002-9610(98)00184-6}}</ref> Earlier findings from two small, low-quality trials suggested a benefit with aspirin (alongside compression therapy) on venous leg ulcer healing time and leg ulcer size,<ref>{{cite journal |vauthors=Layton AM, Ibbotson SH, Davies JA, Goodfield MJ |title=Randomised trial of oral aspirin for chronic venous leg ulcers |journal=Lancet |volume=344 |issue=8916 |pages=164–5 |date=July 1994 |pmid=7912767 |doi=10.1016/s0140-6736(94)92759-6 |s2cid=912169}}</ref><ref>{{cite journal |vauthors=del Río Solá ML, Antonio J, Fajardo G, Vaquero Puerta C |title=Influence of aspirin therapy in the ulcer associated with chronic venous insufficiency |journal=Annals of Vascular Surgery |volume=26 |issue=5 |pages=620–9 |date=July 2012 |pmid=22437068 |doi=10.1016/j.avsg.2011.02.051 | hdl=10324/2904 |hdl-access=free }}</ref><ref>{{cite journal |vauthors=de Oliveira Carvalho PE, Magolbo NG, De Aquino RF, Weller CD |title=Oral aspirin for treating venous leg ulcers |journal=The Cochrane Database of Systematic Reviews |volume=2016 |pages=CD009432 |date=February 2016 |issue=2 |pmid=26889740 |doi=10.1002/14651858.CD009432.pub2 |pmc=8627253 |collaboration=Cochrane Wounds Group}}</ref> however larger, more recent studies of higher quality have been unable to corroborate these outcomes.<ref>{{cite journal |vauthors=Jull A, Wadham A, Bullen C, Parag V, Kerse N, Waters J |title=Low dose aspirin as adjuvant treatment for venous leg ulceration: pragmatic, randomised, double blind, placebo controlled trial (Aspirin4VLU) |journal=BMJ |volume=359 |pages=j5157 |date=November 2017 |pmid=29175902 |pmc=5701114 |doi=10.1136/bmj.j5157}}</ref><ref>{{cite journal|vauthors=Tilbrook H, Clark L, Cook L, Bland M, Buckley H, Chetter I, Dumville J, Fenner C, Forsythe R, Gabe R, Harding K, Layton A, Lindsay E, McDaid C, Moffatt C, Rolfe D, Sbizzera I, Stansby G, Torgerson D, Vowden P, Williams L, Hinchliffe R|date=October 2018|title=AVURT: aspirin versus placebo for the treatment of venous leg ulcers - a Phase II pilot randomised controlled trial|journal=Health Technology Assessment|volume=22|issue=55|pages=1–138|doi=10.3310/hta22550|pmc=6204573|pmid=30325305}}</ref> As such, further research is required to clarify the role of aspirin in this context. |
||
===Other adverse effects=== |
===Other adverse effects=== |
||
Aspirin can induce [[angioedema|swelling of skin tissues]] in some people. In one study, [[angioedema]] appeared one to six hours after ingesting aspirin in some of the people. However, when the aspirin was taken alone, it did not cause angioedema in these people; the aspirin had been taken in combination with another NSAID-induced drug when angioedema appeared.<ref>{{cite journal |vauthors = Berges-Gimeno MP, Stevenson DD |title = Nonsteroidal anti-inflammatory drug-induced reactions and desensitization |journal = The Journal of Asthma |volume = 41 |issue = 4 |pages = 375–84 |date = June 2004 |pmid = 15281324 |doi = 10.1081/JAS-120037650 |s2cid = 29909460 }}</ref> |
Aspirin can induce [[angioedema|swelling of skin tissues]] in some people. In one study, [[angioedema]] appeared one to six hours after ingesting aspirin in some of the people. However, when the aspirin was taken alone, it did not cause angioedema in these people; the aspirin had been taken in combination with another NSAID-induced drug when angioedema appeared.<ref>{{cite journal |vauthors = Berges-Gimeno MP, Stevenson DD |title = Nonsteroidal anti-inflammatory drug-induced reactions and desensitization |journal = The Journal of Asthma |volume = 41 |issue = 4 |pages = 375–84 |date = June 2004 |pmid = 15281324 |doi = 10.1081/JAS-120037650 |s2cid = 29909460 }}</ref> |
||
Aspirin causes an increased risk of cerebral microbleeds having the appearance on [[MRI]] scans of 5 to 10{{nbsp}}mm or smaller, hypointense (dark holes) patches.<ref>{{cite journal |vauthors = Vernooij MW, Haag MD, van der Lugt A, Hofman A, Krestin GP, Stricker BH, Breteler MM |
Aspirin causes an increased risk of cerebral microbleeds, having the appearance on [[MRI]] scans of 5 to 10{{nbsp}}mm or smaller, hypointense (dark holes) patches.<ref>{{cite journal |vauthors = Vernooij MW, Haag MD, van der Lugt A, Hofman A, Krestin GP, Stricker BH, Breteler MM |title = Use of antithrombotic drugs and the presence of cerebral microbleeds: the Rotterdam Scan Study |journal = Archives of Neurology |volume = 66 |issue = 6 |pages = 714–20 | date = June 2009 |pmid = 19364926 |doi = 10.1001/archneurol.2009.42 |doi-access = free | title-link = doi }}</ref><ref>{{cite journal |vauthors = Gorelick PB |title = Cerebral microbleeds: evidence of heightened risk associated with aspirin use |journal = Archives of Neurology |volume = 66 |issue = 6 |pages = 691–3 |date = June 2009 |pmid = 19506128 |doi = 10.1001/archneurol.2009.85 }}</ref> |
||
A study of a group with a mean dosage of aspirin of 270{{nbsp}}mg per day estimated an average absolute risk increase in [[intracerebral hemorrhage]] (ICH) of 12 events per 10,000 persons.<ref name=He1998/> In comparison, the estimated absolute risk reduction in myocardial infarction was 137 events per 10,000 persons, and a reduction of 39 events per 10,000 persons in ischemic stroke.<ref name=He1998>{{cite journal |vauthors = He J, Whelton PK, Vu B, Klag MJ |title = Aspirin and risk of hemorrhagic stroke: a meta-analysis of randomized controlled trials |journal = JAMA |volume = 280 |issue = 22 |pages = 1930–5 |date = December 1998 |pmid = 9851479 |doi = 10.1001/jama.280.22.1930 |s2cid = 22997730 }}</ref> In cases where ICH already has occurred, aspirin use results in higher mortality, with a dose of about 250{{nbsp}}mg per day resulting in a [[relative risk]] of death within three months after the ICH around 2.5 (95% [[confidence interval]] 1.3 to 4.6).<ref name=Saloheimo2006>{{cite journal |vauthors = Saloheimo P, Ahonen M, Juvela S, Pyhtinen J, Savolainen ER, Hillbom M |title = Regular aspirin-use preceding the onset of primary intracerebral hemorrhage is an independent predictor for death |journal = Stroke |volume = 37 |issue = 1 |pages = 129–33 |date = January 2006 |pmid = 16322483 |doi = 10.1161/01.STR.0000196991.03618.31 |doi-access = free | title-link = doi }}</ref> |
A study of a group with a mean dosage of aspirin of 270{{nbsp}}mg per day estimated an average absolute risk increase in [[intracerebral hemorrhage]] (ICH) of 12 events per 10,000 persons.<ref name=He1998/> In comparison, the estimated absolute risk reduction in myocardial infarction was 137 events per 10,000 persons, and a reduction of 39 events per 10,000 persons in ischemic stroke.<ref name=He1998>{{cite journal |vauthors = He J, Whelton PK, Vu B, Klag MJ |title = Aspirin and risk of hemorrhagic stroke: a meta-analysis of randomized controlled trials |journal = JAMA |volume = 280 |issue = 22 |pages = 1930–5 |date = December 1998 |pmid = 9851479 |doi = 10.1001/jama.280.22.1930 |s2cid = 22997730 }}</ref> In cases where ICH already has occurred, aspirin use results in higher mortality, with a dose of about 250{{nbsp}}mg per day resulting in a [[relative risk]] of death within three months after the ICH around 2.5 (95% [[confidence interval]] 1.3 to 4.6).<ref name=Saloheimo2006>{{cite journal |vauthors = Saloheimo P, Ahonen M, Juvela S, Pyhtinen J, Savolainen ER, Hillbom M |title = Regular aspirin-use preceding the onset of primary intracerebral hemorrhage is an independent predictor for death |journal = Stroke |volume = 37 |issue = 1 |pages = 129–33 |date = January 2006 |pmid = 16322483 |doi = 10.1161/01.STR.0000196991.03618.31 |doi-access = free | title-link = doi }}</ref> |
||
Aspirin and other NSAIDs can cause [[hyperkalemia|abnormally high blood levels of potassium]] by inducing a [[hyporeninemic hypoaldosteronism|hyporeninemic |
Aspirin and other NSAIDs can cause [[hyperkalemia|abnormally high blood levels of potassium]] by inducing a [[hyporeninemic hypoaldosteronism|hyporeninemic hypoaldosteronism state]] via inhibition of prostaglandin synthesis; however, these agents do not typically cause hyperkalemia by themselves in the setting of normal renal function and euvolemic state.<ref>Medical knowledge self-assessment program for students 4, By American College of Physicians, Clerkship Directors in Internal Medicine, Nephrology 227, Item 29</ref> |
||
Use of low-dose aspirin before a surgical procedure has been associated with an increased risk of bleeding events in some patients, however, ceasing aspirin prior to surgery has also been associated with an increase in major adverse cardiac events. An analysis of multiple studies found a three-fold increase in adverse events such as [[myocardial infarction]] in patients who ceased aspirin prior to surgery. The analysis found that the risk is dependent on the type of surgery being performed and the patient indication for aspirin use.<ref>{{cite journal | vauthors = Biondi-Zoccai GG, Lotrionte M, Agostoni P, Abbate A, Fusaro M, Burzotta F, Testa L, Sheiban I, Sangiorgi G |
Use of low-dose aspirin before a surgical procedure has been associated with an increased risk of bleeding events in some patients, however, ceasing aspirin prior to surgery has also been associated with an increase in major adverse cardiac events. An analysis of multiple studies found a three-fold increase in adverse events such as [[myocardial infarction]] in patients who ceased aspirin prior to surgery. The analysis found that the risk is dependent on the type of surgery being performed and the patient indication for aspirin use.<ref>{{cite journal | vauthors = Biondi-Zoccai GG, Lotrionte M, Agostoni P, Abbate A, Fusaro M, Burzotta F, Testa L, Sheiban I, Sangiorgi G | title = A systematic review and meta-analysis on the hazards of discontinuing or not adhering to aspirin among 50,279 patients at risk for coronary artery disease | journal = European Heart Journal | volume = 27 | issue = 22 | pages = 2667–2674 | date = November 2006 | pmid = 17053008 | doi = 10.1093/eurheartj/ehl334 }}</ref> |
||
On 9 July 2015, the US [[Food and Drug Administration]] (FDA) toughened warnings of increased [[heart attack]] and [[stroke]] risk associated with [[nonsteroidal anti-inflammatory drug]]s (NSAID).<ref name="FDA-20150709" /> Aspirin is an NSAID but is not affected by the new warnings.<ref name="FDA-20150709">{{cite web |title=FDA strengthens warning of heart attack and stroke risk for non-steroidal anti-inflammatory drugs |url=https://www.fda.gov/consumers/consumer-updates/fda-strengthens-warning-heart-attack-and-stroke-risk-non-steroidal-anti-inflammatory-drugs |date=9 July 2015 |work=U.S. [[Food and Drug Administration]] (FDA) |access-date=9 July 2015 |url-status=live |archive-url=https://web.archive.org/web/20150711004922/https://www.fda.gov/ForConsumers/ConsumerUpdates/ucm453610.htm |archive-date=11 July 2015}}</ref> |
On 9 July 2015, the US [[Food and Drug Administration]] (FDA) toughened warnings of increased [[heart attack]] and [[stroke]] risk associated with [[nonsteroidal anti-inflammatory drug]]s (NSAID).<ref name="FDA-20150709" /> Aspirin is an NSAID but is not affected by the new warnings.<ref name="FDA-20150709">{{cite web |title=FDA strengthens warning of heart attack and stroke risk for non-steroidal anti-inflammatory drugs |url=https://www.fda.gov/consumers/consumer-updates/fda-strengthens-warning-heart-attack-and-stroke-risk-non-steroidal-anti-inflammatory-drugs |date=9 July 2015 |work=U.S. [[Food and Drug Administration]] (FDA) |access-date=9 July 2015 |url-status=live |archive-url=https://web.archive.org/web/20150711004922/https://www.fda.gov/ForConsumers/ConsumerUpdates/ucm453610.htm |archive-date=11 July 2015}}</ref> |
||
| Line 368: | Line 361: | ||
===Overdose=== |
===Overdose=== |
||
{{Main|Aspirin poisoning}} |
{{Main|Aspirin poisoning}} |
||
Aspirin overdose can be acute or chronic. In acute poisoning, a single large dose is taken; in chronic poisoning, higher than normal doses are taken over a period of time. Acute overdose has a [[mortality rate]] of 2%. Chronic overdose is more commonly lethal, with a mortality rate of 25%;<ref>{{cite web |vauthors = Kreplick LW |year=2001 |title=Salicylate toxicity in emergency medicine |publisher=[[Medscape]] |url=http://misc.medscape.com/pi/android/medscapeapp/html/A818242-business.html |url-status=live |archive-url=https://web.archive.org/web/20120831184805/http://misc.medscape.com/pi/android/medscapeapp/html/A818242-business.html |archive-date=31 August 2012}}</ref> chronic overdose may be especially severe in children.<ref name="Pediatrics1982-gaudreault">{{cite journal |vauthors = Gaudreault P, Temple AR, Lovejoy FH |title = The relative severity of acute versus chronic salicylate poisoning in children: a clinical comparison |journal = Pediatrics |volume = 70 |issue = 4 |pages = 566–9 |date = October 1982 |doi = 10.1542/peds.70.4.566 |pmid = 7122154 |s2cid = 12738659 }} (primary source)</ref> Toxicity is managed with a number of potential treatments, including [[activated charcoal]], intravenous dextrose and normal saline, [[sodium bicarbonate]], and [[Kidney dialysis|dialysis]].<ref>{{ |
Aspirin overdose can be acute or chronic. In acute poisoning, a single large dose is taken; in chronic poisoning, higher than normal doses are taken over a period of time. Acute overdose has a [[mortality rate]] of 2%. Chronic overdose is more commonly lethal, with a mortality rate of 25%;<ref>{{cite web |vauthors = Kreplick LW |year=2001 |title=Salicylate toxicity in emergency medicine |publisher=[[Medscape]] |url=http://misc.medscape.com/pi/android/medscapeapp/html/A818242-business.html |url-status=live |archive-url=https://web.archive.org/web/20120831184805/http://misc.medscape.com/pi/android/medscapeapp/html/A818242-business.html |archive-date=31 August 2012}}</ref> chronic overdose may be especially severe in children.<ref name="Pediatrics1982-gaudreault">{{cite journal |vauthors = Gaudreault P, Temple AR, Lovejoy FH |title = The relative severity of acute versus chronic salicylate poisoning in children: a clinical comparison |journal = Pediatrics |volume = 70 |issue = 4 |pages = 566–9 |date = October 1982 |doi = 10.1542/peds.70.4.566 |pmid = 7122154 |s2cid = 12738659 }} (primary source)</ref> Toxicity is managed with a number of potential treatments, including [[activated charcoal]], intravenous dextrose and normal saline, [[sodium bicarbonate]], and [[Kidney dialysis|dialysis]].<ref>{{cite book |title=Rosen's emergency medicine: concepts and clinical practice |vauthors = Marx J |year=2006 |publisher=Mosby/Elsevier |isbn=978-0-323-02845-5 |page=[https://archive.org/details/rosensemergencym0002unse/page/2242 2242] |url=https://archive.org/details/rosensemergencym0002unse/page/2242 }}</ref> The diagnosis of poisoning usually involves measurement of plasma salicylate, the active metabolite of aspirin, by automated spectrophotometric methods. Plasma salicylate levels in general range from 30 to 100{{nbsp}}mg/L after usual therapeutic doses, 50–300{{nbsp}}mg/L in people taking high doses and 700–1400{{nbsp}}mg/L following acute overdose. Salicylate is also produced as a result of exposure to [[bismuth subsalicylate]], [[methyl salicylate]], and [[sodium salicylate]].<ref>{{cite journal |vauthors = Morra P, Bartle WR, Walker SE, Lee SN, Bowles SK, Reeves RA |title = Serum concentrations of salicylic acid following topically applied salicylate derivatives |journal = The Annals of Pharmacotherapy |volume = 30 |issue = 9 |pages = 935–40 |date = September 1996 |pmid = 8876850 |doi = 10.1177/106002809603000903 |s2cid = 9843820 }}</ref><ref>{{cite book |vauthors = Baselt R |title=Disposition of toxic drugs and chemicals in man |edition=9th |publisher=Biomedical Publications |location=Seal Beach, California |year=2011 |pages=20–23|isbn=978-0-9626523-8-7 }}</ref> |
||
=== Interactions === |
=== Interactions === |
||
| Line 374: | Line 367: | ||
==Research== |
==Research== |
||
The ISIS-2 trial demonstrated that aspirin at doses of 160{{nbsp}}mg daily for one month, decreased the mortality by 21% of participants with a suspected myocardial infarction in the first five weeks.<ref name="The Lancet-1988">{{cite journal |date=August 1988 |journal=The Lancet |volume=332 |issue=8607 |pages=349–360 |doi=10.1016/s0140-6736(88)92833-4 |issn=0140-6736|title=Randomised Trial of Intravenous Streptokinase, Oral Aspirin, Both, or Neither Among 17,187 Cases of Suspected Acute Myocardial Infarction: Isis-2 |s2cid=21071664 | pmid = 2899772 }}</ref> A single daily dose of 324{{nbsp}}mg of aspirin for 12 weeks has a highly protective effect against acute myocardial infarction and death in men with unstable angina.<ref name="Lewis-1983">{{cite journal | vauthors = Lewis HD, Davis JW, Archibald DG, Steinke WE, Smitherman TC, Doherty JE, Schnaper HW, LeWinter MM, Linares E, Pouget JM, Sabharwal SC, Chesler E, DeMots H |
The ISIS-2 trial demonstrated that aspirin at doses of 160{{nbsp}}mg daily for one month, decreased the mortality by 21% of participants with a suspected myocardial infarction in the first five weeks.<ref name="The Lancet-1988">{{cite journal |date=August 1988 |journal=The Lancet |volume=332 |issue=8607 |pages=349–360 |doi=10.1016/s0140-6736(88)92833-4 |issn=0140-6736|title=Randomised Trial of Intravenous Streptokinase, Oral Aspirin, Both, or Neither Among 17,187 Cases of Suspected Acute Myocardial Infarction: Isis-2 |s2cid=21071664 | pmid = 2899772 }}</ref> A single daily dose of 324{{nbsp}}mg of aspirin for 12 weeks has a highly protective effect against acute myocardial infarction and death in men with unstable angina.<ref name="Lewis-1983">{{cite journal | vauthors = Lewis HD, Davis JW, Archibald DG, Steinke WE, Smitherman TC, Doherty JE, Schnaper HW, LeWinter MM, Linares E, Pouget JM, Sabharwal SC, Chesler E, DeMots H |date=August 1983 |title=Protective effects of aspirin against acute myocardial infarction and death in men with unstable angina. Results of a Veterans Administration Cooperative Study |journal=New England Journal of Medicine |volume=309 |issue=7 |pages=396–403 |doi=10.1056/NEJM198308183090703 |issn=0028-4793 |pmid=6135989 }}</ref> |
||
=== Bipolar disorder === |
=== Bipolar disorder === |
||
| Line 380: | Line 373: | ||
===Infectious diseases=== |
===Infectious diseases=== |
||
Several studies investigated the anti-infective properties of aspirin for bacterial, viral and parasitic infections. Aspirin was demonstrated to limit platelet activation induced by ''Staphylococcus aureus'' and ''Enterococcus faecalis'' and to reduce streptococcal adhesion to heart valves. In patients with tuberculous meningitis, the addition of aspirin reduced the risk of new cerebral infarction [RR = 0.52 (0.29-0.92)]. A role of aspirin on bacterial and fungal biofilm is also being supported by growing evidence.<ref>{{cite journal| vauthors = Di Bella S, Luzzati R, Principe L, Zerbato V, Meroni E, Giuffrè M, Crocè LS, Merlo M, Perotto M, Dolso E, Maurel C |
Several studies investigated the anti-infective properties of aspirin for bacterial, viral and parasitic infections. Aspirin was demonstrated to limit platelet activation induced by ''Staphylococcus aureus'' and ''Enterococcus faecalis'' and to reduce streptococcal adhesion to heart valves. In patients with tuberculous meningitis, the addition of aspirin reduced the risk of new cerebral infarction [RR = 0.52 (0.29-0.92)]. A role of aspirin on bacterial and fungal biofilm is also being supported by growing evidence.<ref>{{cite journal| vauthors = Di Bella S, Luzzati R, Principe L, Zerbato V, Meroni E, Giuffrè M, Crocè LS, Merlo M, Perotto M, Dolso E, Maurel C |date=25 January 2022 |title=Aspirin and Infection: A Narrative Review |journal=Biomedicines |volume=10 |issue=2 |pages=263 |doi=10.3390/biomedicines10020263 | pmid = 35203473 | pmc = 8868581 |issn=2227-9059 |doi-access=free}}</ref> |
||
===Cancer prevention=== |
===Cancer prevention=== |
||
Evidence from observational studies were conflicting on the effect of aspirin in breast cancer prevention,<ref>{{cite journal | vauthors = Cao Y, Tan A | title = Aspirin might reduce the incidence of breast cancer: An updated meta-analysis of 38 observational studies | journal = Medicine | volume = 99 | issue = 38 | pages = e21917 | date = September 2020 | pmid = 32957311 | doi = 10.1097/md.0000000000021917 | pmc = 7505405 }}</ref> a randomized controlled trial showed that aspirin had no significant effect in reducing breast cancer <ref>{{cite journal | vauthors = Cook NR, Lee IM, Gaziano JM, Gordon D, Ridker PM, Manson JE, Hennekens CH, Buring JE |
Evidence from observational studies were conflicting on the effect of aspirin in breast cancer prevention,<ref>{{cite journal | vauthors = Cao Y, Tan A | title = Aspirin might reduce the incidence of breast cancer: An updated meta-analysis of 38 observational studies | journal = Medicine | volume = 99 | issue = 38 | pages = e21917 | date = September 2020 | pmid = 32957311 | doi = 10.1097/md.0000000000021917 | pmc = 7505405 }}</ref> a randomized controlled trial showed that aspirin had no significant effect in reducing breast cancer <ref>{{cite journal | vauthors = Cook NR, Lee IM, Gaziano JM, Gordon D, Ridker PM, Manson JE, Hennekens CH, Buring JE | title = Low-dose aspirin in the primary prevention of cancer: the Women's Health Study: a randomized controlled trial | journal = JAMA | volume = 294 | issue = 1 | pages = 47–55 | date = July 2005 | pmid = 15998890 | doi = 10.1001/jama.294.1.47 }}</ref> thus further studies are needed to clarify aspirin effect in cancer prevention. |
||
=== In gardening === |
=== In gardening === |
||
There are |
There are many anecdotal reportings that aspirin can improve plant's growth and resistance<ref>{{cite web |title=Aspirin Water Helps Plants |url=https://cybercemetery.unt.edu/archive/allcollections/20090117082434/http://www.plantea.com/plant-aspirin.htm |access-date= |website=cybercemetery.unt.edu}}</ref><ref>{{cite web |title=Gardens: drug therapy for plants {{!}} Gardening advice |url=https://amp.theguardian.com/lifeandstyle/2016/jan/31/drug-therapy-for-plants |access-date= |website=[[The Guardian]]}}</ref> though most research involved [[salicylic acid]] instead of aspirin.<ref>{{cite web |title=Priming Plant Defenses with Aspirin-like Compound : USDA ARS |url=https://www.ars.usda.gov/news-events/news/research-news/2014/priming-plant-defenses-with-aspirin-like-compound/ |access-date= |website=www.ars.usda.gov}}</ref> |
||
== Veterinary medicine == |
== Veterinary medicine == |
||
Aspirin is sometimes used in veterinary medicine as an [[anticoagulant]] or to [[analgesic|relieve pain]] associated with musculoskeletal inflammation or [[osteoarthritis]]. Aspirin should only be given to animals under the direct supervision of a [[veterinarian]], as adverse effects—including gastrointestinal issues—are common. An aspirin overdose in any species may result in [[salicylate poisoning]], characterized by hemorrhaging, seizures, coma, and even death.<ref name="Edwards-2016">{{ |
Aspirin is sometimes used in veterinary medicine as an [[anticoagulant]] or to [[analgesic|relieve pain]] associated with musculoskeletal inflammation or [[osteoarthritis]]. Aspirin should only be given to animals under the direct supervision of a [[veterinarian]], as adverse effects—including gastrointestinal issues—are common. An aspirin overdose in any species may result in [[salicylate poisoning]], characterized by hemorrhaging, seizures, coma, and even death.<ref name="Edwards-2016">{{cite web|url=http://www.merckvetmanual.com/pharmacology/anti-inflammatory-agents/nonsteroidal-anti-inflammatory-drugs#v3337669|title=Nonsteroidal Anti-inflammatory Drugs: Aspirin |vauthors = Edwards SH |work=Merck Veterinary Manual|access-date=20 January 2018|archive-url=https://web.archive.org/web/20161218082147/http://www.merckvetmanual.com/pharmacology/anti-inflammatory-agents/nonsteroidal-anti-inflammatory-drugs#v3337669|archive-date=18 December 2016|url-status=dead }}</ref> |
||
Dogs are better able to tolerate aspirin than cats are.<ref name="Merck" /> Cats metabolize aspirin slowly because they lack the [[glucuronide]] conjugates that aid in the excretion of aspirin, making it potentially toxic if dosing is not spaced out properly.<ref name="Edwards-2016" /><ref>{{cite book|title=Feline internal medicine secrets|publisher=Hanley & Belfus|year=2001|isbn=978-1-56053-461-7 |veditors = Lappin MR |location=Philadelphia|page=160}}</ref> No clinical signs of toxicosis occurred when cats were given 25{{nbsp}}mg/kg of aspirin every 48 hours for 4 weeks,<ref name="Merck">{{cite web|url=http://www.merckmanuals.com/vet/toxicology/toxicities_from_human_drugs/analgesics_toxicity.html|title=Analgesics (toxicity) |publisher=Merck|archive-url= https://web.archive.org/web/20150411095033/http://www.merckmanuals.com/vet/toxicology/toxicities_from_human_drugs/analgesics_toxicity.html |archive-date=11 April 2015 |url-status=live|access-date=19 January 2018}}</ref> but the recommended dose for relief of pain and fever and for treating [[thrombophilia|blood clotting diseases]] in cats is 10{{nbsp}}mg/kg every 48 hours to allow for metabolization.<ref name="Edwards-2016" /><ref>{{cite web|url=http://www.ansci.cornell.edu/plants/toxcat/toxcat.html|title=Plants poisonous to livestock|publisher=Cornell University Department of Animal Science|archive-url=https://web.archive.org/web/20150816192109/http://www.ansci.cornell.edu/plants/toxcat/toxcat.html|archive-date=16 August 2015|url-status=live|access-date=3 March 2016}}</ref> |
Dogs are better able to tolerate aspirin than cats are.<ref name="Merck" /> Cats metabolize aspirin slowly because they lack the [[glucuronide]] conjugates that aid in the excretion of aspirin, making it potentially toxic if dosing is not spaced out properly.<ref name="Edwards-2016" /><ref>{{cite book|title=Feline internal medicine secrets|publisher=Hanley & Belfus|year=2001|isbn=978-1-56053-461-7 |veditors = Lappin MR |location=Philadelphia|page=160}}</ref> No clinical signs of toxicosis occurred when cats were given 25{{nbsp}}mg/kg of aspirin every 48 hours for 4 weeks,<ref name="Merck">{{cite web|url=http://www.merckmanuals.com/vet/toxicology/toxicities_from_human_drugs/analgesics_toxicity.html|title=Analgesics (toxicity) |publisher=Merck|archive-url= https://web.archive.org/web/20150411095033/http://www.merckmanuals.com/vet/toxicology/toxicities_from_human_drugs/analgesics_toxicity.html |archive-date=11 April 2015 |url-status=live|access-date=19 January 2018}}</ref> but the recommended dose for relief of pain and fever and for treating [[thrombophilia|blood clotting diseases]] in cats is 10{{nbsp}}mg/kg every 48 hours to allow for metabolization.<ref name="Edwards-2016" /><ref>{{cite web|url=http://www.ansci.cornell.edu/plants/toxcat/toxcat.html|title=Plants poisonous to livestock|publisher=Cornell University Department of Animal Science|archive-url=https://web.archive.org/web/20150816192109/http://www.ansci.cornell.edu/plants/toxcat/toxcat.html|archive-date=16 August 2015|url-status=live|access-date=3 March 2016}}</ref> |
||
==See also== |
|||
| ⚫ | |||
*[[Fluoroaspirin]] |
|||
== References == |
== References == |
||
| Line 406: | Line 395: | ||
* {{cite journal | vauthors = Desborough MJ, Keeling DM | title = The aspirin story - from willow to wonder drug | journal = British Journal of Haematology | volume = 177 | issue = 5 | pages = 674–683 | date = June 2017 | pmid = 28106908 | doi = 10.1111/bjh.14520 | s2cid = 46794541 | doi-access = free }} |
* {{cite journal | vauthors = Desborough MJ, Keeling DM | title = The aspirin story - from willow to wonder drug | journal = British Journal of Haematology | volume = 177 | issue = 5 | pages = 674–683 | date = June 2017 | pmid = 28106908 | doi = 10.1111/bjh.14520 | s2cid = 46794541 | doi-access = free }} |
||
* {{cite journal | vauthors = McTavish JR | title = What's in a name? Aspirin and the American Medical Association | journal = Bulletin of the History of Medicine | volume = 61 | issue = 3 | pages = 343–66 | date = 1987 | pmid = 3311247 | doi = | jstor = 44442097 }} |
* {{cite journal | vauthors = McTavish JR | title = What's in a name? Aspirin and the American Medical Association | journal = Bulletin of the History of Medicine | volume = 61 | issue = 3 | pages = 343–66 | date = 1987 | pmid = 3311247 | doi = | jstor = 44442097 }} |
||
| ⚫ | * {{cite encyclopedia |vauthors=Ling G |title=Aspirin |url=http://www.madehow.com/Volume-1/Aspirin.html |encyclopedia=How Products Are Made |volume=1 |publisher=Thomson Gale |year=2005}} |
||
{{refend}} |
{{refend}} |
||
== External links == |
== External links == |
||
{{Commons}} |
{{Commons}} |
||
* {{cite web |title=Aspirin |url=https://druginfo.nlm.nih.gov/drugportal/name/aspirin |work=Drug Information Portal |publisher=U.S. National Library of Medicine}} |
|||
| ⚫ | * {{cite encyclopedia |vauthors=Ling G |title=Aspirin |url=http://www.madehow.com/Volume-1/Aspirin.html |encyclopedia=How Products Are Made |volume=1 |publisher=Thomson Gale |year=2005}} |
||
{{ATC navboxes|B01|D10|M01A|N02A}} |
{{ATC navboxes|B01|D10|M01A|N02A}} |
||
{{Salicylates}} |
{{Salicylates}} |
||
{{Prostanoid signaling modulators}} |
{{Prostanoid signaling modulators}} |
||
| ⚫ | |||
{{Authority control}} |
{{Authority control}} |
||
| Line 424: | Line 413: | ||
[[Category:Acetylsalicylic acids]] |
[[Category:Acetylsalicylic acids]] |
||
[[Category:Antiplatelet drugs]] |
[[Category:Antiplatelet drugs]] |
||
[[Category: |
[[Category:Drugs developed by Bayer]] |
||
[[Category:Brands that became generic]] |
[[Category:Brands that became generic]] |
||
[[Category:Chemical substances for emergency medicine]] |
[[Category:Chemical substances for emergency medicine]] |
||
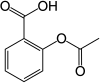 | |
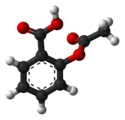 | |
| Clinical data | |
|---|---|
| Pronunciation | /əˌsiːtəlˌsælɪˈsɪlɪk/ |
| Trade names | Bayer Aspirin, others |
| Other names |
|
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a682878 |
| License data | |
| Pregnancy category |
|
| Routes of administration | Oral, rectal |
| Drug class | Nonsteroidal anti-inflammatory drug (NSAID) |
| ATC code | |
| Legal status | |
| Legal status |
|
| Pharmacokinetic data | |
| Bioavailability | 80–100%[6] |
| Protein binding | 80–90%[7] |
| Metabolism | Liver (CYP2C19 and possibly CYP3A), some is also hydrolysed to salicylate in the gut wall.[7] |
| Elimination half-life | Dose-dependent; 2–3 h for low doses (100 mg or less), 15–30 h for larger doses.[7] |
| Excretion | Urine (80–100%), sweat, saliva, feces[6] |
| Identifiers | |
| |
| CAS Number |
|
| PubChem CID | |
| IUPHAR/BPS | |
| DrugBank |
|
| ChemSpider |
|
| UNII | |
| KEGG |
|
| ChEBI | |
| ChEMBL |
|
| PDB ligand | |
| CompTox Dashboard (EPA) | |
| ECHA InfoCard | 100.000.059 |
| Chemical and physical data | |
| Formula | C9H8O4 |
| Molar mass | 180.159 g·mol−1 |
| 3D model (JSmol) | |
| Density | 1.40 g/cm3 |
| Melting point | 135 °C (275 °F) [9] |
| Boiling point | 140 °C (284 °F) (decomposes) |
| Solubility in water | 3 g/L |
| |
| |
| (verify) | |
Aspirin, also known as acetylsalicylic acid (ASA), is a nonsteroidal anti-inflammatory drug (NSAID) used to reduce pain, fever, and/or inflammation, and as an antithrombotic.[10] Specific inflammatory conditions which aspirin is used to treat include Kawasaki disease, pericarditis, and rheumatic fever.[10]
Aspirin is also used long-term to help prevent further heart attacks, ischaemic strokes, and blood clots in people at high risk.[10] For pain or fever, effects typically begin within 30 minutes.[10] Aspirin works similarly to other NSAIDs but also suppresses the normal functioning of platelets.[10]
One common adverse effect is an upset stomach.[10] More significant side effects include stomach ulcers, stomach bleeding, and worsening asthma.[10] Bleeding risk is greater among those who are older, drink alcohol, take other NSAIDs, or are on other blood thinners.[10] Aspirin is not recommended in the last part of pregnancy.[10] It is not generally recommended in children with infections because of the risk of Reye syndrome.[10] High doses may result in ringing in the ears.[10]
Aprecursor to aspirin found in the bark of the willow tree (genus Salix) has been used for its health effects for at least 2,400 years.[11][12] In 1853, chemist Charles Frédéric Gerhardt treated the medicine sodium salicylate with acetyl chloride to produce acetylsalicylic acid for the first time.[13] Over the next 50 years, other chemists, mostly of the German company Bayer, established the chemical structure and devised more efficient production methods.[13]: 69–75
Aspirin is available without medical prescription as a proprietary or generic medication[10] in most jurisdictions. It is one of the most widely used medications globally, with an estimated 40,000 tonnes (44,000 tons) (50 to 120 billion pills)[clarification needed] consumed each year,[11][14] and is on the World Health Organization's List of Essential Medicines.[15] In 2021, it was the 34th most commonly prescribed medication in the United States, with more than 17 million prescriptions.[16][17]
In 1897, scientists at the Bayer company began studying acetylsalicylic acid as a less-irritating replacement medication for common salicylate medicines.[13]: 69–75 [18] By 1899, Bayer had named it "Aspirin" and was selling it around the world.[19]
Aspirin's popularity grew over the first half of the 20th century, leading to competition between many brands and formulations.[20] The word Aspirin was Bayer's brand name; however, their rights to the trademark were lost or sold in many countries.[20] The name is ultimately a blend of the prefix a(cetyl) + spir Spiraea, the meadowsweet plant genus from which the acetylsalicylic acid was originally derived at Bayer + -in, the common chemical suffix.[citation needed]
Aspirin decomposes rapidly in solutions of ammonium acetate or the acetates, carbonates, citrates, or hydroxides of the alkali metals. It is stable in dry air, but gradually hydrolyses in contact with moisture to acetic and salicylic acids. In solution with alkalis, the hydrolysis proceeds rapidly and the clear solutions formed may consist entirely of acetate and salicylate.[21]
Like flour mills, factories producing aspirin tablets must control the amount of the powder that becomes airborne inside the building, because the powder-air mixture can be explosive. The National Institute for Occupational Safety and Health (NIOSH) has set a recommended exposure limit in the United States of 5 mg/m3 (time-weighted average).[22] In 1989, the Occupational Safety and Health Administration (OSHA) set a legal permissible exposure limit for aspirin of 5 mg/m3, but this was vacated by the AFL-CIO v. OSHA decision in 1993.[23]
The synthesis of aspirin is classified as an esterification reaction. Salicylic acid is treated with acetic anhydride, an acid derivative, causing a chemical reaction that turns salicylic acid's hydroxyl group into an ester group (R-OH → R-OCOCH3). This process yields aspirin and acetic acid, which is considered a byproduct of this reaction. Small amounts of sulfuric acid (and occasionally phosphoric acid) are almost always used as a catalyst. This method is commonly demonstrated in undergraduate teaching labs.[24]

Reaction between acetic acid and salicylic acid can also form aspirin but this esterification reaction is reversible and the presence of water can lead to hydrolysis of the aspirin. So, an anhydrous reagent is preferred.[25]
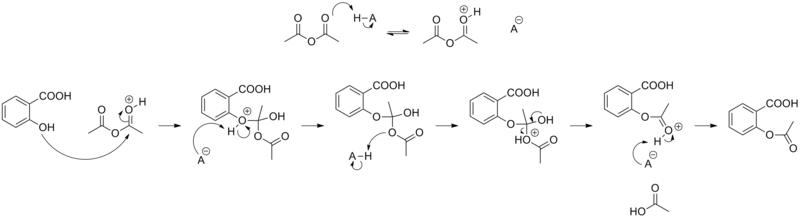
Formulations containing high concentrations of aspirin often smell like vinegar[26] because aspirin can decompose through hydrolysis in moist conditions, yielding salicylic and acetic acids.[27]
Aspirin, an acetyl derivative of salicylic acid, is a white, crystalline, weakly acidic substance, which melts at 136 °C (277 °F),[9] and decomposes around 140 °C (284 °F).[28] Its acid dissociation constant (pKa) is 3.5 at 25 °C (77 °F).[29]
Polymorphism, or the ability of a substance to form more than one crystal structure, is important in the development of pharmaceutical ingredients. Many drugs receive regulatory approval for only a single crystal form or polymorph.
There was only one proven polymorph Form I of aspirin, though the existence of another polymorph was debated since the 1960s, and one report from 1981 reported that when crystallized in the presence of aspirin anhydride, the diffractogram of aspirin has weak additional peaks. Though at the time it was dismissed as mere impurity, it was, in retrospect, Form II aspirin.[30]
Form II was reported in 2005,[31][32] found after attempted co-crystallization of aspirin and levetiracetam from hot acetonitrile.
In form I, pairs of aspirin molecules form centrosymmetric dimers through the acetyl groups with the (acidic) methyl proton to carbonyl hydrogen bonds. In form II, each aspirin molecule forms the same hydrogen bonds, but with two neighbouring molecules instead of one. With respect to the hydrogen bonds formed by the carboxylic acid groups, both polymorphs form identical dimer structures. The aspirin polymorphs contain identical 2-dimensional sections and are therefore more precisely described as polytypes.[33]
Pure Form II aspirin could be prepared by seeding the batch with aspirin anhydrate in 15% weight.[30]
In 1971, British pharmacologist John Robert Vane, then employed by the Royal College of Surgeons in London, showed aspirin suppressed the production of prostaglandins and thromboxanes.[34][35] For this discovery he was awarded the 1982 Nobel Prize in Physiology or Medicine, jointly with Sune Bergström and Bengt Ingemar Samuelsson.[36]
Aspirin's ability to suppress the production of prostaglandins and thromboxanes is due to its irreversible inactivation of the cyclooxygenase (COX; officially known as prostaglandin-endoperoxide synthase, PTGS) enzyme required for prostaglandin and thromboxane synthesis. Aspirin acts as an acetylating agent where an acetyl group is covalently attached to a serine residue in the active site of the COX enzyme (Suicide inhibition). This makes aspirin different from other NSAIDs (such as diclofenac and ibuprofen), which are reversible inhibitors.
Low-dose aspirin use irreversibly blocks the formation of thromboxane A2 in platelets, producing an inhibitory effect on platelet aggregation during the lifetime of the affected platelet (8–9 days). This antithrombotic property makes aspirin useful for reducing the incidence of heart attacks in people who have had a heart attack, unstable angina, ischemic stroke or transient ischemic attack.[37]40 mg of aspirin a day is able to inhibit a large proportion of maximum thromboxane A2 release provoked acutely, with the prostaglandin I2 synthesis being little affected; however, higher doses of aspirin are required to attain further inhibition.[38]
Prostaglandins, local hormones produced in the body, have diverse effects, including the transmission of pain information to the brain, modulation of the hypothalamic thermostat, and inflammation. Thromboxanes are responsible for the aggregation of platelets that form blood clots. Heart attacks are caused primarily by blood clots, and low doses of aspirin are seen as an effective medical intervention to prevent a second acute myocardial infarction.[39]
At least two different types of cyclooxygenases, COX-1 and COX-2, are acted on by aspirin. Aspirin irreversibly inhibits COX-1 and modifies the enzymatic activity of COX-2. COX-2 normally produces prostanoids, most of which are proinflammatory. Aspirin-modified COX-2 (aka prostaglandin-endoperoxide synthase 2 or PTGS2) produces lipoxins, most of which are anti-inflammatory.[40][verification needed] Newer NSAID drugs, COX-2 inhibitors (coxibs), have been developed to inhibit only COX-2, with the intent to reduce the incidence of gastrointestinal side effects.[14]
Several COX-2 inhibitors, such as rofecoxib (Vioxx), have been withdrawn from the market, after evidence emerged that COX-2 inhibitors increase the risk of heart attack and stroke.[41][42] Endothelial cells lining the microvasculature in the body are proposed to express COX-2, and, by selectively inhibiting COX-2, prostaglandin production (specifically, PGI2; prostacyclin) is downregulated with respect to thromboxane levels, as COX-1 in platelets is unaffected. Thus, the protective anticoagulative effect of PGI2 is removed, increasing the risk of thrombus and associated heart attacks and other circulatory problems. Since platelets have no DNA, they are unable to synthesize new COX once aspirin has irreversibly inhibited the enzyme, an important difference as compared with reversible inhibitors.
Furthermore, aspirin, while inhibiting the ability of COX-2 to form pro-inflammatory products such as the prostaglandins, converts this enzyme's activity from a prostaglandin-forming cyclooxygenase to a lipoxygenase-like enzyme: aspirin-treated COX-2 metabolizes a variety of polyunsaturated fatty acids to hydroperoxy products which are then further metabolized to specialized proresolving mediators such as the aspirin-triggered lipoxins, aspirin-triggered resolvins, and aspirin-triggered maresins. These mediators possess potent anti-inflammatory activity. It is proposed that this aspirin-triggered transition of COX-2 from cyclooxygenase to lipoxygenase activity and the consequential formation of specialized proresolving mediators contributes to the anti-inflammatory effects of aspirin.[43][44][45]
Aspirin has been shown to have at least three additional modes of action. It uncouples oxidative phosphorylation in cartilaginous (and hepatic) mitochondria, by diffusing from the inner membrane space as a proton carrier back into the mitochondrial matrix, where it ionizes once again to release protons.[46] Aspirin buffers and transports the protons. When high doses are given, it may actually cause fever, owing to the heat released from the electron transport chain, as opposed to the antipyretic action of aspirin seen with lower doses. In addition, aspirin induces the formation of NO-radicals in the body, which have been shown in mice to have an independent mechanism of reducing inflammation. This reduced leukocyte adhesion is an important step in the immune response to infection; however, evidence is insufficient to show aspirin helps to fight infection.[47] More recent data also suggest salicylic acid and its derivatives modulate signalling through NF-κB.[48] NF-κB, a transcription factor complex, plays a central role in many biological processes, including inflammation.[49][50][51]
Aspirin is readily broken down in the body to salicylic acid, which itself has anti-inflammatory, antipyretic, and analgesic effects. In 2012, salicylic acid was found to activate AMP-activated protein kinase, which has been suggested as a possible explanation for some of the effects of both salicylic acid and aspirin.[52][53] The acetyl portion of the aspirin molecule has its own targets. Acetylation of cellular proteins is a well-established phenomenon in the regulation of protein function at the post-translational level. Aspirin is able to acetylate several other targets in addition to COX isoenzymes.[54][55] These acetylation reactions may explain many hitherto unexplained effects of aspirin.[56]
This section needs expansion. You can help by adding to it. (January 2023)
|
Aspirin is produced in many formulations, with some differences in effect. In particular, aspirin can cause gastrointestinal bleeding, and formulations are sought which deliver the benefits of aspirin while mitigating harmful bleeding. Formulations may be combined (e.g., buffered + vitamin C).
Acetylsalicylic acid is a weak acid, and very little of it is ionized in the stomach after oral administration. Acetylsalicylic acid is quickly absorbed through the cell membrane in the acidic conditions of the stomach. The increased pH and larger surface area of the small intestine causes aspirin to be absorbed more slowly there, as more of it is ionized. Owing to the formation of concretions, aspirin is absorbed much more slowly during overdose, and plasma concentrations can continue to rise for up to 24 hours after ingestion.[58][59][60]
About 50–80% of salicylate in the blood is bound to human serum albumin, while the rest remains in the active, ionized state; protein binding is concentration-dependent. Saturation of binding sites leads to more free salicylate and increased toxicity. The volume of distribution is 0.1–0.2 L/kg. Acidosis increases the volume of distribution because of enhancement of tissue penetration of salicylates.[60]
As much as 80% of therapeutic doses of salicylic acid is metabolized in the liver. Conjugation with glycine forms salicyluric acid, and with glucuronic acid to form two different glucuronide esters. The conjugate with the acetyl group intact is referred to as the acyl glucuronide; the deacetylated conjugate is the phenolic glucuronide. These metabolic pathways have only a limited capacity. Small amounts of salicylic acid are also hydroxylated to gentisic acid. With large salicylate doses, the kinetics switch from first-order to zero-order, as metabolic pathways become saturated and renal excretion becomes increasingly important.[60]
Salicylates are excreted mainly by the kidneys as salicyluric acid (75%), free salicylic acid (10%), salicylic phenol (10%), and acyl glucuronides (5%), gentisic acid (< 1%), and 2,3-dihydroxybenzoic acid.[61] When small doses (less than 250 mg in an adult) are ingested, all pathways proceed by first-order kinetics, with an elimination half-life of about 2.0 h to 4.5 h.[62][63] When higher doses of salicylate are ingested (more than 4 g), the half-life becomes much longer (15 h to 30 h),[64] because the biotransformation pathways concerned with the formation of salicyluric acid and salicyl phenolic glucuronide become saturated.[65] Renal excretion of salicylic acid becomes increasingly important as the metabolic pathways become saturated, because it is extremely sensitive to changes in urinary pH. A 10- to 20-fold increase in renal clearance occurs when urine pH is increased from 5 to 8. The use of urinary alkalinization exploits this particular aspect of salicylate elimination.[66] It was found that short-term aspirin use in therapeutic doses might precipitate reversible acute kidney injury when the patient was ill with glomerulonephritisorcirrhosis.[67] Aspirin for some patients with chronic kidney disease and some children with congestive heart failure was contraindicated.[67]

Medicines made from willow and other salicylate-rich plants appear in clay tablets from ancient Sumer as well as the Ebers Papyrus from ancient Egypt.[13]: 8–13 [20] Hippocrates referred to the use of salicylic tea to reduce fevers around 400 BC, and willow bark preparations were part of the pharmacopoeia of Western medicine in classical antiquity and the Middle Ages.[20] Willow bark extract became recognized for its specific effects on fever, pain, and inflammation in the mid-eighteenth century.[68] By the nineteenth century, pharmacists were experimenting with and prescribing a variety of chemicals related to salicylic acid, the active component of willow extract.[13]: 46–55

In 1853, chemist Charles Frédéric Gerhardt treated sodium salicylate with acetyl chloride to produce acetylsalicylic acid for the first time;[13]: 46–48 in the second half of the 19th century, other academic chemists established the compound's chemical structure and devised more efficient methods of synthesis. In 1897, scientists at the drug and dye firm Bayer began investigating acetylsalicylic acid as a less-irritating replacement for standard common salicylate medicines, and identified a new way to synthesize it.[13]: 69–75 By 1899, Bayer had dubbed this drug Aspirin and was selling it globally.[19]: 27 The word Aspirin was Bayer's brand name, rather than the generic name of the drug; however, Bayer's rights to the trademark were lost or sold in many countries. Aspirin's popularity grew over the first half of the 20th century leading to fierce competition with the proliferation of aspirin brands and products.[20]
Aspirin's popularity declined after the development of acetaminophen/paracetamol in 1956 and ibuprofen in 1962. In the 1960s and 1970s, John Vane and others discovered the basic mechanism of aspirin's effects,[13]: 226–231 while clinical trials and other studies from the 1960s to the 1980s established aspirin's efficacy as an anti-clotting agent that reduces the risk of clotting diseases.[13]: 247–257 The initial large studies on the use of low-dose aspirin to prevent heart attacks that were published in the 1970s and 1980s helped spur reform in clinical research ethics and guidelines for human subject research and US federal law, and are often cited as examples of clinical trials that included only men, but from which people drew general conclusions that did not hold true for women.[69][70][71]
Aspirin sales revived considerably in the last decades of the 20th century, and remain strong in the 21st century with widespread use as a preventive treatment for heart attacks and strokes.[13]: 267–269
Bayer lost its trademark for Aspirin in the United States and some other countries in actions taken between 1918 and 1921 because it had failed to use the name for its own product correctly and had for years allowed the use of "Aspirin" by other manufacturers without defending the intellectual property rights.[72] Today, aspirin is a generic trademark in many countries.[73][74] Aspirin, with a capital "A", remains a registered trademark of Bayer in Germany, Canada, Mexico, and in over 80 other countries, for acetylsalicylic acid in all markets, but using different packaging and physical aspects for each.[75][76]
Aspirin is used in the treatment of a number of conditions, including fever, pain, rheumatic fever, and inflammatory conditions, such as rheumatoid arthritis, pericarditis, and Kawasaki disease.[10] Lower doses of aspirin have also been shown to reduce the risk of death from a heart attack, or the risk of stroke in people who are at high risk or who have cardiovascular disease, but not in elderly people who are otherwise healthy.[79][80][81][82][83] There is evidence that aspirin is effective at preventing colorectal cancer, though the mechanisms of this effect are unclear.[84] In the United States, the selective initiation of low-dose aspirin, based on an individualised assessment, has been deemed reasonable for the primary prevention of cardiovascular disease in people aged between 40 and 59 who have a 10% or greater risk of developing cardiovascular disease over the next 10 years and are not at an increased risk of bleeding.[85]
Aspirin is an effective analgesic for acute pain, although it is generally considered inferior to ibuprofen because aspirin is more likely to cause gastrointestinal bleeding.[86] Aspirin is generally ineffective for those pains caused by muscle cramps, bloating, gastric distension, or acute skin irritation.[87] As with other NSAIDs, combinations of aspirin and caffeine provide slightly greater pain relief than aspirin alone.[88] Effervescent formulations of aspirin relieve pain faster than aspirin in tablets,[89] which makes them useful for the treatment of migraines.[90] Topical aspirin may be effective for treating some types of neuropathic pain.[91]
Aspirin, either by itself or in a combined formulation, effectively treats certain types of a headache, but its efficacy may be questionable for others. Secondary headaches, meaning those caused by another disorder or trauma, should be promptly treated by a medical provider. Among primary headaches, the International Classification of Headache Disorders distinguishes between tension headache (the most common), migraine, and cluster headache. Aspirin or other over-the-counter analgesics are widely recognized as effective for the treatment of tension headaches.[92] Aspirin, especially as a component of an aspirin/paracetamol/caffeine combination, is considered a first-line therapy in the treatment of migraine, and comparable to lower doses of sumatriptan. It is most effective at stopping migraines when they are first beginning.[93]
Like its ability to control pain, aspirin's ability to control fever is due to its action on the prostaglandin system through its irreversible inhibition of COX.[94] Although aspirin's use as an antipyretic in adults is well established, many medical societies and regulatory agencies, including the American Academy of Family Physicians, the American Academy of Pediatrics, and the Food and Drug Administration, strongly advise against using aspirin for the treatment of fever in children because of the risk of Reye's syndrome, a rare but often fatal illness associated with the use of aspirin or other salicylates in children during episodes of viral or bacterial infection.[95][96][97] Because of the risk of Reye's syndrome in children, in 1986, the US Food and Drug Administration (FDA) required labeling on all aspirin-containing medications advising against its use in children and teenagers.[98]
Aspirin is used as an anti-inflammatory agent for both acute and long-term inflammation,[99] as well as for the treatment of inflammatory diseases, such as rheumatoid arthritis.[10]
Aspirin is an important part of the treatment of those who have had a heart attack.[100] It is generally not recommended for routine use by people with no other health problems, including those over the age of 70.[101]
The 2009 Antithrombotic Trialists' Collaboration published in Lancet evaluated the efficacy and safety of low dose aspirin in secondary prevention. In those with prior ischaemic stroke or acute myocardial infarction, daily low dose aspirin was associated with a 19% relative risk reduction of serious cardiovascular events (non-fatal myocardial infarction, non-fatal stroke, or vascular death). This did come at the expense of a 0.19% absolute risk increase in gastrointestinal bleeding; however, the benefits outweigh the hazard risk in this case.[citation needed] Data from previous trials have suggested that weight-based dosing of aspirin has greater benefits in primary prevention of cardiovascular outcomes.[102] However, more recent trials were not able to replicate similar outcomes using low dose aspirin in low body weight (<70 kg) in specific subset of population studied i.e. elderly and diabetic population, and more evidence is required to study the effect of high dose aspirin in high body weight (≥70 kg).[103][104][105]
After percutaneous coronary interventions (PCIs), such as the placement of a coronary artery stent, a U.S. Agency for Healthcare Research and Quality guideline recommends that aspirin be taken indefinitely.[106] Frequently, aspirin is combined with an ADP receptor inhibitor, such as clopidogrel, prasugrel, or ticagrelor to prevent blood clots. This is called dual antiplatelet therapy (DAPT). Duration of DAPT was advised in the United States and European Union guidelines after the CURE[107] and PRODIGY[108] studies. In 2020, the systematic review and network meta-analysis from Khan et al.[109] showed promising benefits of short-term (< 6 months) DAPT followed by P2Y12 inhibitors in selected patients, as well as the benefits of extended-term (> 12 months) DAPT in high risk patients. In conclusion, the optimal duration of DAPT after PCIs should be personalized after outweighing each patient's risks of ischemic events and risks of bleeding events with consideration of multiple patient-related and procedure-related factors. Moreover, aspirin should be continued indefinitely after DAPT is complete.[110][111][112]
The status of the use of aspirin for the primary prevention in cardiovascular disease is conflicting and inconsistent, with recent changes from previously recommending it widely decades ago, and that some referenced newer trials in clinical guidelines show less of benefit of adding aspirin alongside other anti-hypertensive and cholesterol lowering therapies.[101][113] The ASCEND study demonstrated that in high-bleeding risk diabetics with no prior cardiovascular disease, there is no overall clinical benefit (12% decrease in risk of ischaemic events v/s 29% increase in GI bleeding) of low dose aspirin in preventing the serious vascular events over a period of 7.4 years. Similarly, the results of the ARRIVE study also showed no benefit of same dose of aspirin in reducing the time to first cardiovascular outcome in patients with moderate risk of cardiovascular disease over a period of five years. Aspirin has also been suggested as a component of a polypill for prevention of cardiovascular disease.[114][115] Complicating the use of aspirin for prevention is the phenomenon of aspirin resistance.[116][117] For people who are resistant, aspirin's efficacy is reduced.[118] Some authors have suggested testing regimens to identify people who are resistant to aspirin.[119]
As of April 2022[update], the United States Preventive Services Task Force (USPSTF) determined that there was a "small net benefit" for patients aged 40–59 with a 10% or greater 10-year cardiovascular disease (CVD) risk, and "no net benefit" for patients aged over 60.[120][121][122] Determining the net benefit was based on balancing the risk reduction of taking aspirin for heart attacks and ischaemic strokes, with the increased risk of gastrointestinal bleeding, intracranial bleeding, and hemorrhagic strokes. Their recommendations state that age changes the risk of the medicine, with the magnitude of the benefit of aspirin coming from starting at a younger age, while the risk of bleeding, while small, increases with age, particular for adults over 60, and can be compounded by other risk factors such as diabetes and a history of gastrointestinal bleeding. As a result, the USPSTF suggests that "people ages 40 to 59 who are at higher risk for CVD should decide with their clinician whether to start taking aspirin; people 60 or older should not start taking aspirin to prevent a first heart attack or stroke." Primary prevention guidelines from September 2019[update] made by the American College of Cardiology and the American Heart Association state they might consider aspirin for patients aged 40–69 with a higher risk of atherosclerotic CVD, without an increased bleeding risk, while stating they would not recommend aspirin for patients aged over 70 or adults of any age with an increased bleeding risk.[101] They state a CVD risk estimation and a risk discussion should be done before starting on aspirin, while stating aspirin should be used "infrequently in the routine primary prevention of (atherosclerotic CVD) because of lack of net benefit". As of August 2021[update], the European Society of Cardiology made similar recommendations; considering aspirin specifically to patients aged less than 70 at high or very high CVD risk, without any clear contraindications, on a case-by-case basis considering both ischemic risk and bleeding risk.[113]
Aspirin may reduce the overall risk of both getting cancer and dying from cancer.[123] There is substantial evidence for lowering the risk of colorectal cancer (CRC),[84][124][125][126] but aspirin must be taken for at least 10–20 years to see this benefit.[127] It may also slightly reduce the risk of endometrial cancer[128] and prostate cancer.[129]
Some conclude the benefits are greater than the risks due to bleeding in those at average risk.[123] Others are unclear if the benefits are greater than the risk.[130][131] Given this uncertainty, the 2007 United States Preventive Services Task Force (USPSTF) guidelines on this topic recommended against the use of aspirin for prevention of CRC in people with average risk.[132] Nine years later however, the USPSTF issued a grade B recommendation for the use of low-dose aspirin (75 to 100 mg/day) "for the primary prevention of CVD [cardiovascular disease] and CRC in adults 50 to 59 years of age who have a 10% or greater 10-year CVD risk, are not at increased risk for bleeding, have a life expectancy of at least 10 years, and are willing to take low-dose aspirin daily for at least 10 years".[133]
A meta-analysis through 2019 said that there was an association between taking aspirin and lower risk of cancer of the colorectum, esophagus, and stomach.[134]
In 2021, the U.S. Preventive services Task Force raised questions about the use of aspirin in cancer prevention. It notes the results of the 2018 ASPREE (Aspirin in Reducing Events in the Elderly) Trial, in which the risk of cancer-related death was higher in the aspirin-treated group than in the placebo group.[135]
Aspirin, along with several other agents with anti-inflammatory properties, has been repurposed as an add-on treatment for depressive episodes in subjects with bipolar disorder in light of the possible role of inflammation in the pathogenesis of severe mental disorders.[136] A 2022 systematic review concluded that aspirin exposure reduced the risk of depression in a pooled cohort of three studies (HR 0.624, 95% CI: 0.0503, 1.198, P=0.033). However, further high-quality, longer-duration, double-blind randomized controlled trials (RCTs) are needed to determine whether aspirin is an effective add-on treatment for bipolar depression.[137][138][139] Thus, notwithstanding the biological rationale, the clinical perspectives of aspirin and anti-inflammatory agents in the treatment of bipolar depression remain uncertain.[136]
Although cohort and longitudinal studies have shown low-dose aspirin has a greater likelihood of reducing the incidence of dementia, numerous randomized controlled trials have not validated this.[140][141]
Some researchers have speculated the anti-inflammatory effects of aspirin may be beneficial for schizophrenia. Small trials have been conducted but evidence remains lacking.[142][143]
Aspirin is a first-line treatment for the fever and joint-pain symptoms of acute rheumatic fever. The therapy often lasts for one to two weeks, and is rarely indicated for longer periods. After fever and pain have subsided, the aspirin is no longer necessary, since it does not decrease the incidence of heart complications and residual rheumatic heart disease.[144][145] Naproxen has been shown to be as effective as aspirin and less toxic, but due to the limited clinical experience, naproxen is recommended only as a second-line treatment.[144][146]
Along with rheumatic fever, Kawasaki disease remains one of the few indications for aspirin use in children[147] in spite of a lack of high quality evidence for its effectiveness.[148]
Low-dose aspirin supplementation has moderate benefits when used for prevention of pre-eclampsia.[149][150] This benefit is greater when started in early pregnancy.[151]
Aspirin has also demonstrated anti-tumoral effects, via inhibition of the PTTG1 gene, which is often overexpressed in tumors.[152]
For some people, aspirin does not have as strong an effect on platelets as for others, an effect known as aspirin-resistance or insensitivity. One study has suggested women are more likely to be resistant than men,[153] and a different, aggregate study of 2,930 people found 28% were resistant.[154] A study in 100 Italian people found, of the apparent 31% aspirin-resistant subjects, only 5% were truly resistant, and the others were noncompliant.[155] Another study of 400 healthy volunteers found no subjects who were truly resistant, but some had "pseudoresistance, reflecting delayed and reduced drug absorption". [156]
Meta-analysis and systematic reviews have concluded that laboratory confirmed aspirin resistance confers increased rates of poorer outcomes in cardiovascular and neurovascular diseases.[157][154][158][159][160][161] Although the majority of research conducted has surrounded cardiovascular and neurovascular, there is emerging research into the risk of aspirin resistance after orthopaedic surgery where aspirin is used for venous thromboembolism prophylaxis.[162] Aspirin resistance in orthopaedic surgery, specifically after total hip and knee arthroplasties, is of interest as risk factors for aspirin resistance are also risk factors for venous thromboembolisms and osteoarthritis; the sequelae of requiring a total hip or knee arthroplasty. Some of these risk factors include obesity, advancing age, diabetes mellitus, dyslipidemia and inflammatory diseases.[162]
Adult aspirin tablets are produced in standardised sizes, which vary slightly from country to country, for example 300 mg in Britain and 325 mg in the United States. Smaller doses are based on these standards, e.g., 75 mg and 81 mg tablets. The 81 mg tablets are commonly called "baby aspirin" or "baby-strength", because they were originally – but no longer – intended to be administered to infants and children.[163] No medical significance occurs due to the slight difference in dosage between the 75 mg and the 81 mg tablets. The dose required for benefit appears to depend on a person's weight.[102] For those weighing less than 70 kilograms (154 lb), low dose is effective for preventing cardiovascular disease; for patients above this weight, higher doses are required.[102]
In general, for adults, doses are taken four times a day for fever or arthritis,[164] with doses near the maximal daily dose used historically for the treatment of rheumatic fever.[165] For the prevention of myocardial infarction (MI) in someone with documented or suspected coronary artery disease, much lower doses are taken once daily.[164]
March 2009 recommendations from the USPSTF on the use of aspirin for the primary prevention of coronary heart disease encourage men aged 45–79 and women aged 55–79 to use aspirin when the potential benefit of a reduction in MI for men or stroke for women outweighs the potential harm of an increase in gastrointestinal hemorrhage.[166][167][needs update] The WHI study of postmenopausal women found that aspirin resulted in a 25% lower risk of death from cardiovascular disease and a 14% lower risk of death from any cause, though there was no significant difference between 81 mg and 325 mg aspirin doses.[168] The 2021 ADAPTABLE study also showed no significant difference in cardiovascular events or major bleeding between 81 mg and 325 mg doses of aspirin in patients (both men and women) with established cardiovascular disease.[169]
Low-dose aspirin use was also associated with a trend toward lower risk of cardiovascular events, and lower aspirin doses (75 or 81 mg/day) may optimize efficacy and safety for people requiring aspirin for long-term prevention.[167]
In children with Kawasaki disease, aspirin is taken at dosages based on body weight, initially four times a day for up to two weeks and then at a lower dose once daily for a further six to eight weeks.[170]
In October 2020, the US Food and Drug Administration (FDA) required the drug label to be updated for all nonsteroidal anti-inflammatory medications to describe the risk of kidney problems in unborn babies that result in low amniotic fluid.[171][172] They recommend avoiding NSAIDs in pregnant women at 20 weeks or later in pregnancy.[171][172] One exception to the recommendation is the use of low-dose 81 mg aspirin at any point in pregnancy under the direction of a health care professional.[172]
Aspirin should not be taken by people who are allergic to ibuprofenornaproxen,[173][174] or who have salicylate intolerance[175][176] or a more generalized drug intolerance to NSAIDs, and caution should be exercised in those with asthma or NSAID-precipitated bronchospasm. Owing to its effect on the stomach lining, manufacturers recommend people with peptic ulcers, mild diabetes, or gastritis seek medical advice before using aspirin.[173][177] Even if none of these conditions is present, the risk of stomach bleeding is still increased when aspirin is taken with alcoholorwarfarin.[173][174] People with hemophilia or other bleeding tendencies should not take aspirin or other salicylates.[173][177] Aspirin is known to cause hemolytic anemia in people who have the genetic disease glucose-6-phosphate dehydrogenase deficiency, particularly in large doses and depending on the severity of the disease.[178] Use of aspirin during dengue fever is not recommended owing to increased bleeding tendency.[179] Aspirin taken at doses of ≤325 mg and ≤100 mg per day for ≥2 days can increase the odds of suffering a gout attack by 81% and 91% respectively. This effect may potentially be worsened by high purine diets, diuretics, and kidney disease, but is eliminated by the urate lowering drug allopurinol.[180] Daily low dose aspirin does not appear to worsen kidney function.[181] Aspirin may reduce cardiovascular risk in those without established cardiovascular disease in people with moderate CKD, without significantly increasing the risk of bleeding.[182] Aspirin should not be given to children or adolescents under the age of 16 to control cold or influenza symptoms, as this has been linked with Reye's syndrome.[183]
Aspirin increases the risk of upper gastrointestinal bleeding.[184] Enteric coating on aspirin may be used in manufacturing to prevent release of aspirin into the stomach to reduce gastric harm, but enteric coating does not reduce gastrointestinal bleeding risk.[184][185] Enteric-coated aspirin may not be as effective at reducing blood clot risk.[186][187] Combining aspirin with other NSAIDs has been shown to further increase the risk of gastrointestinal bleeding.[184] Using aspirin in combination with clopidogrel or warfarin also increases the risk of upper gastrointestinal bleeding.[188]
Blockade of COX-1 by aspirin apparently results in the upregulation of COX-2 as part of a gastric defense.[189] There is no clear evidence that simultaneous use of a COX-2 inhibitor with aspirin may increase the risk of gastrointestinal injury.[190]
"Buffering" is an additional method used with the intent to mitigate gastrointestinal bleeding, such as by preventing aspirin from concentrating in the walls of the stomach, although the benefits of buffered aspirin are disputed.[191] Almost any buffering agent used in antacids can be used; Bufferin, for example, uses magnesium oxide. Other preparations use calcium carbonate.[192] Gas-forming agents in effervescent tablet and powder formulations can also double as a buffering agent, one example being sodium bicarbonate, used in Alka-Seltzer.[193]
Taking vitamin C with aspirin has been investigated as a method of protecting the stomach lining. In trials vitamin C-releasing aspirin (ASA-VitC) or a buffered aspirin formulation containing vitamin C was found to cause less stomach damage than aspirin alone.[194][195]
It is a widespread habit among eye specialists (ophthalmologists) to prescribe aspirin as an add-on medication for patients with retinal vein occlusion (RVO), such as central retinal vein occlusion (CRVO) and branch retinal vein occlusion (BRVO). The reason of this widespread use is the evidence of its proven effectiveness in major systemic venous thrombotic disorders, and it has been assumed that may be similarly beneficial in various types of retinal vein occlusion.
However, a large-scale investigation based on data of nearly 700 patients showed "that aspirin or other antiplatelet aggregating agents or anticoagulants adversely influence the visual outcome in patients with CRVO and hemi-CRVO, without any evidence of protective or beneficial effect".[196] Several expert groups, including the Royal College of Ophthalmologists, recommended against the use of antithrombotic drugs (incl. aspirin) for patients with RVO.[197]
Large doses of salicylate, a metabolite of aspirin, cause temporary tinnitus (ringing in the ears) based on experiments in rats, via the action on arachidonic acid and NMDA receptors cascade.[198]
Reye's syndrome, a rare but severe illness characterized by acute encephalopathy and fatty liver, can occur when children or adolescents are given aspirin for a fever or other illness or infection. From 1981 to 1997, 1207 cases of Reye's syndrome in people younger than 18 were reported to the US Centers for Disease Control and Prevention (CDC). Of these, 93% reported being ill in the three weeks preceding the onset of Reye's syndrome, most commonly with a respiratory infection, chickenpox, or diarrhea. Salicylates were detectable in 81.9% of children for whom test results were reported.[199] After the association between Reye's syndrome and aspirin was reported, and safety measures to prevent it (including a Surgeon General's warning, and changes to the labeling of aspirin-containing drugs) were implemented, aspirin taken by children declined considerably in the United States, as did the number of reported cases of Reye's syndrome; a similar decline was found in the United Kingdom after warnings against pediatric aspirin use were issued.[199] The US Food and Drug Administration recommends aspirin (or aspirin-containing products) should not be given to anyone under the age of 12 who has a fever,[183] and the UK National Health Service recommends children who are under 16 years of age should not take aspirin, unless it is on the advice of a doctor.[200]
For a small number of people, taking aspirin can result in symptoms including hives, swelling, and headache.[201] Aspirin can exacerbate symptoms among those with chronic hives, or create acute symptoms of hives.[202] These responses can be due to allergic reactions to aspirin, or more often due to its effect of inhibiting the COX-1 enzyme.[202][203] Skin reactions may also tie to systemic contraindications, seen with NSAID-precipitated bronchospasm,[202][203] or those with atopy.[204]
Aspirin and other NSAIDs, such as ibuprofen, may delay the healing of skin wounds.[205] Earlier findings from two small, low-quality trials suggested a benefit with aspirin (alongside compression therapy) on venous leg ulcer healing time and leg ulcer size,[206][207][208] however larger, more recent studies of higher quality have been unable to corroborate these outcomes.[209][210] As such, further research is required to clarify the role of aspirin in this context.
Aspirin can induce swelling of skin tissues in some people. In one study, angioedema appeared one to six hours after ingesting aspirin in some of the people. However, when the aspirin was taken alone, it did not cause angioedema in these people; the aspirin had been taken in combination with another NSAID-induced drug when angioedema appeared.[211]
Aspirin causes an increased risk of cerebral microbleeds, having the appearance on MRI scans of 5 to 10 mm or smaller, hypointense (dark holes) patches.[212][213]
A study of a group with a mean dosage of aspirin of 270 mg per day estimated an average absolute risk increase in intracerebral hemorrhage (ICH) of 12 events per 10,000 persons.[214] In comparison, the estimated absolute risk reduction in myocardial infarction was 137 events per 10,000 persons, and a reduction of 39 events per 10,000 persons in ischemic stroke.[214] In cases where ICH already has occurred, aspirin use results in higher mortality, with a dose of about 250 mg per day resulting in a relative risk of death within three months after the ICH around 2.5 (95% confidence interval 1.3 to 4.6).[215]
Aspirin and other NSAIDs can cause abnormally high blood levels of potassium by inducing a hyporeninemic hypoaldosteronism state via inhibition of prostaglandin synthesis; however, these agents do not typically cause hyperkalemia by themselves in the setting of normal renal function and euvolemic state.[216]
Use of low-dose aspirin before a surgical procedure has been associated with an increased risk of bleeding events in some patients, however, ceasing aspirin prior to surgery has also been associated with an increase in major adverse cardiac events. An analysis of multiple studies found a three-fold increase in adverse events such as myocardial infarction in patients who ceased aspirin prior to surgery. The analysis found that the risk is dependent on the type of surgery being performed and the patient indication for aspirin use.[217]
On 9 July 2015, the US Food and Drug Administration (FDA) toughened warnings of increased heart attack and stroke risk associated with nonsteroidal anti-inflammatory drugs (NSAID).[218] Aspirin is an NSAID but is not affected by the new warnings.[218]
Aspirin overdose can be acute or chronic. In acute poisoning, a single large dose is taken; in chronic poisoning, higher than normal doses are taken over a period of time. Acute overdose has a mortality rate of 2%. Chronic overdose is more commonly lethal, with a mortality rate of 25%;[219] chronic overdose may be especially severe in children.[220] Toxicity is managed with a number of potential treatments, including activated charcoal, intravenous dextrose and normal saline, sodium bicarbonate, and dialysis.[221] The diagnosis of poisoning usually involves measurement of plasma salicylate, the active metabolite of aspirin, by automated spectrophotometric methods. Plasma salicylate levels in general range from 30 to 100 mg/L after usual therapeutic doses, 50–300 mg/L in people taking high doses and 700–1400 mg/L following acute overdose. Salicylate is also produced as a result of exposure to bismuth subsalicylate, methyl salicylate, and sodium salicylate.[222][223]
Aspirin is known to interact with other drugs. For example, acetazolamide and ammonium chloride are known to enhance the intoxicating effect of salicylates, and alcohol also increases the gastrointestinal bleeding associated with these types of drugs.[173][174] Aspirin is known to displace a number of drugs from protein-binding sites in the blood, including the antidiabetic drugs tolbutamide and chlorpropamide, warfarin, methotrexate, phenytoin, probenecid, valproic acid (as well as interfering with beta oxidation, an important part of valproate metabolism), and other NSAIDs. Corticosteroids may also reduce the concentration of aspirin. Other NSAIDs, such as ibuprofen and naproxen, may reduce the antiplatelet effect of aspirin.[224][225] Although limited evidence suggests this may not result in a reduced cardioprotective effect of aspirin.[224] Analgesic doses of aspirin decrease sodium loss induced by spironolactone in the urine, however this does not reduce the antihypertensive effects of spironolactone.[226] Furthermore, antiplatelet doses of aspirin are deemed too small to produce an interaction with spironolactone.[227] Aspirin is known to compete with penicillin G for renal tubular secretion.[228] Aspirin may also inhibit the absorption of vitamin C.[229][230][unreliable medical source?][231]
The ISIS-2 trial demonstrated that aspirin at doses of 160 mg daily for one month, decreased the mortality by 21% of participants with a suspected myocardial infarction in the first five weeks.[232] A single daily dose of 324 mg of aspirin for 12 weeks has a highly protective effect against acute myocardial infarction and death in men with unstable angina.[233]
Aspirin has been repurposed as an add-on treatment for depressive episodes in subjects with bipolar disorder.[136] However, meta-analytic evidence is based on very few studies and does not suggest any efficacy of aspirin in the treatment of bipolar depression.[136] Thus, notwithstanding the biological rationale, the clinical perspectives of aspirin and anti-inflammatory agents in the treatment of bipolar depression remain uncertain.[136]
Several studies investigated the anti-infective properties of aspirin for bacterial, viral and parasitic infections. Aspirin was demonstrated to limit platelet activation induced by Staphylococcus aureus and Enterococcus faecalis and to reduce streptococcal adhesion to heart valves. In patients with tuberculous meningitis, the addition of aspirin reduced the risk of new cerebral infarction [RR = 0.52 (0.29-0.92)]. A role of aspirin on bacterial and fungal biofilm is also being supported by growing evidence.[234]
Evidence from observational studies were conflicting on the effect of aspirin in breast cancer prevention,[235] a randomized controlled trial showed that aspirin had no significant effect in reducing breast cancer [236] thus further studies are needed to clarify aspirin effect in cancer prevention.
There are many anecdotal reportings that aspirin can improve plant's growth and resistance[237][238] though most research involved salicylic acid instead of aspirin.[239]
Aspirin is sometimes used in veterinary medicine as an anticoagulant or to relieve pain associated with musculoskeletal inflammation or osteoarthritis. Aspirin should only be given to animals under the direct supervision of a veterinarian, as adverse effects—including gastrointestinal issues—are common. An aspirin overdose in any species may result in salicylate poisoning, characterized by hemorrhaging, seizures, coma, and even death.[240]
Dogs are better able to tolerate aspirin than cats are.[241] Cats metabolize aspirin slowly because they lack the glucuronide conjugates that aid in the excretion of aspirin, making it potentially toxic if dosing is not spaced out properly.[240][242] No clinical signs of toxicosis occurred when cats were given 25 mg/kg of aspirin every 48 hours for 4 weeks,[241] but the recommended dose for relief of pain and fever and for treating blood clotting diseases in cats is 10 mg/kg every 48 hours to allow for metabolization.[240][243]
...there was postprandial reduction on the plasma concentration of IL-6 and IkBα preservation, followed by the lower activation of NFκB, considered the main transcription factor capable of inducing inflammatory response by stimulating the expression of proinflammatory cytokines, chemokines, and adhesion molecules.
The present comprehensive meta-analysis supports and further quantifies the inverse association between regular aspirin use and the risk of colorectal and other digestive tract cancers, including some rare ones. The favorable effect of aspirin increases with longer duration of use, and, for colorectal cancer, with increasing dose.
|
| |
|---|---|
|
|
| |||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Receptor (ligands) |
| ||||||||||||||||||||||||||
| Enzyme (inhibitors) |
| ||||||||||||||||||||||||||
| Others |
| ||||||||||||||||||||||||||
| |||||||||||||||||||||||||||